What Is Nuchal Translucency?
In early pregnancy, there is a small window where doctors try to gather as much information as possible about how the baby is developing.
One of the first structured screenings offered during this time is the nuchal translucency scan, usually done between 11 and 14 weeks.
Nuchal translucency refers to a thin layer of fluid that naturally collects at the back of the baby’s neck. Every fetus has this. It is not abnormal on its own.
What matters is the thickness of this fluid space.
From a clinical point of view, this measurement helps identify whether the baby may have a higher likelihood of certain chromosomal or structural conditions.
It is not a diagnosis. It is more like an early signal that helps guide the next step.
Read about: Early Signs of Cervical Spine Damage You Should Never Ignore
Quick Answer
Nuchal translucency is a fluid-filled space at the back of a baby’s neck measured between 11 and 14 weeks of pregnancy. It helps assess the risk of chromosomal conditions and certain structural abnormalities. A higher measurement does not confirm a problem but indicates the need for further evaluation through combined screening or diagnostic tests.
Read about our Complete Neck Pain Guide : Causes, Symptoms, Exercises and Treatment
Key Takeaways
- Nuchal translucency is an early screening tool, not a diagnosis.
- The scan is performed between 11 and 14 weeks of pregnancy.
- Higher NT values increase risk but do not confirm abnormalities.
- Combined screening improves accuracy significantly.
- Even with increased NT, many pregnancies result in healthy babies.
- Follow-up testing is essential for clarity and reassurance.
- Early detection supports better planning and intervention if needed.
Read about : 15 Common Causes of Neck Pain You Should Know
Why the NT Scan Is Still Relevant Today
Over the years, screening methods have evolved. Blood tests, genetic screening, and advanced imaging have improved accuracy.
Yet the NT scan still holds value because it gives a structural and physiological clue very early in pregnancy.
When combined with maternal blood markers and age, detection rates improve significantly.
Studies suggest that NT-based combined screening can detect up to 90 to 95 percent of Down syndrome cases when used appropriately. (Nicolaides et al., 2013)
What I find important in practice is that NT gives us an early direction, not a final answer. That distinction often reduces unnecessary anxiety when explained properly.
Read: What is Torticollis? How to treat neck tilt condition
When and How the Measurement Is Done
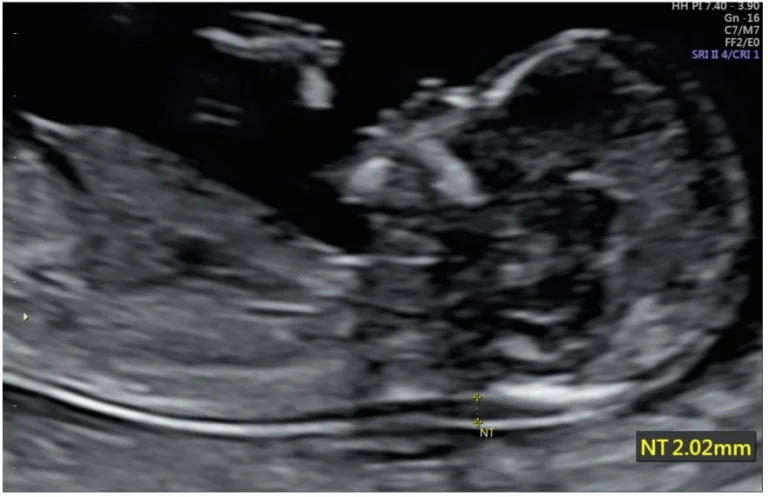
The scan is performed when the baby’s crown-rump length falls within a specific range.
This typically corresponds to 11 weeks to 13 weeks and 6 days.
During the scan:
- The baby must be in a neutral position
- The neck should not be overly flexed or extended
- The measurement is taken at the widest visible point of the fluid
Something not commonly discussed is how dependent this is on the person performing the scan.
A slight variation in angle or timing can change the reading.
This is why repeat scans are sometimes done if the image is not clear.
Read: What Causes Neck Pain in Children And How To Treat
What Is Considered Normal?
There is no single number that applies to all pregnancies. The measurement is interpreted relative to gestational age.
