In clinical practice, there are very few infections that genuinely worry us because of how fast they can change a patient’s condition. Meningococcal disease is one of them.
According to the World Health Organization, bacterial meningitis can become fatal within 24 hours, even with previously healthy individuals.
The global burden is still significant, with around 240,000 deaths annually and millions affected worldwide. (World Health Organization 2025)
Recent real-world data continues to reinforce this concern.
In 2026, a meningococcal outbreak among university students led to multiple deaths and severe illness within days, highlighting how rapidly the disease spreads in close-contact environments.
As a physiotherapist, my concern is not just survival. It is what happens after the patient leaves the hospital.
Read about : What is Cervical Facet Joint Pain, how it causes cervicogenic headaches and how to correct it naturally
Meningococcal disease is a fast-progressing bacterial infection that can become life-threatening within 24 hours. Even after survival, many patients experience long-term complications such as fatigue, weakness, and neurological issues. Physiotherapy plays a key role in restoring strength, balance, and independence during recovery.
Read: Eagle Syndrome: Hidden Cause of Neck, Ear and Throat Pain
- Meningococcal disease can become severe within hours and requires urgent medical care.
- Up to 20–40% of survivors may develop long-term physical or neurological complications.
- Fatigue and reduced endurance are common but often underestimated.
- Physiotherapy helps restore mobility, coordination, and daily function.
- Recovery is gradual and requires structured rehabilitation and patience.
- Vaccination remains the most effective method of prevention.
Read: How to Reduce Tinnitus Naturally
A Real Patient Scenario I Still Remember
A few months ago, I worked with a 19-year-old college student who initially thought he had a viral fever.
Within a day, his condition worsened, and he was admitted to the ICU with meningococcal infection.
When he came to physiotherapy, he could barely sit unsupported. What stood out was not just the weakness, but the frustration.
He kept saying, “I was completely fine two days ago.”
Over the next few weeks, we worked on basic movements, balance, and gradually walking again.
But the bigger challenge was his fatigue. Even small activities drained him.
This is something I see often. Recovery is not just physical. It is emotional and unpredictable.
Read: Cervicocephalic Syndrome: Simple Exercises For Neck Related Headaches
What Is Meningococcal Disease and Why It Becomes Severe So Quickly
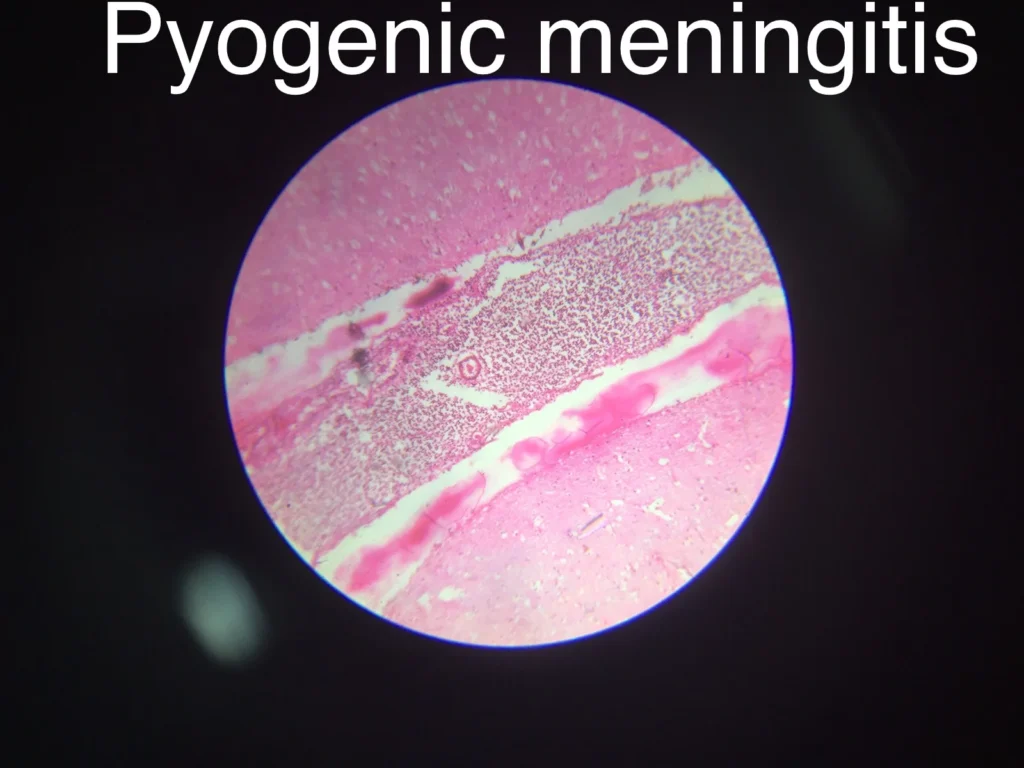
Meningococcal disease is caused by Neisseria meningitidis, a bacterium that lives in the nose and throat of many people without causing symptoms.
