There is a type of neck pain that does not follow the usual rules.
A patient sits in front of you and points to a very specific spot on the front of the neck. Not the back, not the shoulder, but just beside the windpipe.
They often say something like, “It hurts when I swallow or even when I touch here lightly.”
At first glance, it may look like a simple muscular issue. But when you examine further, things do not quite add up.
Movement does not fully reproduce the pain. Stretching does not ease it. And local pressure feels unusually sharp.
This is where carotidynia comes into the picture.
Read about our Complete Neck Pain Guide : Causes, Symptoms, Exercises and Treatment
Quick Answer
Carotidynia is a rare inflammatory condition that causes sharp, localized pain on one side of the front of the neck, usually over the carotid artery. Unlike muscle pain, it often worsens with swallowing or light touch and does not improve with stretching.
Read about: Early Signs of Cervical Spine Damage You Should Never Ignore
Key Takeaways
- Carotidynia causes very specific, one-sided front neck pain that feels different from usual muscle pain.
- It is mainly an inflammatory condition around the carotid artery, not a mechanical neck problem.
- Swallowing pain and touch sensitivity are common clues that help identify it early.
- Avoid deep massage or aggressive neck treatment, as it may worsen symptoms.
- Physiotherapy focuses on posture correction, relaxation, and indirect support rather than local treatment.
- Most cases improve within 1 to 3 weeks with proper care and reassurance.
- If symptoms include dizziness, vision changes, or severe sudden pain, seek medical attention immediately.
Read: Understanding Pain In The Front Side Of The Neck
What is carotidynia in simple clinical terms
Carotidynia is a condition characterized by localized pain and tenderness over the carotid artery, usually near its bifurcation.
It is most often unilateral and presents with very specific point tenderness.
In recent years, the condition has been more clearly defined as Transient Perivascular Inflammation of the Carotid artery (TIPIC syndrome).
This shift is important because it moves our understanding away from a vague pain description to a defined inflammatory process. (Lecler et al., 2017)
This study demonstrated imaging evidence of perivascular inflammation, helping establish carotidynia as a distinct entity rather than just a symptom.
Read: What is Sternocleidomastoid Syndrome, Trigger Points and Its Treatment
Why carotidynia is often missed in practice
From a physiotherapy perspective, carotidynia can easily be mistaken for more common conditions.
Patients are frequently treated for:
- Sternocleidomastoid tightness
- Cervical strain
- Myofascial trigger points
The problem is that carotidynia does not behave like a mechanical disorder.
It sits in a grey zone between vascular and musculoskeletal systems, which is why it is often overlooked or misdiagnosed. (Biousse et al., 1994)
This paper emphasized the importance of distinguishing carotidynia from serious vascular pathologies.
Read about: What Is Cervical Myofascial Pain Syndrome And How To Relieve Trigger Points
What happens inside the neck
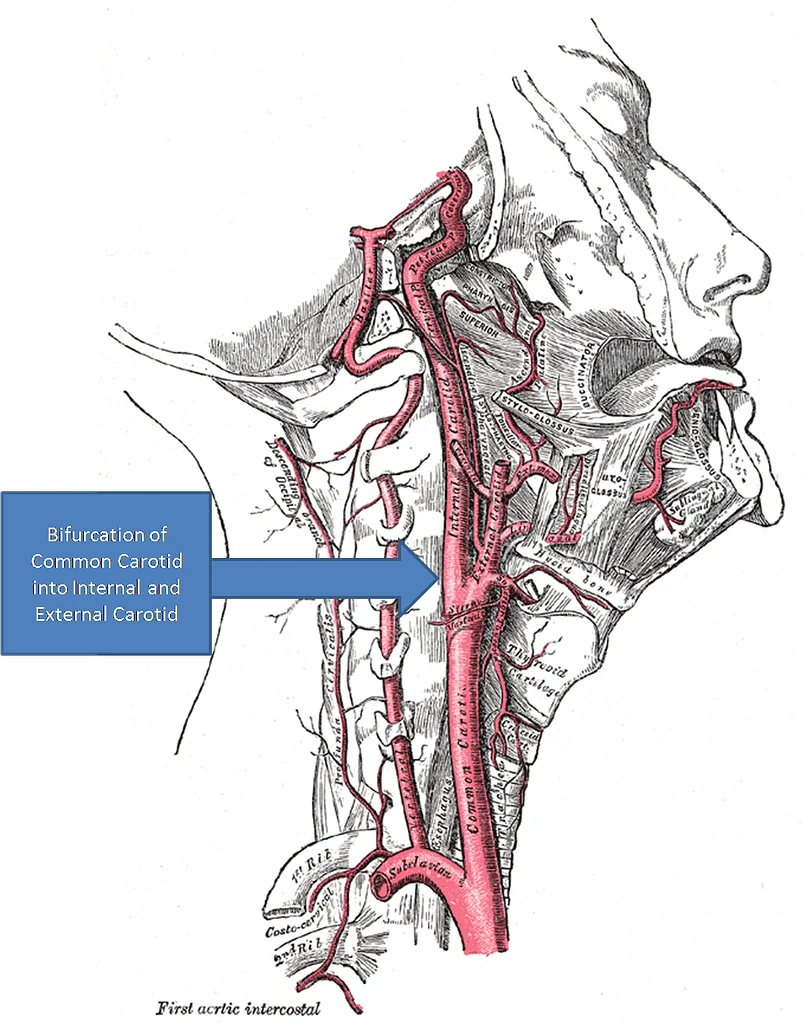
Current evidence suggests that carotidynia is primarily an inflammatory condition affecting the tissues surrounding the carotid artery.
