Shoulder dislocation treatment at home?
One wrong move could make it worse, but the right steps might speed up your recovery faster than you expect.
The first time your shoulder dislocates, it feels like a one-time accident.
A fall. A gym mistake. A sports injury.
You get it treated. Shoulder pain reduces. Life goes back to normal.
Then one day, it slips again.
Not during something intense. Sometimes just while reaching, turning, or even sleeping.
That is the moment people realise this is not just an injury. It is a stability problem.
Quick Answer
What is a shoulder dislocation?
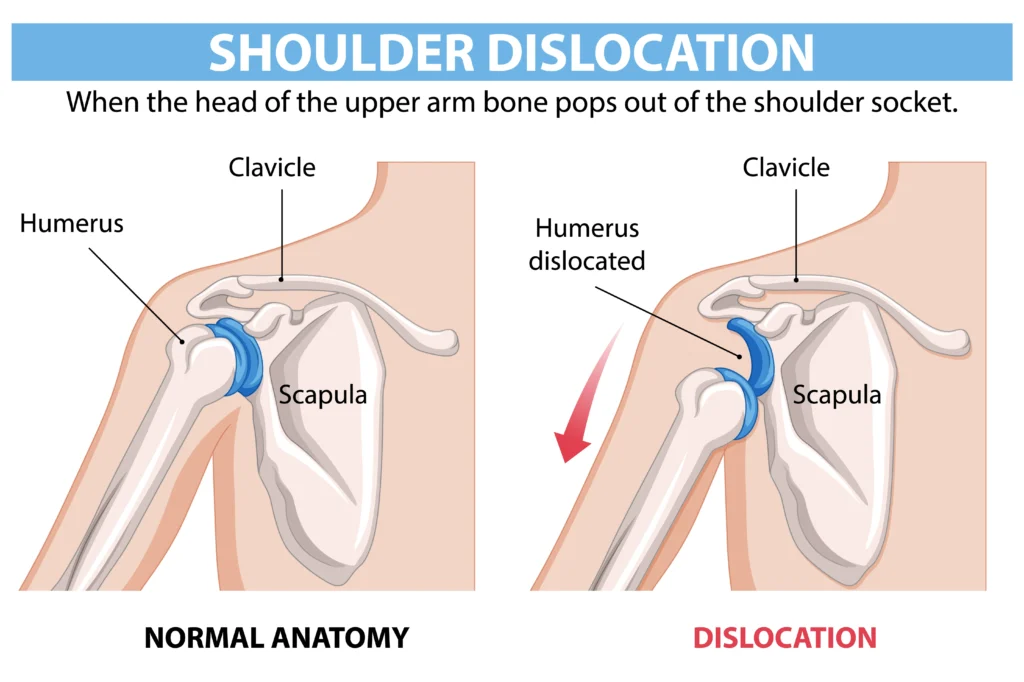
It is when the upper arm bone comes out of its socket, usually due to injury or sudden force.
Will it heal completely?
Yes, but only if proper rehabilitation restores stability, not just pain relief.
Why does it happen again?
Because ligaments become loose and the shoulder loses control, not just strength.
Do I need surgery?
Not always. Many first-time cases recover well with structured physiotherapy.
How long does recovery take?
Basic recovery takes weeks, but full stability can take 3 to 6 months.
Key Takeaways
- Shoulder dislocation is a stability issue, not just a pain problem
- Pain relief does not mean full recovery
- Rehabilitation must include control and coordination training
- Returning too early increases recurrence risk
- Young and active individuals have higher recurrence rates
- Proper physiotherapy can prevent repeat dislocations
What A Shoulder Dislocation Really Is
Your shoulder joint is built for movement, not stability.
The ball of your arm sits in a very shallow socket.
This design allows you to move freely but makes it easier to dislocate.
When a dislocation happens, the ball comes out of the socket.
Most cases are anterior dislocations, where the arm moves outward and backward.
This is not just a position problem. Structures inside the joint get affected immediately.
Was It a Full Dislocation or Just a Slip (Subluxation)?
Not every case is a full dislocation.
Sometimes the shoulder partially slips out and comes back on its own.
That is called a subluxation.
Here’s how people usually describe it:
- “It shifted but came back quickly”
- “I felt a pop but didn’t need hospital”
- “It didn’t look deformed, just painful”
Even if it was a subluxation, don’t ignore it.
