The frozen shoulder early signs and symptoms often start so subtly that you won’t notice them, until your shoulder suddenly refuses to move.
It has a frustrating reputation and honestly, it earns it.
Patients often walk into my clinic saying, “It just started as mild stiffness and now I can’t even reach my back.”
What makes this condition tricky is not just pain, but the slow, stubborn loss of movement that can last months to years if not managed properly.
This guide will walk you through early signs, stages, recovery timeline, and physiotherapy-based solutions, backed by current research and clinical experience, so you don’t feel lost in the process.
Quick Answer
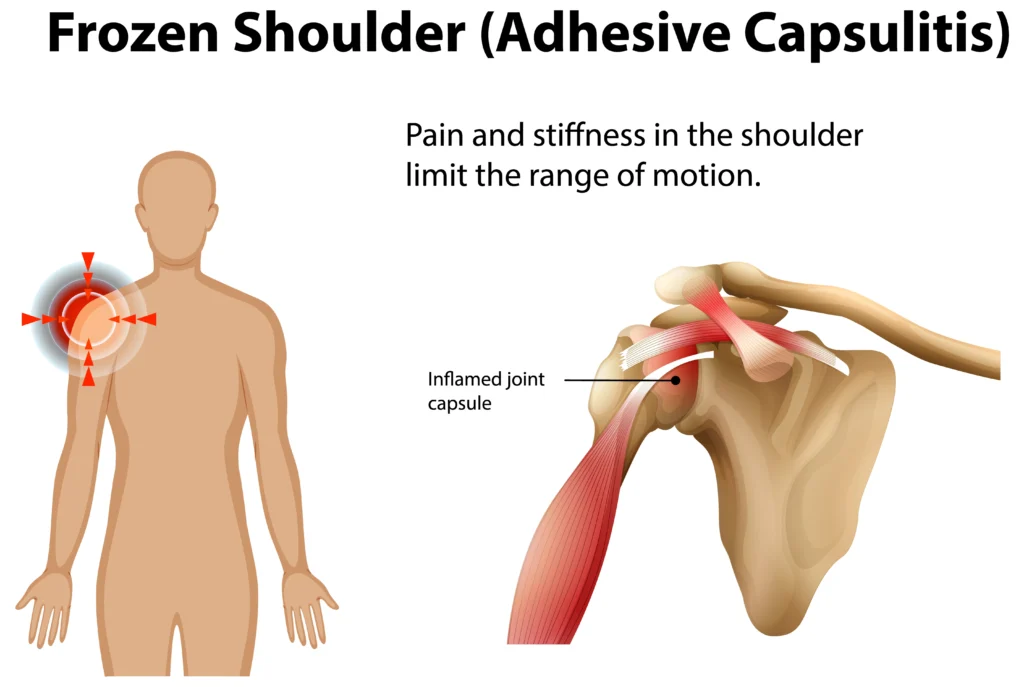
Frozen shoulder (adhesive capsulitis) is a condition causing pain and stiffness in the shoulder joint. It progresses in 3 stages-freezing, frozen, and thawing-and can take 1–3 years to fully recover. Early physiotherapy significantly reduces recovery time and improves movement.
Key Takeaways
- Frozen shoulder develops gradually and worsens over time
- Early stiffness is the most important warning sign
- There are 3 stages: freezing, frozen, thawing
- Recovery can take up to 3 years without treatment
- Physiotherapy can significantly speed up recovery
- Avoid complete rest—controlled movement is essential
What Is Frozen Shoulder (Adhesive Capsulitis)?
Frozen shoulder, medically known as adhesive capsulitis, is a condition where the shoulder joint capsule becomes inflamed, thickened, and stiff, leading to progressive pain and restriction in movement.
Unlike common shoulder pain, this condition affects both:
- Active movement (what you can do)
- Passive movement (what someone else can move for you)
This is a key clinical sign that differentiates it from rotator cuff injuries. (NCBI)
Frozen Shoulder Early Signs And Symptoms
Frozen shoulder rarely starts dramatically. It creeps in quietly.
Subtle Symptoms You Should Not Dismiss
- Mild shoulder stiffness, especially in the morning
- Difficulty reaching overhead or behind the back
- Pain while sleeping on the affected side
- Gradual loss of range, not sudden injury
- Pain that worsens at night
Research Insight: Early stiffness is often misdiagnosed as simple muscle strain, delaying treatment. (PMC)
Lesser-Known Early Indicator
One of the earliest signs I notice clinically:
Difficulty fastening a bra or reaching your back pocket
This is because internal rotation is usually the first movement affected.
Who Is at Higher Risk?
Frozen shoulder is not random, it has strong associations.
High-Risk Groups
- People aged 40-60 years
- Individuals with diabetes (risk increases up to 5x)
- Thyroid disorders
- Post-surgery or prolonged immobilization
- Sedentary lifestyle
Study: Diabetes significantly increases severity and duration. (Cleveland Clinic)
Lesser-Known Fact
Even minor shoulder neglect after pain (like avoiding movement) can trigger frozen shoulder.
Your body reacts by tightening the joint capsule as a protective mechanism.