What imaging typically shows:
- Localized inflammation around the artery
- Soft tissue thickening
- No significant blockage in most cases
This study supports the concept of transient inflammation with a self-limiting course. (Kosaka et al., 2020)
Also Read: Sore Throat and Stiff Neck: When to Worry
Recognizing the symptom pattern
Once you see a few cases, the pattern becomes quite recognizable.
Common symptoms
- Pain on one side of the neck
- Very localized tenderness
- Pain during swallowing
- Discomfort while speaking for long periods
- Radiation to jaw or ear in some cases
What makes it different from muscle pain
- Pain is sharply localized
- Light touch can be very sensitive
- Stretching does not reduce symptoms
- Movement does not fully explain the pain
Patients often point to the exact spot with one finger. That level of precision is a useful clinical clue.
Read about: Neck And Jaw Pain Together? Here’s The Full Clinical Picture
What a Typical Carotidynia Episode Feels Like
Patients often feel more reassured when they understand how the condition typically unfolds. In clinical practice, carotidynia tends to follow a fairly predictable pattern.
Day 1 to 3
Pain appears suddenly, usually on one side. It feels sharp or deep and is very localized. Swallowing or touching the area becomes uncomfortable.
Day 3 to 7
Pain intensity may peak. Patients often become anxious during this phase because the location feels unusual and sensitive.
Week 2
Symptoms begin to settle. Tenderness reduces gradually, and daily activities become easier.
Week 3 onwards
Most patients recover completely without any long-term issues.
One thing I often tell my patients is this: if the pain is not behaving like muscle pain, do not panic, but do not ignore it either. Observe it, protect the area, and get it properly assessed.
Read about : 15 Common Causes of Neck Pain You Should Know
Causes and triggers
The exact cause is still not fully established, but several contributing factors are recognized.
1. Local inflammation
This is the most widely accepted mechanism.
2. Post-infectious onset
Many patients report symptoms after:
- Cold
- Flu
- Upper respiratory infection
3. Immune response
Some recent studies suggest a possible immune-mediated component.
4. Rare vascular association
Although uncommon, recurrent cases have been linked with vascular complications. (Morcillo et al., 2024)
This recent report discussed recurrence and highlighted the importance of careful evaluation in atypical cases.
Also Read: Neck Pain with Fever: When To Worry And How To Treat
Differential diagnosis you should never skip
Before concluding carotidynia, it is essential to rule out serious conditions.
Critical conditions
- Carotid artery dissection
- Giant cell arteritis
- Thrombosis
- Tumors
Common musculoskeletal mimics
- Sternocleidomastoid trigger points
- Cervical facet dysfunction
- Temporomandibular disorders
This step is where clinical responsibility becomes crucial. Not every anterior neck pain is benign.
Read about : What is Cervical Facet Joint Pain, how it causes cervicogenic headaches and how to correct it naturally
Assessment approach in physiotherapy
A structured approach makes all the difference.
History taking
Ask specifically:
- Did it start after an illness
- Is swallowing painful
- Is the pain very localized
Palpation
Gently examine the anterior neck. Avoid deep pressure.
If there is sharp tenderness directly over the carotid region, proceed cautiously.
Movement testing
Assess cervical motion, but observe carefully:
- Does movement reproduce symptoms fully
- Or is the pain independent of motion
Red flag screening
Always check for:
- Neurological symptoms
- Dizziness
- Visual disturbances
If present, refer immediately.
Read: How to Treat Trismus- A Jaw Stiffness Naturally with Exercises
Imaging and confirmation
Carotidynia is often confirmed using imaging when needed.