In general:
- Around 1.0 to 2.5 mm is commonly seen in low-risk cases
- Values above 3.5 mm are usually considered elevated
But here is where it gets more meaningful.
Instead of looking at normal versus abnormal, current practice looks at risk gradients.
Also Read : Neck Cracking: Benefits, Risks, and the Truth About Stroke
What NT Thickness Means in Real Terms
Recent data gives a clearer picture of how risk changes with increasing NT values.
- 2.5 to 2.9 mm shows a small rise in risk
- Around 3.5 mm begins to draw more attention
- 4 mm and above is associated with a significant increase in probability
In one large analysis, the risk of chromosomal abnormalities increased from about 4 percent at lower elevations to nearly 46 percent when NT exceeded 4 mm. (ScienceDirect, 2025)
In real clinical conversations, I often tell parents that the number itself is only part of the story. What matters more is what else is seen alongside it.
Read: How to Treat Trismus- A Jaw Stiffness Naturally with Exercises
What NT Report Does Not Tell You
One thing I often notice in practice is how much weight is placed on a single number in the report.
While the NT value is important, there are several things it does not capture.
- It does not show how the baby is functioning overall
A normal NT does not reflect neurological development, movement patterns, or future milestones. - It does not include dynamic changes
The scan is a snapshot taken at one moment. Fluid levels and fetal position can vary even within minutes. - It does not account for measurement variability
Even in experienced hands, small differences in angle or magnification can slightly change the reading. - It does not replace follow-up scans
A reassuring NT still needs to be followed by anomaly scans later in pregnancy.
In simple terms, the NT report gives direction, but not the full picture. Understanding this often helps reduce unnecessary worry or overconfidence.
Read: Branchial Cleft Cyst: A Complete Guide To Neck Lump
Why Increased NT Happens
From a physiological standpoint, increased NT is thought to be linked to:
- Temporary lymphatic drainage delay
- Subtle cardiac function differences
- Connective tissue variation
- Fluid redistribution patterns in early development
It is important to understand that these are mechanisms, not diagnoses.
In many cases, the fluid resolves as the pregnancy progresses.
Read: Understanding Dropped Head Syndrome in Simple Terms
When NT Is High but Everything Else Is Normal
This is one of the most important and reassuring areas of recent research.
If:
- NT is increased
- Detailed ultrasound is normal
- Genetic screening such as NIPT is low risk
Then about 96 percent of babies are born healthy. (ScienceDirect, 2025)
This is something that is often missed in general articles but makes a huge difference emotionally for parents.
Read: The Lemierre’s Syndrome: Rare Symptoms and Rehab Plan
The Link Between NT and Heart Development
A lesser-known but clinically important association is between increased NT and congenital heart conditions.
Even in babies with normal chromosomes:
- Higher NT measurements may be linked to cardiac abnormalities
Because of this, doctors may recommend a fetal echocardiogram later in pregnancy. (Frontiers in Medicine, 2025)
From a physiotherapy perspective, early identification of such risks helps in planning postnatal monitoring and developmental support.
Read: Understanding Swollen Lymph Nodes In The Neck
Does Increased NT Always Stay High?
Not necessarily.
A systematic review found that nearly half of the cases with increased NT showed resolution later in pregnancy.
However, there is an important nuance.
Even when NT resolves:
- Adverse outcomes were still observed in a significant number of cases
This tells us that resolution is reassuring but not definitive. (PubMed, 2024)
Also Read: Sore Throat and Stiff Neck: When to Worry
Why NT Alone Is No Longer Enough
Modern screening has shifted from single markers to combined assessment.
Today, NT is interpreted along with:
- Non-invasive prenatal testing
- Nasal bone assessment
- Blood flow patterns
- Maternal serum markers
This approach improves accuracy and reduces false positives.
In simple terms, NT is now one part of a bigger picture rather than a standalone decision tool.
Read: Lhermitte’s sign- An Electic Shock Sensation Down The Neck
Common Misunderstandings That Create Anxiety
There are a few patterns I repeatedly see in patients:
Assuming high NT equals confirmed abnormality
It does not. It only increases probability.
Believing normal NT guarantees everything is fine
It reduces risk but cannot rule out all conditions.
