It starts as a dull ache and slowly worsens, learning how to treat shoulder avascular necrosis at the right time can change everything.
Shoulder avascular necrosis, also called Avascular Necrosis, is a condition where the blood supply to the top of your arm bone slowly reduces.
This part of the bone is called the humeral head.
When blood flow drops, bone tissue does not get enough oxygen. Over time, it weakens and may collapse.
This is not a muscle issue. It is a bone problem that starts quietly.
Quick Answer
Shoulder avascular necrosis (AVN) is a condition where reduced blood supply damages the humeral head bone inside the shoulder joint. Early symptoms often include deep shoulder pain, night pain, stiffness, and weakness. MRI is usually needed for early diagnosis. Physiotherapy plays a major role in pain relief, mobility restoration, joint protection, and delaying surgery. Early treatment and proper activity modification can significantly improve long-term shoulder function.
Key Takeaways
- Shoulder AVN starts silently and is often missed in early stages.
- Deep shoulder pain and night pain are important warning signs.
- MRI is the most reliable method for early diagnosis.
- Heavy exercise and overloading the shoulder can worsen bone damage.
- Physiotherapy helps improve movement, reduce pain, and protect the joint.
- Scapular control and posture play a bigger role than many people realize.
- Lifestyle changes like quitting smoking and reducing alcohol matter significantly.
- Early treatment improves the chances of avoiding surgery.
Why many people miss avascular necrosis in the beginning
In clinic, I often hear this:
“I thought it was just shoulder stiffness”
That is exactly why AVN is tricky.
Early stage:
- No visible swelling
- No injury history
- X-ray often looks normal
But internally, changes have already started.
MRI is usually what reveals it early. (Mitchell et al., 2020)
What actually happens inside your shoulder
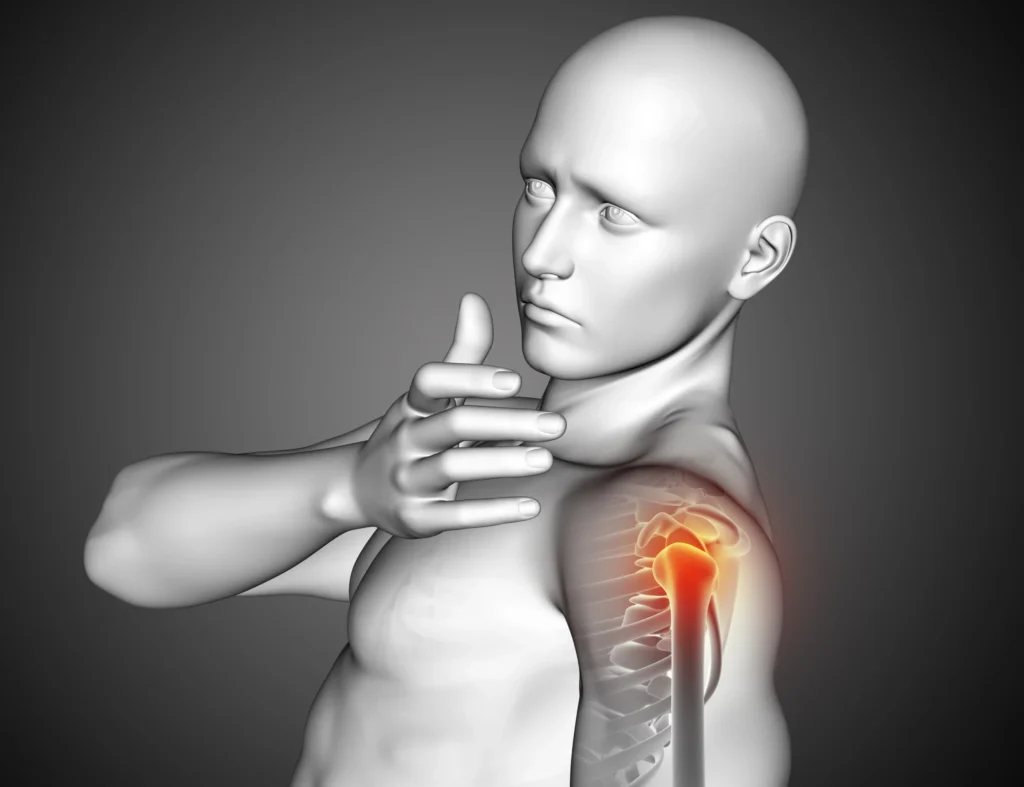
Your shoulder is one of the most mobile joints in the body.
That mobility comes at a cost. It depends heavily on soft tissue support and blood supply.
If circulation reduces:
- Bone cells begin to die
- Structure weakens from inside
- Surface collapse happens later
This is why symptoms and damage do not appear at the same time.
Causes I commonly see in patients
Some causes are well known. Others are often overlooked.
Common causes
- Steroid use
- Alcohol intake
- Trauma like dislocation or fracture
- Blood disorders
Less obvious but important triggers
- Short term high dose steroids
- Post viral vascular changes
- Poor metabolic health
- Long periods of inactivity (Hernigou et al., 2018)
One important point. Even patients without any major risk factor can develop AVN.
