Swan neck deformity is more than just a visible finger abnormality. From a physiotherapy perspective, it represents a complex imbalance between tendons, ligaments, and joint mechanics.
Many patients assume it is purely a joint problem, but in reality, it is a dynamic failure of the hand’s biomechanical system.
As a physiotherapist, I often emphasize that early understanding and timely intervention can completely change outcomes.
This guide brings together recent research, clinical insights, and rehabilitation strategies to help you understand and manage this condition effectively.
Read about: Early Signs of Cervical Spine Damage You Should Never Ignore
Quick Answer
Swan neck deformity is a finger condition where the middle joint bends backward and the tip bends downward due to tendon imbalance. It is commonly caused by rheumatoid arthritis, injury, or ligament laxity. Early treatment with splinting and physiotherapy can often correct the deformity, while advanced cases may require surgery followed by rehabilitation.
Read about our Complete Neck Pain Guide : Causes, Symptoms, Exercises and Treatment
Key Takeaways
- Swan neck deformity is caused by imbalance between flexor and extensor tendons, not just joint damage.
- Early-stage deformities are often reversible with physiotherapy and splinting.
- Splints help control hyperextension but must be combined with targeted exercises.
- Delayed treatment can lead to permanent stiffness and functional loss.
- Rehabilitation plays a crucial role in both non-surgical and post-surgical recovery.
Read about: What Is Military Neck Or Cervical Kyphosis And How To Treat It
What is Swan Neck Deformity?
Swan neck deformity is defined by:
- Hyperextension of the proximal interphalangeal joint
- Flexion of the distal interphalangeal joint
This creates a curved appearance resembling a swan’s neck.
Unlike simple joint deformities, this condition reflects a loss of balance between flexor and extensor forces in the finger. Daniati et al. (2023)
Read: Lhermitte’s sign- An Electic Shock Sensation Down The Neck
Understanding the Biomechanics
To truly understand swan neck deformity, you need to look beyond the surface.
The key structures involved are:
- Extensor tendon mechanism
- Flexor tendons
- Volar plate
- Intrinsic hand muscles
When the volar plate becomes stretched or weakened, the proximal joint loses stability. At the same time, the extensor mechanism overpowers the system, pushing the joint into hyperextension.
This creates a chain reaction:
- PIP joint moves into hyperextension
- Lateral bands shift dorsally
- DIP joint compensates by flexing
- Grip strength and coordination decline StatPearls (2023)
Lesser known fact
Even a small untreated finger injury can gradually disrupt this balance and lead to deformity over time.
Read more: Cervical Myelopathy: The Hidden Neck Condition Affecting Your Walking
Classification of Swan Neck Deformity
From a physiotherapy standpoint, classification is critical because it determines treatment.
Flexible or Correctable Deformity
- Finger can be manually corrected
- No fixed joint stiffness
- Excellent response to physiotherapy and splinting
Fixed Deformity
- Joint stiffness present
- Structural changes in ligaments or joints
- Often requires surgical correction
Clinical insight
If the finger can still bend actively at the PIP joint, you are in the most treatable stage.