Searching too much online immediately after the report
This often leads to worst-case interpretations without context.
A balanced discussion with a healthcare provider is always more helpful than isolated reading.
Read about: What Is Military Neck Or Cervical Kyphosis And How To Treat It
The Emotional Side
Waiting for results after an NT scan can feel long and uncomfortable.
Even when the numbers are borderline, the uncertainty can be difficult to process.
In practice, what helps most is:
- Understanding that screening is stepwise
- Avoiding immediate conclusions
- Taking decisions only after complete evaluation
Many parents later say that the waiting period was more stressful than the outcome itself.
Read : How to Treat Neck Pain in Ankylosing Spondylitis
Physiotherapy Perspective on Early Screening
You may wonder how this connects to physiotherapy.
Early indicators like NT help identify babies who may need:
- Developmental monitoring
- Early intervention
- Postural or neuromotor support
The earlier we are aware, the better we can guide parents after birth.
This is not about predicting problems. It is about being prepared if support is needed.
Read about: Effective Neck Pain Exercises At Home: A Complete Guide to Relief and Improved Mobility
What Should You Do After the NT Scan?
A practical approach usually works best.
- Wait for combined screening results
- Follow your doctor’s advice regarding further tests
- Avoid comparing reports with others
- Focus on complete evaluation rather than a single number
Step-by-step clarity is always better than rushed conclusions.
Read about: What is Turkey Neck And How To Fix It Naturally
Questions You Should Ask After an NT Scan
After the scan, most people either feel relieved or anxious, but very few know what to ask next.
Having the right questions can make the conversation with your doctor much clearer.
1. Is this NT value concerning when combined with my blood test results?
The combined result matters more than NT alone.
2. Do I need additional screening like NIPT or a detailed scan?
This helps you understand the next step rather than guessing.
3. Was the baby in the correct position during measurement?
This can influence accuracy more than most people realize.
4. Should I plan a follow-up scan or fetal echocardiography?
Especially important if NT is on the higher side.
5. What is the actual risk percentage in my case?
Asking for numbers often gives better clarity than general terms like “high” or “low risk”.
These questions shift you from passive worrying to active understanding, which makes a big difference emotionally.
Read about: Neck And Jaw Pain Together? Here’s The Full Clinical Picture
Conclusion
Nuchal translucency is often one of the first structured checkpoints in pregnancy. It can feel overwhelming because it introduces uncertainty early on.
But from a clinical perspective, it is simply a tool that helps guide decisions.
It does not define the pregnancy. It informs it.
Most importantly, many pregnancies with borderline or even increased NT go on to have completely healthy outcomes.
Understanding the context, not just the number, makes all the difference.
Read about: How to Relieve Morning Neck Stiffness Naturally
Frequently Asked Questions
1. What is a normal nuchal translucency measurement?
A normal NT measurement typically ranges between 1.0 to 2.5 mm depending on gestational age and fetal size.
2. Does a high NT measurement always mean a problem?
No, it only indicates increased risk. Many babies with higher NT measurements are born healthy.
3. When is the NT scan done?
The NT scan is performed between 11 weeks and 13 weeks 6 days of pregnancy.
4. Is the NT scan safe?
Yes, it is a safe and non-invasive ultrasound procedure.
5. Can NT reduce later in pregnancy?
Yes, in some cases the fluid decreases as pregnancy progresses, but follow-up is still important.
6. What happens if NT is higher than normal?
Doctors may recommend additional tests such as NIPT, detailed ultrasound, or diagnostic procedures.
7. Is NT scan alone enough?
No, it is part of combined screening and should be interpreted with other tests.
Stay tuned with us for more health related topics.
Follow us on LinkedIn and Instagram for more.
Medical Disclaimer!
This article has been reviewed and written under the guidance of our Head Physiotherapist, Dr. Kruti Raj (PT, MUHS,CPT,CMPT). The information shared is intended for educational purposes only and should not be considered a substitute for personalized medical advice, diagnosis, or treatment.
Please consult us or any other qualified healthcare professional before beginning any exercise program, especially if you are experiencing pain, recovering from injury, or managing a medical condition.