In some individuals, it invades the bloodstream and brain, leading to meningitis or septicemia.
The danger lies in how the body reacts:
- Rapid inflammatory response
- Blood vessel damage
- Impaired circulation
- Brain swelling
These changes explain why symptoms escalate so quickly and why complications can affect multiple systems. (World Health Organization EMRO 2024)
Read: The Morning Headache Causes and Easy Fixes
What Makes Meningococcal Disease Different from Other Infections
Many infections start with similar symptoms, which is why meningococcal disease is often mistaken for a common viral illness in the early stage.
What makes it different is how quickly it escalates.
Unlike most infections that worsen gradually, meningococcal disease can change a patient’s condition within hours.
A person may feel mildly unwell in the morning and become critically ill by evening.
Another important difference is the involvement of multiple systems at once.
It does not just affect the brain. It also impacts blood circulation, which can lead to skin changes, organ stress, and in severe cases, tissue damage.
This combination of rapid progression and multi-system involvement is what makes early recognition so important.
Also Read: Neck Pain with Fever: When To Worry And How To Treat
Early Symptoms That Are Often Ignored
One of the biggest clinical challenges is that early symptoms look harmless.
Patients often report:
At this stage, many assume it is a viral infection.
However, this phase is critical. Once neurological symptoms appear such as confusion, neck stiffness, or sensitivity to light, the disease has already progressed significantly.
Read: How to Fix Neck Fatigue After Migraine Naturally
Early Warning Signs vs Late Danger Signs
Understanding the difference can help you act faster.
Early signs
- Mild fever
- Headache
- Fatigue
- Body aches
- Nausea
Late or emergency signs
- Neck stiffness
- Confusion or drowsiness
- Sensitivity to light
- Seizures
- Rash that does not fade on pressure
If late signs appear, it is already an emergency.
Read more: Cervical Vertigo Explained: Why Neck Pain Make You Feel Dizzy
How Fast It Can Deteriorate
This is not a gradual illness.
Clinical progression may include:
- Sudden drop in blood pressure
- Altered consciousness
- Seizures
- Non-blanching rash
Fatality rates remain around 10 to 15 percent even with treatment, and complications are common. (WHO EMRO 2024)
Read: How to Manage Migraine Naturally and Effectively
What Happens After Survival
This is the part that is often underexplored.
Around 20 percent of survivors develop long-term complications that affect their daily life. (World Health Organization 2025)
A 2025 research review further shows that up to 20 to 40 percent of survivors may experience disabling long-term effects. (Christensen et al. 2025)
Also Read: Sore Throat and Stiff Neck: When to Worry
The Hidden Long-Term Effects
Physical complications
- Muscle weakness
- Joint stiffness
- Reduced mobility
- Limb loss in severe cases
Long-term complications can include hearing loss, seizures, skin damage, and amputations due to vascular compromise. (National Vaccine Information Center 2024)
Neurological complications
- Memory issues
- Poor coordination
- Slowed reaction time
- Balance problems
Psychological and cognitive impact
This is where newer research adds important insight.
Nearly 60 percent of adolescent survivors experience long-term psychological issues including anxiety, reduced quality of life, and cognitive difficulties. (Marshall et al. 2025)
Read : How to Treat Neck Pain in Ankylosing Spondylitis
Daily Life Challenges Patients Often Face
Even after discharge, many patients struggle with everyday activities.
Common issues include:
- Difficulty concentrating at work or studies
- Feeling exhausted after simple tasks
- Fear of falling due to poor balance
- Reduced confidence in physical activity
These challenges are often misunderstood because they are not always visible.
Also Read: Neck Pain When Coughing: Causes, Relief, and When to Worry
A Physiotherapist’s Perspective on Recovery
From my clinical experience, recovery is not just about regaining strength.