It still means your shoulder is unstable.
What Actually Gets Damaged Inside
This is where things become important.
- The labrum, which deepens the socket, often tears
- Ligaments stretch and become loose
- The rotator cuff muscles stop firing properly
- Your brain loses precise control over the joint
The labral injury seen in many dislocations is called a Bankart lesion.
It is strongly linked with recurrent instability (Olds et al., 2015)
There can also be a compression injury on the bone called a Hill Sachs lesion, which further reduces joint stability.
Why Recurrence Is So Common
This is something I explain to almost every patient.
Pain goes away faster than stability returns.
So people assume they are healed when they are not.
Studies have shown that younger individuals, especially under 25, have a very high recurrence rate, sometimes up to 70 to 90 percent depending on activity level (Hovelius et al., 2008)
That is not because the shoulder is weak.
It is because the system controlling the shoulder has changed.
Why Some People Recover Fully and Others Don’t
This is something patients often ask.
Two people can have the same injury but very different outcomes.
The difference usually comes down to:
- How early rehab started
- Whether control training was done
- Returning to activity too soon
- Type of tissue damage
- Activity level
It is not just luck.
It is what you do after the injury.
The Hidden Problem No One Talks About
After a dislocation, your shoulder loses something called proprioception.
In simple terms, your brain becomes less accurate at sensing where your shoulder is in space.
This leads to:
- Delayed muscle activation
- Poor joint control
- A feeling that the shoulder might slip
This is one of the biggest reasons why dislocations repeat, even when strength looks normal.
Research in rehabilitation science continues to highlight the importance of neuromuscular control in preventing recurrence (Warby et al., 2017)
The Fear Factor Is Real
After a dislocation, many people hesitate.
Even simple movements feel risky.
This is not weakness.
Your brain is trying to protect you.
Gradual exposure to movement helps rebuild confidence.
Ignoring this part slows recovery.
What You Might Feel Even After “Recovery”
Patients often describe:
- A sense of looseness
- Fear in overhead positions
- Clicking or shifting
- Avoiding certain movements without thinking
These are not small symptoms. These are signs that stability is not restored.
Pain vs Instability
This confuses a lot of people.
- Pain means irritation or inflammation
- Instability means lack of control
You can have:
- No pain but still unstable
- Mild pain but good stability
If your shoulder feels like it might slip, that matters more than pain.
What Should Be Done Immediately After Dislocation
First step is always reduction by a medical professional.
After that:
- Sling support is usually needed for a short duration, often one to three weeks
- Gentle movement should begin early
- Complete immobilisation for long periods is not helpful
Early controlled movement has been shown to support better outcomes compared to prolonged rest
(Paterson et al., 2010)
How to Sleep Without Irritating Your Shoulder
Sleep is often uncomfortable after this injury.
Try this:
- Sleep on your back with a pillow under your arm
- If side sleeping, lie on the opposite side
- Hug a pillow to support your arm
Avoid letting your arm hang or stretch backward.
Small changes here make a big difference.
The Biggest Mistake People Make
They stop rehab when pain reduces.
This is where the problem starts.
Pain is just one part of recovery. Stability takes much longer.
How Physiotherapy Actually Works When Done Properly
Let me simplify this into phases without making it sound like a textbook.
Early phase
The goal here is simple.
Calm the shoulder down.
Reduce pain. Avoid risky movements. Start gentle mobility.
Nothing aggressive. Nothing fancy.
Activation phase
This is where real work begins.
We focus on small stabilising muscles, especially the rotator cuff and scapular muscles.
Movements are slow and controlled.
This phase is often rushed or skipped, which leads to poor outcomes.
Strength phase
Now we start loading the shoulder.
Resistance bands, controlled strengthening, and gradual increase in range.
But strength alone is not enough.
Control and stability phase
This is the most important and most ignored part.
We train:
- Reaction speed
- Joint awareness
- Control during unpredictable movement
Things like ball drills, perturbation training, and functional movement patterns are used.
This is what actually reduces recurrence.
Rehabilitation programs that include neuromuscular and proprioceptive training show better long term stability (Kirkley et al., 1999)
When Surgery Becomes Necessary
Not everyone needs surgery.