Useful modalities
- MRI
- Ultrasound
Typical findings include perivascular inflammation without significant narrowing. (Lecler et al., 2017)
Read: Branchial Cleft Cyst: A Complete Guide To Neck Lump
Natural course and recovery
One reassuring aspect is that carotidynia is usually self-limiting. (Kosaka et al., 2020)
- Most cases resolve within 1 to 3 weeks
- Pain may be intense initially
- Recurrence is possible but uncommon
Read more: Cervical Vertigo Explained: Why Neck Pain Make You Feel Dizzy
Physiotherapy management: a careful and indirect approach
This is where clinical judgment is essential.
What to avoid
- Deep tissue work over the carotid area
- Aggressive stretching
- High velocity manipulations
- Direct pressure techniques
These can worsen symptoms and may carry risk.
Read about: Effective Neck Pain Exercises At Home: A Complete Guide to Relief and Improved Mobility
What actually helps patients
1. Clear explanation and reassurance
Patients often worry because of the location of pain.
Explain:
- It is inflammatory
- It is temporary
- It usually resolves
This alone reduces fear significantly.
Simple Posture Correction Exercises for Forward Head Posture
2. Postural correction
Focus on reducing strain:
- Neutral head alignment
- Avoid forward head posture
- Limit prolonged screen time
Read about: Which Is The Best Sitting Posture To Avoid Neck Pain And How To Achieve It
3. Indirect treatment strategies
Work away from the painful site:
- Upper trapezius relaxation
- Thoracic mobility
- Gentle scapular work
4. Pain modulation
- Heat therapy
- Relaxed breathing exercises
- Activity pacing
Read more: Heat Or Cold Therapy for Neck Pain: What Actually Works?
5. Activity modification
Advise patients to:
- Avoid sudden neck movements
- Limit excessive talking if painful
- Avoid pressing or massaging the area
Medical management awareness
Patients are often prescribed:
- NSAIDs
- Anti-inflammatory medication
In some cases:
- Corticosteroids
Your role is supportive, ensuring safe recovery.
Also Read: Neck Pain When Coughing: Causes, Relief, and When to Worry
Lesser-known but important clinical insights
It is more common than we think
Many cases go undiagnosed or mislabeled.
Pain location is a major clue
Patients usually indicate a very precise spot.
It does not respond to typical physiotherapy
If standard treatment fails, rethink your diagnosis.
It can recur
Though uncommon, recurrence has been documented. (Morcillo et al., 2024)
Read: Branchial Cleft Cyst: A Complete Guide To Neck Lump
Simple Self-Check
When It Might Be Carotidynia vs Muscle Pain
If you are unsure whether your pain is muscular or something like carotidynia, these simple observations can help.
It may be carotidynia if:
- Pain is very specific to one small point in the front of the neck
- Light touch feels unusually tender
- Swallowing increases discomfort
- Stretching does not relieve the pain
It is more likely muscle-related if:
- Pain spreads across a broader area
- Movement clearly increases or decreases symptoms
- Massage or stretching provides relief
- Pain is linked to posture or activity
This is not a diagnosis, but it gives you a direction.
If something feels different from your usual neck pain experience, it is always worth getting it checked.
Read: Understanding Dropped Head Syndrome in Simple Terms
When to refer immediately
Do not delay referral if you notice:
- Sudden severe pain
- Neurological symptoms
- Vision changes
- Fainting or dizziness
These are not typical for carotidynia and require urgent evaluation.
Read : Chiropractic for Neck Pain: Does It Really Work?
Frequently Asked Questions
1. What is carotidynia?
Carotidynia is a condition involving localized pain and tenderness over the carotid artery due to inflammation.
2. Is carotidynia dangerous?
It is usually self-limiting, but proper evaluation is necessary to rule out serious vascular conditions.
3. How long does carotidynia last?
Most cases resolve within 1 to 3 weeks with appropriate care.
4. Can physiotherapy treat carotidynia?
Physiotherapy supports recovery through posture correction and pain management but avoids direct treatment over the artery.
5. What activities should be avoided?
Avoid deep pressure, aggressive neck movements, and excessive strain on the neck.
6. Can carotidynia come back?
Recurrence is rare but has been reported in some cases.
7. Do I need imaging?
Imaging may be required if diagnosis is unclear or to rule out serious conditions.
Stay tuned with us for more health related topics.
Follow us on LinkedIn and Instagram for more.
Medical Disclaimer!
This article has been reviewed and written under the guidance of our Head Physiotherapist, Dr. Kruti Raj (PT, MUHS,CPT,CMPT). The information shared is intended for educational purposes only and should not be considered a substitute for personalized medical advice, diagnosis, or treatment.
Please consult us or any other qualified healthcare professional before beginning any exercise program, especially if you are experiencing pain, recovering from injury, or managing a medical condition.