It is about restoring function, confidence, and independence.
Read: Lhermitte’s sign- An Electic Shock Sensation Down The Neck
Phase-Based Rehabilitation Approach
Phase 1: Early Recovery
Focus is on:
- Preventing muscle loss
- Restoring basic movement
Interventions include:
- Bed mobility exercises
- Assisted sitting and standing
- Gentle breathing work
Phase 2: Functional Independence
Patients begin relearning daily movements:
- Sit-to-stand training
- Walking practice
- Balance exercises
At this stage, fatigue becomes noticeable.
Phase 3: Neurological Rehabilitation
This phase is often underestimated.
- Coordination training
- Proprioception exercises
- Dual-task activities
These help restore brain-body connection.
Phase 4: Fatigue and Energy Management
This is one of the most important yet overlooked components.
Patients often report:
- Sudden exhaustion
- Reduced endurance
- Difficulty sustaining activity
Rehabilitation includes:
- Activity pacing
- Structured rest intervals
- Gradual workload progression
Common Mistakes I See During Recovery
- Trying to return to normal activity too quickly
- Ignoring fatigue signals
- Skipping rehabilitation exercises
- Comparing recovery with others
Recovery after meningococcal disease is individual. Pushing too hard can delay progress.
Read about: Effective Neck Pain Exercises At Home: A Complete Guide to Relief and Improved Mobility
A Simple Home Exercise Routine I Recommend
Start only after medical clearance.
1. Sit to stand
Repeat 8 to 10 times
Helps improve leg strength
2. Heel raises
Hold a support and lift heels
Repeat 10 times
3. Single leg balance
Hold for 10 seconds each side
4. Deep breathing
5 slow breaths, 3 times daily
5. Short walks
Start with 5 minutes and increase gradually
Consistency matters more than intensity.
Also Read: Ultimate 6 Weeks Neck Rehabilitation Exercises For Pain Relief
Recovery Timeline: What You Should Realistically Expect
Recovery is not the same for everyone, but a general pattern looks like this:
First 2 weeks
- Severe weakness
- Limited mobility
- High fatigue
2 to 6 weeks
- Gradual improvement in movement
- Better balance
- Fatigue still present
2 to 3 months
- Functional independence improves
- Endurance still reduced
3 to 6 months
- Most daily activities resume
- Some fatigue and cognitive issues may persist
Some patients take longer, especially if complications were severe.
Read: Spasm In Neck: What Causes It & How to Fix It Fast
Red Flags During Recovery That Should Not Be Ignored
Recovery is usually gradual, but there are certain signs that should prompt immediate medical attention.
Watch for the following:
- Sudden worsening of headache
- New onset confusion or memory problems
- Persistent vomiting
- Increased difficulty in walking or balance
- Severe fatigue that does not improve with rest
- Any new seizures or unusual movements
These symptoms may indicate complications or delayed effects of the infection.
If any of these appear, it is important not to wait or self-manage. Early medical review can prevent further deterioration.
Also Read : Neck Cracking: Benefits, Risks, and the Truth About Stroke
Lesser Known Clinical Insights
The disease is partly vascular
Many complications arise due to blood vessel damage, not just infection.
Survivors may look normal but struggle functionally
Especially with endurance and cognition.
Adolescents are a high-risk group
Due to close contact behaviors and lower perceived risk. (Christensen et al. 2025)
Read : Chiropractic for Neck Pain: Does It Really Work?