But it becomes more likely if:
- The shoulder dislocates repeatedly
- There is a significant labral tear
- You are involved in high demand sports
- Rehab has been done properly but instability remains
Surgical stabilization, such as arthroscopic Bankart repair, has been shown to reduce recurrence in high risk individuals (Longo et al., 2014)
When Rehab Hits a Limit
Physiotherapy works well in many cases.
But sometimes it is not enough.
Be honest if:
- Shoulder keeps slipping despite rehab
- You avoid movements out of fear
- Strength improves but control does not
In these cases, further evaluation is needed.
Physiotherapy vs Surgery In Simple Terms
Physiotherapy works well for many first time dislocations.
Surgery is considered when instability persists or keeps returning.
Both have a role.
The decision depends on your activity level, age, and how your shoulder responds to rehab.
Returning To Gym Or Sports
This is where patience matters.
- Basic activity can begin in a few weeks
- Strength training usually starts around 8 to 12 weeks
- Full return to sport can take 4 to 6 months
Only return when:
- Strength is restored
- Movement feels controlled
- There is no fear or instability
Before You Go Back to the Gym, Check This
Ask yourself:
- Can I move my arm fully without hesitation?
- Does it feel stable under light load?
- Can I control slow movements easily?
- Do I trust my shoulder again?
If the answer is no, you are not ready yet.
Daily Movements That Can Catch You Off Guard
It is not always gym or sports.
I’ve seen dislocations happen during:
- Reaching into the back seat of a car
- Throwing something casually
- Sudden pulling movements
- Lifting awkward objects
Be mindful during these movements early on.
Things that actually help prevent it from happening again
Keep it simple.
- Strengthen the rotator cuff
- Train scapular control
- Work on joint awareness
- Progress gradually
There is no shortcut here.
Something I tell every patient
After a dislocation, your shoulder is not the same as before.
That does not mean it is damaged forever.
It just means it needs better control than before.
Quick Do’s and Don’ts
Do:
- Keep moving within comfort
- Follow structured rehab
- Focus on control
- Progress gradually
Don’t:
- Rush back to heavy lifting
- Ignore instability feeling
- Skip rehab phases
- Compare your recovery with others
Keep it simple and consistent.
Final Thoughts
If there is one thing I would want you to remember, it is this:
A shoulder dislocation is not just an injury you recover from.
It is a change in how your shoulder behaves.
Pain settles. Movement returns.
But stability needs to be rebuilt.
That part takes effort and patience.
Most repeat dislocations do not happen because the injury was severe.
They happen because recovery was incomplete.
If you take your rehab seriously:
- You can return to gym
- You can play sports again
- You can move without fear
But only if you train your shoulder to be controlled, not just strong.
Do not rush the process. Do not chase quick fixes.
Build stability step by step.
Because in the long run, the goal is simple:
To trust your shoulder again without thinking about it.
Your shoulder won’t fix itself.
Follow the right shoulder dislocation treatment at home now, or risk turning a simple injury into a lifelong problem.”
Frequently Asked Questions
Can a shoulder dislocation heal on its own?
Yes, but without proper rehabilitation it often leads to instability and repeated dislocations.
How do I know if my shoulder is still unstable?
A feeling of slipping, fear during movement, or lack of control are common signs.
Is surgery always required?
No, many cases improve with structured physiotherapy, especially after the first dislocation.
When can I return to the gym?
Usually after 8 to 12 weeks, but only when strength and control are properly restored.
Why does it dislocate again so easily?
Because the stabilizing structures and neuromuscular control are affected after the first injury.
What is the most important part of rehab?
Restoring shoulder control and stability, not just building strength.
Can I avoid surgery completely?
In many cases yes, especially with proper and consistent physiotherapy.
Stay tuned with us for more health related topics.
Follow us on LinkedIn and Instagram for more.
Medical Disclaimer!
This article has been reviewed and written under the guidance of our Head Physiotherapist, Dr. Kruti Raj (PT, MUHS,CPT,CMPT). The information shared is intended for educational purposes only and should not be considered a substitute for personalized medical advice, diagnosis, or treatment.
Please consult us or any other qualified healthcare professional before beginning any exercise program, especially if you are experiencing pain, recovering from injury, or managing a medical condition.