The 3 Stages of Frozen Shoulder Explained
Frozen shoulder progresses in three distinct stages, each with different symptoms and treatment priorities.
Stage 1: Freezing Phase (Painful Stage)
Duration: 6 weeks to 9 months
What Happens?
- Increasing pain (especially at night)
- Gradual loss of motion
- Inflammation inside the joint capsule
Clinical Insight
This is when patients think:
“It’s just a minor issue, it will go away.”
But this is actually the most critical stage to intervene early.
Study: Detection of frozen shoulder early signs and symptoms leads to early intervention which reduces long-term stiffness. (LongDom)
Stage 2: Frozen Phase (Stiffness Stage)
Duration: 4 to 12 months
What Happens?
- Pain reduces slightly
- Severe stiffness sets in
- Daily activities become difficult
Examples:
- Wearing clothes
- Combing hair
- Driving
Key Physiotherapy Note
Pain may reduce, but function worsens, this confuses many patients.
Stage 3: Thawing Phase (Recovery Stage)
Duration: 6 months to 2 years
What Happens?
- Gradual return of movement
- Reduced stiffness
- Slow functional recovery
Study: Full recovery can take up to 24 months without proper rehab. (PubMed)
Recovery Timeline: What to Expect Realistically
Frozen shoulder is not a “quick fix” condition.
Typical Timeline
- Early stage (painful): 2-9 months
- Stiff phase: 4-12 months
- Recovery phase: 6-24 months
Total duration: 1 to 3 years (if untreated or poorly managed)
With Physiotherapy?
Recovery can be significantly faster:
- Pain controlled earlier
- Movement preserved
- Function restored quicker
10 Physiotherapy Exercises for Frozen Shoulder
This is where recovery truly begins.
The right exercises, done at the right stage, with the right intensity, can dramatically improve outcomes in Frozen Shoulder.
As a physiotherapist, I’ll guide you exactly how I teach my patients in clinic, safe, progressive, and evidence-based.
Before You Start
- Always warm up with heat for 10 minutes
- Exercises should be pain-free or mildly uncomfortable, not sharp pain
- Move slowly and with control
- Consistency matters more than intensity
Research shows gradual mobilization improves range without worsening inflammation. (PMC)
1. Pendulum Exercise (Best for Painful Stage)
How to Do It
- Stand and lean forward slightly, supporting yourself with your other hand
- Let the affected arm hang freely
- Gently swing:
- Forward-backward
- Side-to-side
- Small circles
Reps
- 1-2 minutes, 2-3 times daily
Why It Works
Uses gravity to gently mobilize the joint without strain
Pro Tip
Keep movements small initially, bigger circles come later
2. Wall Walk (Finger Climbing)
How to Do It
- Face a wall
- Use your fingers to slowly “walk” your arm upward
- Stop when you feel a stretch (not pain)
- Hold for 5-10 seconds, then slowly come down
Reps
- 10-15 repetitions
Why It Works
Improves forward elevation (flexion) gradually
Mistake to Avoid
Do NOT shrug your shoulder, keep it relaxed
3. Towel Stretch (Internal Rotation Focus)
How to Do It
- Hold a towel behind your back with both hands
- Use the top hand to gently pull the affected arm upward
- Feel stretch in the shoulder
Hold
- 15-20 seconds
Reps
- 8-10 times
Why It Works
Targets internal rotation, usually the first movement restricted
4. Cross-Body Stretch
How to Do It
- Bring affected arm across your chest
- Use the opposite hand to support and gently pull
Hold
- 20-30 seconds
Reps
- 8-10 times
Why It Works
Improves posterior capsule flexibility
Tight posterior capsule is a key contributor to stiffness (PubMed)
5. External Rotation with Stick
How to Do It
- Hold a stick (or umbrella) with both hands
- Keep elbows at your sides
- Use the healthy arm to push the affected arm outward
Reps
- 10-15 slow repetitions
Why It Works
Restores external rotation, essential for daily tasks
6. Internal Rotation Stretch (Behind the Back)
How to Do It
- Place affected hand behind your back
- Use other hand or towel to gently pull upward
Hold
- 15-20 seconds
Why It Works
Critical for activities like dressing and hygiene
7. Shoulder Blade Squeeze (Scapular Retraction)
How to Do It
- Sit or stand upright
- Pull your shoulder blades back and down
- Hold for 5 seconds
Reps
- 15-20 repetitions
Why It Works
Improves scapular stability, reducing compensatory strain
Lesser-Known Insight
Poor scapular control can slow frozen shoulder recovery
8. Resistance Band External Rotation
How to Do It
- Attach resistance band to a stable object
- Keep elbow at 90° close to body
- Rotate arm outward slowly
Reps
- 10-12 repetitions × 2 sets
Why It Works
Strengthens rotator cuff muscles
Strengthening improves long-term outcomes and reduces recurrence. (PMC)
9. Overhead Reach
How to Do It
- Use your other hand or a stick to assist lifting your arm overhead
- Move slowly within comfort
Reps
- 10-12 repetitions
Why It Works
Restores functional overhead movement
10. Functional Reach Training
How to Do It
Practice real-life movements:
- Reaching shelves
- Combing hair
- Wearing clothes
Why It Works
Retrains the brain + shoulder coordination
Pro Tip
This is where true recovery happens, not just exercises, but real-life movement confidence
Weekly Progression Plan
Week 1-2
- Focus: Pain relief + gentle mobility
- Exercises: Pendulum, wall walk
Week 3-6
- Add: Stretching + assisted movements
Week 6+
- Add: Strength training + functional tasks
What to Avoid During Exercise
- Jerky or fast movements
- Lifting heavy weights early
- Ignoring pain signals
- Comparing with others’ recovery speed
Simple Daily Routine
Morning (10-15 min):
- Heat + pendulum + wall walk
Afternoon:
- Stretching exercises
Evening:
- Strength + functional reach
Lesser-Known Tips That Speed Up Recovery
1. Don’t Stop Using Your Shoulder Completely
Avoiding movement worsens stiffness.