The kind of pain that should make you pause
This is not sharp injury shoulder pain.
Patients describe it like this:
- Deep, dull ache
- Hard to point to exact spot
- Worse at night
- Feels heavy inside the joint
Night pain is one of the biggest red flags.
When you should not ignore it
Get medical evaluation if you notice:
- Pain that wakes you at night regularly
- Sudden increase in stiffness
- Loss of ability to lift your arm
- Pain even at rest
- No improvement after 2 to 3 weeks
Early diagnosis changes outcomes significantly.
Stages of avascular necrosis
You do not need complicated classifications to understand shoulder AVN.
What matters is how the bone is behaving and what you feel during daily life.
Stage 1
No pain. Only visible on MRI.
At this stage, the bone has already started losing its blood supply, but you feel completely normal.
- No pain during activity
- Full shoulder movement
- No weakness
This is usually found accidentally when MRI is done for some other reason.
What is important here is awareness.
If diagnosed at this stage, progression can often be slowed significantly with proper load management and medical care.
Stage 2
Pain begins but feels confusing
This is where most patients start noticing something, but it does not feel serious.
- Mild, deep discomfort
- Feels like muscle strain or gym soreness
- Pain may come and go
- Slight stiffness in certain movements
Many people ignore this stage or treat it like a simple soft tissue issue.
Clinically, this is a critical window.
The bone structure is still intact, which means intervention can be very effective.
Stage 3
Movement reduces and pain becomes more noticeable
Now the condition starts affecting daily life.
- Pain increases with lifting or overhead movement
- Range of motion reduces
- Shoulder feels weak or unreliable
- Difficulty with activities like reaching, dressing, or sleeping on that side
At this stage, the bone has started to lose its structural strength.
Small areas may begin to collapse internally.
This is where physiotherapy becomes very specific.
The goal is to protect the joint while maintaining as much function as possible.
Stage 4
Joint damage and arthritis-like symptoms
This is the advanced stage.
- Constant pain, even at rest
- Significant stiffness
- Grinding or catching sensation
- Clear limitation in daily activities
By now, the surface of the joint is affected, and it behaves like arthritis.
Patients often struggle with simple tasks like combing hair or lifting light objects.
At this stage, conservative treatment helps with pain and function, but surgical options are often considered depending on severity. (Mont et al., 2020)
The biggest mistake people make
They start aggressive exercises too early.
This is risky.
Weak bone + high load = faster damage
I have seen patients worsen simply because they followed random online workouts.
What to do instead
If certain movements increase your pain, do not stop moving completely. Adjust instead.
- Replace overhead lifting with waist-level activities
- Replace gym pressing exercises with wall-supported movements
- Replace heavy resistance bands with very light resistance
- Replace fast movements with slow, controlled motion
- Replace long workouts with short, frequent sessions
The goal is not rest.
The goal is safe movement without overload.
How to treat shoulder avascular necrosis with physiotherapy
There is no one-size plan.
Everything depends on how much load the joint can tolerate.
Quick self-check before you exercise
Ask yourself:
- Does my shoulder hurt at rest today?
- Is my pain increasing compared to yesterday?
- Do I feel sharp pain during movement?
If yes, reduce intensity or rest.
Listen to your body before pushing it.
Phase 1: Reduce stress on the joint
Goal is protection.
- Gentle pendulum movements
- Light isometric exercises
- Avoid overhead lifting
If pain increases after exercise, that is your body telling you to slow down.
Phase 2: Restore movement safely
Once pain settles, we start movement.
- Assisted range of motion
- Gradual active movements
- Focus on shoulder blade control
This stage prevents stiffness and secondary frozen shoulder.
A simple 10-minute shoulder-friendly routine
You can follow this daily:
- 2 minutes pendulum swings
- 2 minutes shoulder blade squeezes
- 2 minutes assisted arm raises (use other hand)
- 2 minutes light band external rotation
- 2 minutes relaxed breathing with posture correction
Keep movements slow and controlled.
No sharp pain. No forcing.
Consistency matters more than intensity.
Phase 3: Strength and control
Now we rebuild function.
- Rotator cuff strengthening
- Scapular stability work
- Low resistance training
Control matters more than weight.
One thing most people do not know
Scapular control plays a major role in recovery.
If the shoulder blade does not move properly:
- Joint stress increases
- Blood flow is affected
- Pain persists
This is often missed in basic exercise routines.
Common mistakes that make avascular necrosis worse
These are things I see very often:
- Starting heavy exercises too early
- Ignoring night pain signals
- Copying generic YouTube workouts
- Pushing through pain thinking it will improve
- Completely stopping movement out of fear
Fixing these alone can prevent progression in many cases.
Pain management beyond medicines
Medicines help, but they are not the full solution.
What works clinically:
- Heat therapy for stiffness
- TENS for pain modulation
- Manual therapy for joint mechanics
These improve comfort and movement together.
How to sleep without increasing pain
Try these:
- Sleep on your back with a pillow under the arm
- If side sleeping, lie on the opposite side
- Place a pillow in front to support the affected arm
- Avoid sleeping directly on the painful shoulder
Small changes in sleep position can reduce night pain significantly.