Read about: What is Turkey Neck And How To Fix It Naturally
How Swan Neck Deformity Progresses
Modern research shows that this condition develops in stages:
- Synovial inflammation or injury
- Ligament stretching especially the volar plate
- Tendon imbalance develops
- Joint instability increases
- Fixed deformity may occur
Early intervention can interrupt this entire cascade. Hamada et al. (2024)
Read about : 15 Common Causes of Neck Pain You Should Know
Causes of Swan Neck Deformity
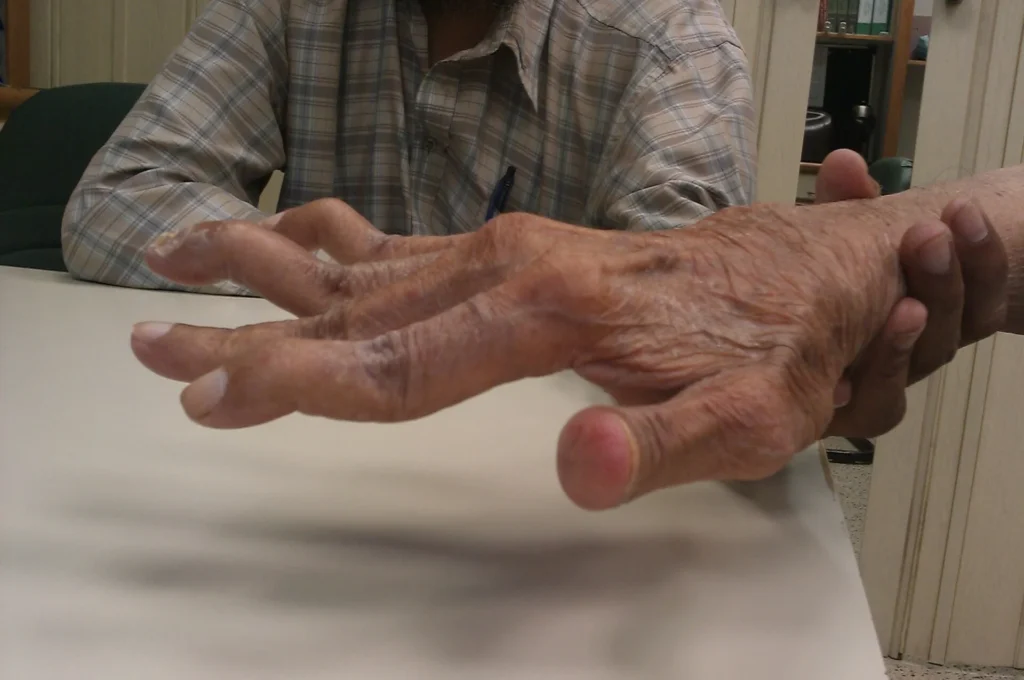
Rheumatoid Arthritis
This is the most common cause. Chronic inflammation weakens ligaments and alters tendon alignment, leading to progressive deformity. Carlson and Carlson (2014)
Trauma and Finger Injuries
- Mallet finger
- Tendon rupture
- Joint injuries
Improper healing can trigger long term imbalance.
Read : Are Your Fingers Or Toes Icy? Let’s Uncover The Reasons
Lesser Known but Important Causes
Post Trigger Finger Surgery
Damage to the pulley system can alter tendon mechanics, leading to abnormal force distribution. Matzon et al. (2023)
Chronic Mallet Finger Neglect
Untreated DIP injuries can evolve into swan neck deformity within weeks or months.
Volar Plate Laxity
Seen in people with hypermobility
Often painless initially but progressively destabilizes the joint.
Neurological Conditions
Muscle imbalance and abnormal tone contribute to deformity.
Congenital Causes
Rare but possible due to inherent tendon imbalance.
Read: How to Fix Sagging,Ozempic Neck After Rapid Weight Loss
Symptoms You Should Not Ignore
- Finger appears bent in a zig zag pattern
- Difficulty gripping objects
- Reduced hand strength
- Stiffness or discomfort
- Clicking or snapping sensation
Important
A painless deformity is often ignored but may worsen silently.
Read about: Cervical Ligament Injury or Neck Ligament Tear
Diagnosis
Diagnosis is primarily clinical:
- Visual inspection
- Range of motion testing
- Tendon balance assessment
Imaging may be used in complex cases.
Read in detail about: How to Fix Upper Crossed Syndrome Naturally
Treatment of Swan Neck Deformity
Treatment of swan neck deformity depends on the stage of the condition, flexibility of the joint, underlying cause, and functional limitations.
From a physiotherapy perspective, the primary goal is not just correcting the deformity but restoring tendon balance, joint stability, and functional hand use.
Early intervention plays a critical role. A flexible deformity can often be managed conservatively, whereas a fixed deformity may require surgical correction followed by structured rehabilitation.
Read about: Effective Neck Pain Exercises At Home: A Complete Guide to Relief and Improved Mobility
Conservative Treatment
Conservative management is most effective in early and correctable stages, where joint structures are still adaptable. The focus is on:
- Preventing progression of deformity
- Restoring biomechanical balance
- Improving functional grip and dexterity
Splinting
Splinting is one of the most important components of conservative treatment.