2. Sleep Position Matters
- Avoid sleeping on affected side
- Use pillow support under arm
3. Heat Before Exercise, Ice After
- Heat improves mobility
- Ice reduces inflammation
4. Hydration & Tissue Health
Dehydrated tissues are less elastic.
5. Manage Blood Sugar (Very Important)
In diabetics, recovery is slower if sugars are uncontrolled.
6. Breathe While Stretching
Holding breath increases muscle tension
7. Small Gains Matter
Even 5° improvement is progress
8. Morning vs Evening
- Stiffness is worse in morning, do gentle exercises then
- Stretch deeper in evening
9. Don’t Chase Pain
Aggressive stretching = more inflammation = delayed recovery
Things You Must Avoid
- Aggressive stretching in early stage
- Ignoring early stiffness
- Long periods of immobilization
- Overhead heavy lifting too soon
- Self-manipulation or forceful cracking
Medical Treatment Options
- Anti-inflammatory medications
- Corticosteroid injections
- Hydrodilatation
- Rarely, surgery
Study: Steroid injections provide short-term relief but must be combined with physiotherapy (PMC)
Red Flags
- Sudden severe pain after injury
- Loss of sensation or weakness
- No improvement after months
- Severe night pain not improving
My Clinical Insight
Frozen shoulder is not just about stiffness, it is your body’s protective response gone overboard.
The biggest mistake I see:
Patients waiting too long before starting physiotherapy.
Early guided movement can literally cut recovery time in half.
My Clinical Insight
The biggest mistake patients make is either:
- Doing too little, or
- Doing too much too soon
Frozen shoulder recovery is about controlled consistency, not force.
The shoulder capsule needs gradual persuasion, not aggression.
Myth vs Reality
Myth: It will heal on its own
Reality: It may, but often with long-term stiffness
Myth: Pain means stop movement
Reality: Controlled movement is essential
Final Word
These exercises are not just movements, they are your roadmap out of stiffness.
If done correctly:
- Pain reduces faster
- Movement returns steadily
- Recovery becomes predictable
Stay consistent, stay patient and your shoulder will open up again.
Don’t wait for stiffness to take control.
Recognizing the frozen shoulder early signs and symptoms today could save you months of pain tomorrow.
Frozen Shoulder: Frequently Asked Questions
1. What is the first warning sign of frozen shoulder?
The earliest sign is mild stiffness with difficulty reaching behind your back, often accompanied by night pain.
2. How do I know if my shoulder pain is frozen shoulder?
If both active and passive movements are restricted along with gradual stiffness progression, it is likely frozen shoulder.
3. How long does frozen shoulder take to heal?
Recovery can take anywhere from 12 to 36 months depending on the stage and treatment approach.
4. Can frozen shoulder go away on its own?
Yes, but without physiotherapy, recovery is slower and may result in long-term stiffness.
5. What is the fastest way to recover from frozen shoulder?
Early physiotherapy, controlled exercises, and pain management techniques significantly speed up recovery.
6. Which exercises are best for frozen shoulder?
Pendulum exercises, wall walks, towel stretches, and resistance band strengthening are most effective.
7. Is frozen shoulder more common in diabetics?
Yes, people with diabetes are up to 5 times more likely to develop frozen shoulder.
8. Should I rest my shoulder completely?
No, complete rest can worsen stiffness. Gentle, guided movement is essential.
9. Can frozen shoulder come back again?
It can recur, especially if underlying risk factors like diabetes or inactivity are not managed.
10. When should I see a doctor for frozen shoulder?
If pain persists, movement reduces significantly, or symptoms worsen over weeks, consult a specialist early.
Stay tuned with us for more health related topics.
Follow us on LinkedIn and Instagram for more.
Medical Disclaimer!
This article has been reviewed and written under the guidance of our Head Physiotherapist, Dr. Kruti Raj (PT, MUHS,CPT,CMPT). The information shared is intended for educational purposes only and should not be considered a substitute for personalized medical advice, diagnosis, or treatment.
Please consult us or any other qualified healthcare professional before beginning any exercise program, especially if you are experiencing pain, recovering from injury, or managing a medical condition.











