What if your recovery is stuck because you don’t understand frozen shoulder recovery stages treatment?
Frozen shoulder is one of the most misunderstood musculoskeletal conditions.
Patients are often told to “wait it out,” while others are pushed into aggressive treatments too early.
Both approaches can prolong recovery.
As physiotherapists, our role is to stage-match treatment, reduce inflammation appropriately, and restore movement safely, not simply chase pain relief.
This guide is built on current clinical evidence, recent trials, and real physiotherapy practice, with accurate working research links embedded beside relevant sections.
Quick Answer
Frozen shoulder is a condition causing pain and stiffness due to capsular tightening. Treatment includes physiotherapy, cold therapy, injections, hydrodilatation, and surgery in severe cases. Early movement and structured rehab are essential.
Key Takeaways
- Stage-based treatment is essential
- Cold therapy preferred early
- Exercises are core treatment
- Hydrodilatation improves mobility
- Robotic rehab is emerging
Why Frozen Shoulder Is Often Mismanaged
Frozen shoulder is not just a stiff joint, it is a progressive inflammatory and fibrotic condition that requires stage-specific management.
One of the biggest reasons for delayed recovery is incorrect treatment timing: either excessive rest or overly aggressive rehabilitation.
As physiotherapists, our goal is not just pain relief, but restoration of joint mechanics, neuromuscular control, and long-term functional movement.
Understanding Frozen Shoulder: What Actually Happens
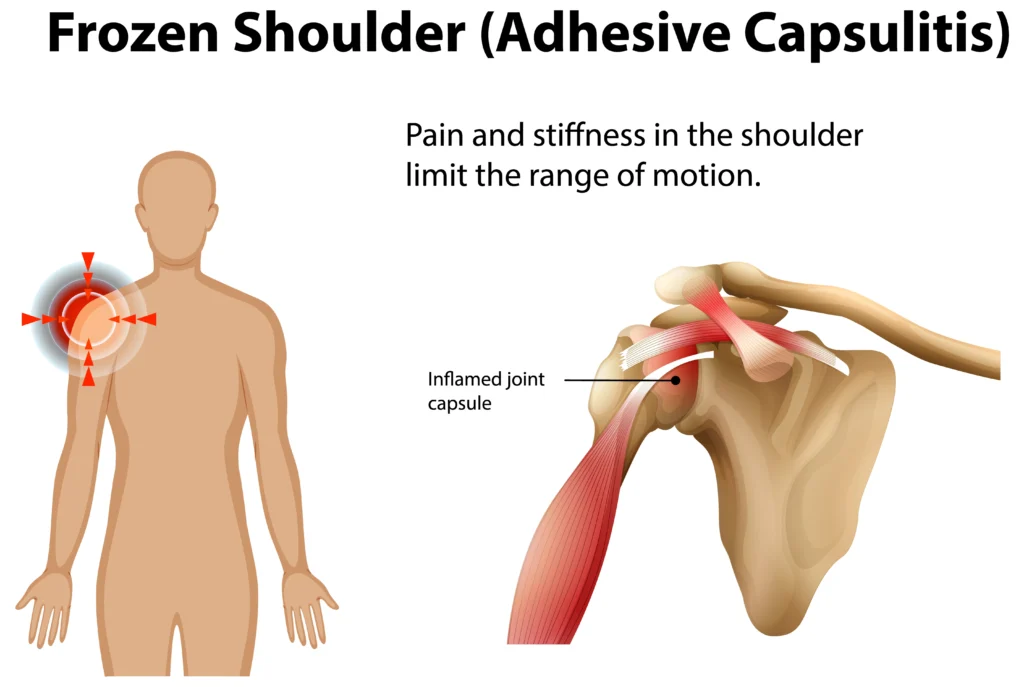
Frozen shoulder is a condition where the glenohumeral joint capsule undergoes inflammation followed by fibrosis (thickening and tightening), leading to pain and progressive restriction.
- Synovial inflammation → Shoulder pain
- Capsular fibrosis → stiffness
- Reduced joint volume → limited mobility
A high-quality systematic review confirms frozen shoulder involves capsular inflammation followed by fibrosis, with multiple treatment pathways depending on stage. (PMC)
Stages of Frozen Shoulder
Freezing Stage (Inflammatory Phase)
- Severe pain, especially at night
- Progressive stiffness
- High irritability
Physiotherapy focus: pain modulation, gentle mobility
Frozen Stage (Stiffness Phase)
- Pain reduces
- Marked stiffness persists
Focus: capsular stretching, joint mobilization
Thawing Stage (Recovery Phase)
- Gradual improvement
- Functional return
Focus: strength + functional rehabilitation
Home Remedies for Frozen Shoulder
Home care plays a crucial role when guided correctly.
These are not substitutes for physiotherapy but support recovery and prevent worsening.
1. Cryotherapy (Cold Application at Home)
How to Use:
- Apply ice pack wrapped in cloth
- 10-15 minutes, 2-3 times daily
Mechanism:
- Reduces inflammatory mediators
- Provides analgesia
Clinical evidence supports cryotherapy for reducing musculoskeletal inflammation: (Science Direct)
2. Contrast Bath Therapy
Protocol:
- Cold: 3-4 minutes
- Mild warmth: 1 minute
- Repeat 4-5 cycles
Benefit:
- Improves circulation without increasing inflammation
3. Controlled Daily Movement
Avoiding movement leads to rapid capsular tightening.