- Ring splints or custom-made orthoses are commonly used
- These splints block excessive hyperextension at the PIP joint while allowing controlled flexion
- They help maintain optimal alignment during daily activities
A well-designed splint does not completely immobilize the finger. Instead, it guides movement in a safe range, which is essential for tendon healing and joint nutrition.
Clinical insight
Patients often wear splints inconsistently, which reduces effectiveness. Proper education and compliance are key to success. Vishwanathan and Ganjiwale (2018)
Read about: Neck And Jaw Pain Together? Here’s The Full Clinical Picture
Evidence Based Physiotherapy Approach
Physiotherapy is not just about exercises. It is about retraining the entire tendon system to work in harmony again.
1. Controlled PIP Flexion Training
This targets the flexor digitorum superficialis, which plays a crucial role in stabilizing the PIP joint.
- Exercises involve active bending of the PIP joint while preventing DIP compensation
- Helps counteract hyperextension forces
- Improves joint control during functional tasks
Key point
Strengthening without control can worsen imbalance, so movements must be slow and precise.
2. Lateral Band Rebalancing
In swan neck deformity, lateral bands often migrate dorsally, increasing extension forces.
- Specific exercises aim to reposition these bands
- Encourages proper alignment of the extensor mechanism
- Reduces abnormal stress on the PIP joint
Lesser known fact
This is one of the most critical yet under-addressed aspects of rehabilitation.
3. Tendon Gliding Exercises
These exercises improve synchronization between flexor and extensor tendons.
- Promote smooth tendon movement within sheaths
- Reduce adhesions
- Enhance coordination
Typical patterns include:
- Straight hand
- Hook fist
- Full fist
- Tabletop position
Clinical benefit
Better tendon glide directly translates to improved functional hand use.
4. Functional Grip Retraining
Many patients regain movement but still struggle with daily tasks. This is where functional retraining becomes essential.
Focus on:
- Hook grip for carrying objects
- Lumbrical grip for precision tasks
These patterns help restore real-world hand function, not just isolated joint motion.
5. Passive Stretching
Passive stretching must be used carefully.
- Helps maintain joint mobility
- Prevents stiffness
However, excessive stretching can worsen ligament laxity, especially in patients with hypermobility.
Physiotherapy caution
Stretch only within controlled limits and always combine with strengthening.
Read: Do You Suffer Hand And Wrist Pain Due to Excessive Typing?
Neuromuscular Re-education (Advanced Addition)
This is often overlooked but highly valuable.
- Focuses on retraining coordinated muscle activation
- Improves timing between intrinsic and extrinsic muscles
- Enhances joint stability during dynamic movements
This is particularly useful in patients with neurological causes or long-standing deformity.
Read: What is Torticollis? How to treat neck tilt condition
Activity Modification
Daily habits significantly influence recovery.
- Avoid prolonged gripping or pinching
- Reduce repetitive hand strain
- Use ergonomic tools to minimize joint stress
Practical tip
Even simple changes like using a thicker pen or cushioned grip can reduce stress on the finger.
Read: This 1 Mistake Can Worsen Your Wrist Fracture, Here’s How to Avoid It
Pain Management
Pain is not always present, but when it is, it should be addressed early.
- Ice therapy helps reduce inflammation
- Anti-inflammatory medications may be prescribed by a doctor
- Gentle movement is preferred over complete rest
Important
Complete immobilization can lead to stiffness and delayed recovery.
What Makes Conservative Treatment Successful?
From clinical experience, the best outcomes are seen when:
- Treatment starts early
- Splinting is combined with active exercises
- Patients follow a structured rehabilitation plan
- Underlying causes like rheumatoid arthritis are managed
Final physiotherapy insight
Swan neck deformity is not corrected by one method alone. It requires a combination of alignment, strengthening, and functional retraining.
Surgical Treatment
Indicated when:
- Deformity becomes fixed
- Function is significantly impaired
Procedures include:
- Tendon reconstruction
- Lateral band correction
- Tenodesis
Modern approaches such as WALANT allow real time functional assessment during surgery. Gueffier et al. (2021)
Physiotherapy After Surgery
Rehabilitation is critical for success.