When surgery becomes necessary
Not every case needs surgery.
But I consider referral when:
- Pain is constant even at rest
- Movement is severely restricted
- Imaging shows progression
Common procedures:
- Core decompression
- Shoulder replacement
Even after surgery, physiotherapy is essential.
Lifestyle changes that actually help
These are simple but powerful.
- Stop smoking
- Limit alcohol
- Maintain healthy weight
- Avoid unnecessary steroid use
These directly affect blood circulation.
How to adjust your daily routine
- Keep frequently used items at chest level
- Avoid repeated overhead reaching
- Take breaks if work involves shoulder use
- Use both hands instead of one when lifting
- Modify desk setup to avoid strain
Daily habits matter more than occasional exercise.
Nutrition and recovery
Diet is often ignored but important.
Focus on:
- Vitamin D
- Calcium
- Omega 3
- Magnesium
Better circulation and reduced inflammation support recovery.
What research is now telling us
Recent clinical understanding highlights:
- Early diagnosis improves outcomes significantly
- Blood supply restoration is key (Mont et al., 2020)
- Conservative management can delay surgery (Hernigou et al., 2018)
What recovery timeline looks like
There is no fixed timeline, but generally:
- Early stage: improvement in 6 to 12 weeks with proper care
- Mid stage: requires consistent management over months
- Late stage: depends on surgery and rehab
Progress is not linear.
Some days feel better, some feel worse. That is normal.
What recovery really looks like
Let’s keep it real.
- Early stage can be managed well
- Mid stage needs consistent care
- Late stage may need surgery
Physiotherapy helps at every stage by improving function and reducing pain.
The mental side people do not talk about
Living with ongoing pain can lead to:
- Fear of movement
- Frustration due to slow recovery
- Anxiety about surgery
This is normal.
Gradual progress and guided rehab help rebuild confidence.
How it actually feels in daily life
Patients often say:
- “I cannot sleep on that side anymore”
- “Reaching overhead feels heavy and restricted”
- “It is not sharp pain, it just feels deep and tiring”
- “Simple things like dressing take effort”
This is not just a physical issue.
It affects confidence in movement.
Final Thoughts
Shoulder avascular necrosis is not the kind of condition most people notice early.
It usually starts quietly.
A little stiffness here, a dull ache there, maybe some discomfort at night that feels easy to ignore.
But the earlier you pay attention to those signals, the better your chances of protecting the joint.
One thing I always tell patients is this:
Do not panic after hearing the diagnosis.
AVN does not automatically mean surgery.
Many people continue working, exercising, and managing daily life well with the right combination of medical care, physiotherapy, and lifestyle changes.
The key is understanding your shoulder instead of fighting against it.
Trying to “push through pain” usually makes things worse.
Smart movement, gradual strengthening, proper load management, and patience matter much more than aggressive exercise.
Recovery also looks different for everyone.
Some improve quickly. Others need long-term management.
What matters is staying consistent and avoiding the cycle of overdoing things on good days and regretting it later.
If your shoulder pain feels deep, persistent, or worse at night, do not ignore it.
Early assessment can make a major difference in preserving joint health and avoiding long-term damage.
Bone damage doesn’t reverse easily, but early action does help.
Start learning how to treat shoulder avascular necrosis today, not when it’s advanced.
And finally, remember this:
Your goal is not just pain relief.
Your goal is keeping your shoulder functional, confident, and usable for years to come.
Frequently Asked Questions
1. Can shoulder avascular necrosis heal naturally?
No. The damaged bone tissue cannot regenerate completely on its own, but early treatment can slow progression and preserve shoulder function.
2. What does shoulder AVN pain feel like?
Most people describe it as a deep, dull ache inside the shoulder. Night pain and pain during overhead movement are common.
3. Is MRI necessary for diagnosis?
Yes. Early-stage AVN often does not appear on regular X-rays. MRI helps detect changes much earlier.
4. Can exercise make AVN worse?
Yes. High-impact or heavy shoulder exercises can increase stress on the weakened bone and worsen the condition.
5. Is physiotherapy helpful for shoulder AVN?
Absolutely. Physiotherapy helps reduce pain, improve movement, maintain muscle strength, and delay joint deterioration.
6. Does every AVN patient need surgery?
No. Many early and moderate cases are managed conservatively with physiotherapy, medication, and lifestyle changes.
7. How long does recovery take?
Recovery varies depending on the stage of AVN. Some people improve within months, while others require long-term management.
Stay tuned with us for more health related topics.
Follow us on LinkedIn and Instagram for more.
Medical Disclaimer!
This article has been reviewed and written under the guidance of our Head Physiotherapist, Dr. Kruti Raj (PT, MUHS,CPT,CMPT). The information shared is intended for educational purposes only and should not be considered a substitute for personalized medical advice, diagnosis, or treatment.
Please consult us or any other qualified healthcare professional before beginning any exercise program, especially if you are experiencing pain, recovering from injury, or managing a medical condition.