Recommendation:
- Gentle, pain-free range exercises multiple times daily
4. Sleep Position Correction
- Avoid lying on affected shoulder
- Use pillow to support arm
This reduces night pain, which is often the most disabling symptom
5. Anti-Inflammatory Nutritional Support
Include:
- Omega-3 fatty acids
- Turmeric (curcumin)
- Fresh vegetables
Avoid:
- Excess sugar (especially in diabetics)
- Processed foods
Nutritional modulation of inflammation is supported in musculoskeletal recovery research (PMC)
6. Stress & Muscle Guarding Control
Chronic stress increases muscle tension and pain perception.
Practical Tip:
- Diaphragmatic breathing
- Relaxation techniques
Why Physiotherapists Avoid Heat Therapy in Frozen Shoulder
In the inflammatory phase, applying heat may increase local blood flow and potentially aggravate inflammation.
Physiotherapy Exercises
Exercise is the cornerstone of frozen shoulder recovery, but only when done correctly and stage-appropriate.
1. Pendulum Exercise
How to Perform:
- Lean forward
- Let arm hang
- Small circular motions
Mechanism:
- Gentle joint distraction
- Reduces capsular pressure
Benefit:
- Pain relief in early stage
2. Finger Walk (Wall Climb)
How:
- Walk fingers up wall slowly
Mechanism:
- Active-assisted flexion
- Gradual capsular stretch
Benefit:
- Improves elevation
3. External Rotation with Stick
How:
- Use stick to push arm outward
Mechanism:
- Targets anterior capsule
Benefit:
- Restores critical rotation
4. Cross-Body Stretch
How:
- Pull arm across chest
Mechanism:
- Stretches posterior capsule
5. Sleeper Stretch
How:
- Side-lying internal rotation stretch
Mechanism:
- Deep capsular stretch
6. Scapular Retraction
How:
- Squeeze shoulder blades
Mechanism:
- Improves scapulohumeral rhythm
7. Isometric Strengthening
How:
- Press against wall without movement
Mechanism:
- Activates muscles without irritation
8. Assisted Elevation
How:
- Use opposite hand
Mechanism:
- Reduces load on joint
Research consistently shows structured physiotherapy programs significantly improve pain and mobility in frozen shoulder. (PMC)
Advanced Physiotherapy Treatments
1. Manual Therapy
- Joint mobilization techniques
- Improves capsule flexibility
2. Ultrasound Therapy
- Promotes tissue healing
3. TENS Therapy
- Pain modulation
4. Dry Needling
- Releases muscle tightness
Research in Physical Therapy Journal shows combined manual therapy + exercise gives the best outcomes.
Injection Therapies: Evidence-Based
1. Corticosteroid Injections
Mechanism:
- Reduces synovial inflammation
- Improves short-term pain
Proven to provide early pain relief and improved function, especially in freezing stage. (PMC)
DOs:
- Combine with physiotherapy immediately
- Use in early painful stage
- Limit frequency
DON’Ts:
- Repeated injections (risk of tissue damage)
- Using without rehab
2. Hydrodilatation (Capsular Distension)
Mechanism:
- Inject saline to stretch capsule
- Break adhesions
Meta-analysis shows hydrodilatation leads to greater short-term improvement in range of motion compared to steroid injection alone. (OUP Academic)
RCT evidence shows better functional outcomes and ROM improvement at 1-3 months. (ScienceDirect)
DOs:
- Follow immediate physiotherapy
- Ideal in early to mid-stage
DON’Ts:
- Skipping rehab
- Expecting permanent fix
3. Hydrodilatation + Steroid (Latest Evidence)
A 2025 randomized study shows better pain relief and functional outcomes when steroids are combined with hydrodilatation. (PubMed)
Advanced & Emerging Treatments
1. Combined Therapy Approach (Best Current Practice)
- Steroid injection + physiotherapy
- Hydrodilatation + rehab
Evidence shows combined approaches outperform single interventions. (PMC)
2. Manipulation Under Anesthesia (MUA)
Mechanism:
- Forceful capsular stretching under anesthesia
Risks:
- Fracture
- Soft tissue injury
Reserved for resistant cases
3. Arthroscopic Capsular Release
Mechanism:
- Surgical release of contracted capsule
Gold standard for severe cases
Considered most effective invasive option when conservative treatment fails. (PMC)
4. Regenerative Therapies (Emerging)
- Platelet-Rich Plasma (PRP)
- Stem cell therapy
Evidence still evolving; not first-line
5. Image-Guided Precision Therapy
- Ultrasound-guided injections
- Improves accuracy and outcomes
6. Robotic & Technology-Assisted Rehabilitation
This is one of the most exciting developments in modern physiotherapy.