Goals
- Restore range of motion
- Prevent stiffness
- Rebalance tendon function
Key Components
- Controlled mobilization
- Gradual strengthening
- Splint progression
Important insight
Poor rehabilitation is a major reason for unsatisfactory outcomes.
Recovery Timeline
- Mild cases: 4 to 8 weeks
- Moderate cases: 2 to 3 months
- Post surgery: 3 to 6 months
Consistency is the most important factor in recovery.
Why Some Patients Do Not Recover Well
Common reasons include:
- Poor adherence to physiotherapy
- Early removal of splints
- Ignoring underlying conditions like rheumatoid arthritis
- Incorrect exercise technique Harris et al. (2023)
Can Swan Neck Deformity Be Reversed?
- Early stage: Often reversible
- Moderate stage: Partially correctable
- Severe stage: Usually requires surgery
Key message
Early detection offers the best chance of full recovery.
Complications if Left Untreated
- Permanent deformity
- Reduced hand function
- Loss of grip strength
- Joint stiffness
Prevention Tips
- Treat finger injuries early
- Do not ignore mallet finger
- Strengthen hand muscles regularly
- Use ergonomic tools
- Manage inflammatory conditions properly
Physiotherapist’s Clinical Pearls
- A painless deformity can still be serious
- Compare both hands for early detection
- Splinting alone is not enough, muscle retraining is essential
- Over stretching can worsen instability
- Early intervention can prevent surgery
Conclusion
Swan neck deformity is not just a cosmetic concern but a reflection of underlying imbalance in the delicate tendon and ligament system of the hand.
From a physiotherapy perspective, it highlights how even small disruptions in biomechanics can gradually lead to significant functional limitations if left unaddressed.
The encouraging part is that early-stage deformities are highly manageable.
With timely intervention, appropriate splinting, and targeted physiotherapy, it is often possible to restore alignment, improve strength, and regain normal hand function without the need for surgery.
The key lies in recognizing the condition early and taking consistent action.
For individuals with more advanced or fixed deformities, surgical options can provide structural correction.
However, the success of any procedure ultimately depends on a well-planned and disciplined rehabilitation program. Physiotherapy remains essential at every stage, whether the goal is prevention, correction, or recovery.
As a clinician, one of the most important messages I share is this: do not ignore subtle changes in your fingers.
A painless deformity today can become a functional limitation tomorrow.
Paying attention to early signs, protecting joint health, and maintaining hand strength can go a long way in preventing long-term complications.
With the right approach, guidance, and commitment, most patients can achieve meaningful recovery and return to their daily activities with confidence.
Frequently Asked Questions
Can swan neck deformity heal without surgery?
Yes, in early stages it can often be corrected with splinting, physiotherapy, and activity modification.
Is swan neck deformity painful?
It may or may not be painful. Some patients experience discomfort, while others notice only functional difficulty.
What causes swan neck deformity?
The most common cause is rheumatoid arthritis, but injuries, tendon imbalance, and ligament laxity can also lead to it.
How long does recovery take?
Mild cases may recover in 4 to 8 weeks, while surgical recovery can take up to 6 months.
Are exercises effective for treatment?
Yes, physiotherapy exercises help restore tendon balance and improve hand function, especially in early stages.
Do I need to wear a splint?
Splints are commonly used to prevent hyperextension and support proper joint alignment during healing.
Can swan neck deformity come back?
Yes, recurrence is possible if the underlying cause is not managed or rehabilitation is incomplete.
When should I see a doctor?
You should consult a healthcare professional if you notice finger deformity, weakness, or difficulty using your hand.
Stay tuned with us for more health related topics.
Follow us on LinkedIn and Instagram for more.
Medical Disclaimer!
This article has been reviewed and written under the guidance of our Head Physiotherapist, Dr. Kruti Raj (PT, MUHS,CPT,CMPT). The information shared is intended for educational purposes only and should not be considered a substitute for personalized medical advice, diagnosis, or treatment.
Please consult us or any other qualified healthcare professional before beginning any exercise program, especially if you are experiencing pain, recovering from injury, or managing a medical condition.