Who Is at Higher Risk
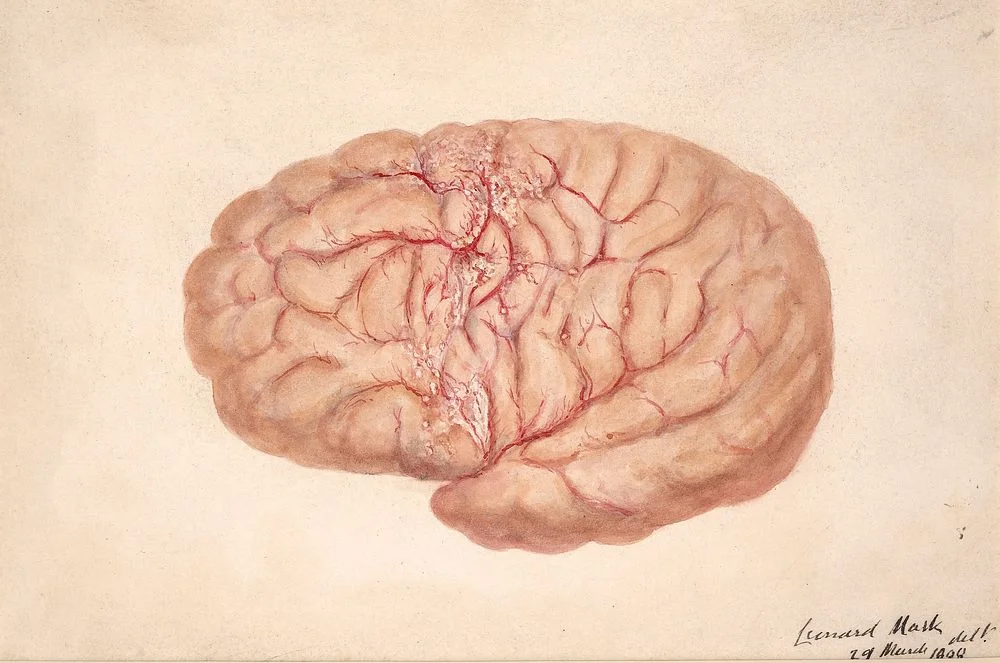
Some groups are more vulnerable:
- Infants and young children
- Teenagers and college students
- People living in shared spaces
- Individuals with weakened immunity
Awareness in these groups is especially important.
Neck Pain in Students: The Hidden Study Habit Destroying Your Spine
Prevention Still Matters
Vaccination remains the most effective protection.
Vaccines target major strains including A, B, C, W, and Y.
Recent trends show cases rising again post-pandemic, emphasizing the importance of immunization and awareness. (CDC 2025)
Read: Pain in the Back Side of the Neck: Causes and Treatment
When to Seek Immediate Medical Help
Act immediately if you notice:
- High fever with confusion
- Neck stiffness
- Rash that does not fade
- Drowsiness or seizures
This disease does not allow delays.
Read about: How to Relieve Morning Neck Stiffness Naturally
When Can You Return to Work or Normal Life
This depends on recovery progress.
- Light activities may resume in a few weeks
- Full return to work may take 1 to 3 months
- Physically demanding work may take longer
A gradual return is always safer than rushing.
Also read: How to Relieve Neck Tightness Without Equipment
Final Thoughts from a Physiotherapist
Meningococcal disease is not just an acute infection.
It is a condition that can change a person’s physical and neurological function for months or even years.
Recovery is possible, but it requires:
- Early diagnosis
- Timely treatment
- Structured rehabilitation
- Long-term support
As clinicians, our role is not just to treat, but to help patients rebuild their lives.
Read more: Cervical Myelopathy: The Hidden Neck Condition Affecting Your Walking
Frequently Asked Questions
1. How quickly does meningococcal disease progress?
It can become life-threatening within 24 hours, which is why early recognition and treatment are critical.
2. What are the early symptoms to watch for?
Early symptoms include fever, headache, fatigue, body aches, and nausea, which can resemble a viral illness.
3. Can people fully recover from meningococcal disease?
Some individuals recover completely, but many experience long-term effects such as fatigue, weakness, or cognitive changes.
4. What long-term complications are common?
Common complications include hearing loss, balance issues, neurological deficits, and reduced physical endurance.
5. How does physiotherapy help in recovery?
Physiotherapy improves strength, coordination, balance, and helps patients regain independence in daily activities.
6. Is fatigue normal after recovery?
Yes, post-infection fatigue is very common and may persist for weeks or months.
7. Who is at higher risk of meningococcal disease?
Infants, adolescents, and people living in close-contact environments such as hostels or dormitories are at higher risk.
8. Can meningococcal disease be prevented?
Yes, vaccination is the most effective way to reduce the risk of infection.
Stay tuned with us for more health related topics.
Follow us on LinkedIn and Instagram for more.
Medical Disclaimer!
This article has been reviewed and written under the guidance of our Head Physiotherapist, Dr. Kruti Raj (PT, MUHS,CPT,CMPT). The information shared is intended for educational purposes only and should not be considered a substitute for personalized medical advice, diagnosis, or treatment.
Please consult us or any other qualified healthcare professional before beginning any exercise program, especially if you are experiencing pain, recovering from injury, or managing a medical condition.