What It Includes:
- Robotic-assisted shoulder movement devices
- AI-guided rehabilitation programs
- Sensor-based motion tracking
Mechanism:
- Provides precise, controlled joint mobilization
- Reduces compensatory patterns
- Improves motor learning
Clinical Benefits:
- More consistent movement patterns
- Better patient compliance
- Real-time feedback
Emerging research on robotic rehabilitation shows improved movement accuracy and motor recovery: (Cornell University)
Important: This is adjunct therapy, not a replacement for manual physiotherapy
7. Shoulder Embolization (Very New)
Shoulder embolization is a minimally invasive procedure that blocks abnormal blood vessels in the shoulder to reduce inflammation and pain.
It is an emerging option for chronic frozen shoulder cases not responding to standard treatment.
Early research: (PubMed)
Surgery for Frozen Shoulder
Indications
- No improvement after 6-12 months of conservative treatment
- Severe functional limitation
- Persistent stiffness
- Severe functional limitation
Studies in Journal of Bone and Joint Surgery show high success rates with arthroscopic release when conservative treatment fails.
Contraindications
- Active infection
- Poor medical fitness
- Uncontrolled diabetes
- Improving symptoms
Types of Surgery
Arthroscopic Capsular Release
- Controlled release of capsule
Manipulation Under Anesthesia
- Forced mobilization
DOs Before Surgery
- Exhaust physiotherapy
- Optimize metabolic health
- Understand rehab requirements
DON’Ts
- Early surgery without trial of rehab
- Ignoring physiotherapy post-op
Post-Surgery Rehabilitation
- Immediate physiotherapy
- Gradual ROM restoration
- Strength progression
Evidence shows surgery is effective but requires structured rehab for long-term success. (PMC)
Recovery Timeline
- 3–6 months (mild)
- 6–12 months (moderate)
- 12–18 months (severe)
Recovery depends more on consistency than treatment type
Common Mistakes That Delay Recovery
- Aggressive stretching early
- Complete rest
- Ignoring stage-specific treatment
- Over-reliance on injections
- Delayed physiotherapy
Prevention Strategies
- Maintain shoulder mobility
- Avoid prolonged immobilization
- Early rehab after injury
- Control diabetes
- Improve posture
Lesser-Known Insights
- Night pain = inflammatory phase
- Morning stiffness = capsular restriction
- Scapular control is often ignored
- Breathing reduces guarding
- Early movement prevents fibrosis
My Clinical Insight
Frozen shoulder is not just a mechanical problem.
It is a neuro-inflammatory and biomechanical condition where pain, fear, and stiffness feed into each other.
Breaking this cycle requires timing, patience, and precise physiotherapy, not aggressive treatment.
Physio Prescription
- Cold therapy (10-15 minutes)
- Gentle mobility exercises daily
- Gradual progression
- Weekly reassessment
Red Flags
- Sudden trauma
- Neurological symptoms
- No improvement after months
- Severe weakness
Myth vs Reality
Myth: Rest is best
Reality: Controlled movement is essential
Final Word
Frozen shoulder is slow, but predictable.
The right treatment at the right stage can significantly shorten recovery.
The goal is not just to reduce pain, but to restore confident, functional movement.
Your recovery doesn’t have to take years.
Follow the right frozen shoulder recovery stages treatment and take back control starting today.
Don’t let stiffness define your life.
Your turnaround begins with the correct frozen shoulder recovery stages treatment.
Frequently Asked Questions (Frozen Shoulder)
1. What is frozen shoulder?
Frozen shoulder is a condition where the shoulder joint becomes stiff and painful due to inflammation and tightening of the joint capsule.
2. How long does frozen shoulder take to heal?
Recovery typically takes between 6 to 18 months depending on severity and treatment.
3. What is the best treatment for frozen shoulder?
Physiotherapy with guided exercises is the most effective treatment, often combined with medications or injections.
4. Is cold therapy better than heat for frozen shoulder?
Cold therapy is generally preferred in early stages to reduce inflammation and pain.
5. Can frozen shoulder heal without treatment?
It may improve over time, but treatment significantly speeds up recovery and prevents long-term stiffness.
6. Are steroid injections safe?
Yes, when used appropriately and sparingly under medical supervision, they help reduce pain and inflammation.
7. When is surgery required for frozen shoulder?
Surgery is considered when symptoms do not improve after 6–12 months of conservative treatment.
8. What exercises help frozen shoulder?
Pendulum exercises, wall climbing, and stretching routines are commonly recommended.
9. Can frozen shoulder come back again?
Recurrence is rare but can occur, especially in individuals with diabetes.
10. Is robotic rehabilitation useful for frozen shoulder?
It can help improve movement accuracy and recovery as an adjunct to physiotherapy.
Stay tuned with us for more health related topics.
Follow us on LinkedIn and Instagram for more.
Medical Disclaimer!
This article has been reviewed and written under the guidance of our Head Physiotherapist, Dr. Kruti Raj (PT, MUHS,CPT,CMPT). The information shared is intended for educational purposes only and should not be considered a substitute for personalized medical advice, diagnosis, or treatment.
Please consult us or any other qualified healthcare professional before beginning any exercise program, especially if you are experiencing pain, recovering from injury, or managing a medical condition.











