If you read five different articles about cervical fractures, you will notice something strange. They all sound similar. Same structure, same advice, same simplified explanations.
But in real clinical practice, neck fractures rarely behave in a predictable way.
I have seen patients with severe fractures walking into the clinic with only mild discomfort.
At the same time, I have seen others with relatively small injuries struggling with long-term stiffness and fear of movement.
This difference exists because a cervical fracture is not just a broken bone.
It is a combination of bone injury, ligament involvement, neurological risk, and patient-specific factors.
Recent research is also pointing in the same direction. There is still no single standardized protocol that fits every patient.
Management decisions vary depending on stability, neurological status, and individual health conditions.
Read about our Complete Neck Pain Guide : Causes, Symptoms, Exercises and Treatment
Quick Answer
A cervical (neck) fracture is a break in one of the seven bones of the neck and can range from stable to life-threatening depending on spinal cord involvement. Common symptoms include neck pain, stiffness, numbness, or weakness. Treatment may involve a cervical collar or surgery based on severity. Physiotherapy plays a crucial role in recovery by restoring movement, strength, and function through a structured and gradual rehabilitation process.
Read about: Early Signs of Cervical Spine Damage You Should Never Ignore
Key Takeaways
- Cervical fractures can be serious even if symptoms appear mild initially.
- Pain intensity does not always reflect the severity of the injury.
- Not all neck fractures require surgery; treatment depends on stability and neurological status.
- Early diagnosis and proper imaging are critical for safe management.
- Physiotherapy is essential and must follow a structured, phase-wise approach.
- Starting exercises too early or avoiding movement for too long can delay recovery.
- Each cervical fracture is different, so treatment should always be personalized.
Read about: Cervical Ligament Injury or Neck Ligament Tear
What exactly is a cervical fracture
The cervical spine consists of seven vertebrae from C1 to C7. These bones support the head and protect the spinal cord.
A cervical fracture means a break in one or more of these vertebrae.
But clinically, the injury is rarely limited to bone alone. It may also involve:
Bone disruption
The visible fracture on imaging.
Ligament injury
Often missed initially but critical for stability.
Spinal cord involvement
The most serious component, which can affect movement, sensation, or even breathing.
This is why even a seemingly small fracture needs careful evaluation.
Read about : 15 Common Causes of Neck Pain You Should Know
What recent research tells us about cervical fractures

Modern research has changed how we understand these injuries.
One important finding is that symptoms do not always match severity. (Hsu et al. 2025)
This study described patients with cervical fracture dislocation who had only mild neurological symptoms initially, even though imaging showed significant structural damage.
Another important observation comes from case reports where severe fractures did not immediately cause paralysis. (Li et al. 2024)
This highlights something very important for patients:
A person can still move normally and yet have a serious cervical injury.
Read in detail: Whiplash Injury After An Accident? Here’s Treatment And Expert Rehab Guide
Causes of cervical fractures in real life
While high-speed trauma is a well-known cause, newer data shows a shift.
Road traffic accidents
Still one of the leading causes, especially in countries like India.
Falls
Particularly in older adults. Even low-impact falls can cause fractures due to reduced bone density. (Segi et al. 2024)
This study showed a rising number of cervical fractures in elderly populations.
Sports and recreational injuries
These are becoming more common. (Kuharski et al. 2025)
Recreational activities are increasingly associated with cervical spine fractures.
Read: Burners Syndrome: The Most Ignored Sports Nerve Injury
Symptoms you should not ignore
In clinical practice, I do not rely only on textbook symptoms. I look for patterns.
Common but important signs
- Persistent neck pain after trauma
- Stiffness that does not improve
- Pain that feels deep rather than muscular
- Tingling or numbness in arms
- Weakness in hands or legs
Red flag signs
- Difficulty walking
- Loss of balance
- Loss of bladder or bowel control
One key point many people miss:
Pain intensity does not always indicate severity.
Read more: Cervical Myelopathy: The Hidden Neck Condition Affecting Your Walking
Diagnosis: why imaging matters more than symptoms
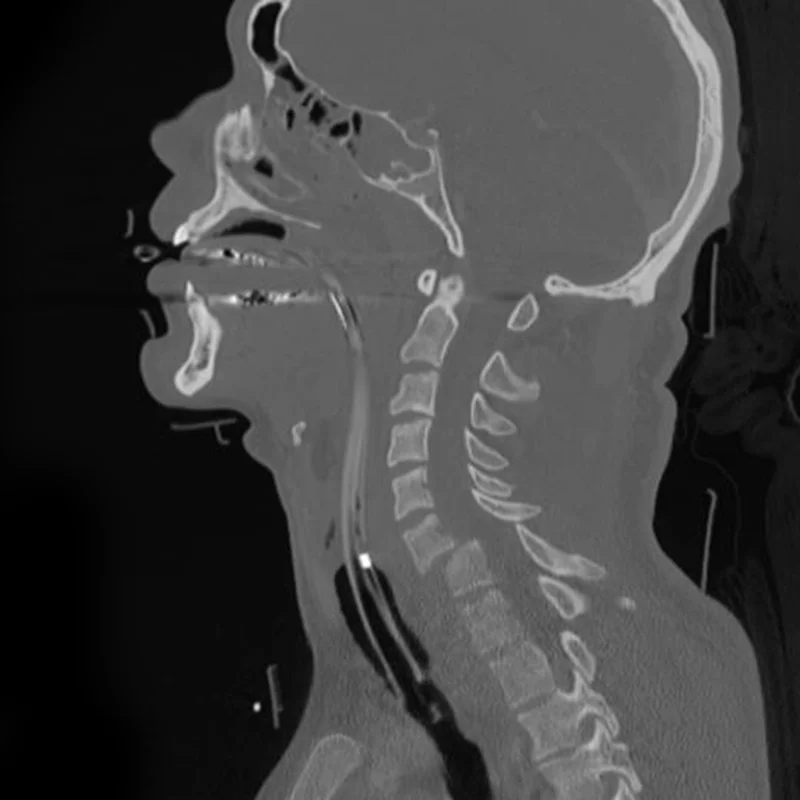
Cervical fractures are frequently underdiagnosed if only clinical symptoms are considered.
X-ray
Useful but may miss subtle injuries
CT scan
Gold standard for bone assessment
MRI
Essential when:
- neurological symptoms are present
- ligament injury is suspected
Recent advances also include AI-based detection systems that improve fracture identification accuracy. (Singh et al. 2025)
AI-assisted tools are being developed to support early and accurate diagnosis.
Read in detail about: What is Cervical Spondylosis? The Truth Behind Chronic Neck Pain
Treatment: not as fixed as people think
One of the biggest misconceptions is that all cervical fractures require surgery.
That is not true.
Conservative treatment
Used when:
- fracture is stable
- no neurological deficit
Includes:
- cervical collar
- rest
- gradual rehabilitation
Surgical treatment
Required when:
- fracture is unstable
- spinal cord is at risk
Recent research suggests that outcomes may not always differ significantly between surgical and non-surgical management in selected patients. (BMC Musculoskeletal Disorders 2025)
Treatment decisions depend more on patient condition than a fixed rule.
Read: What is Torticollis? How to treat neck tilt condition
Timing of treatment matters more than many realize
Another critical factor is timing. Quinteros et al. 2025
Delays in surgical stabilization can affect recovery outcomes.
In simple terms:
Early correct management often matters more than the type of treatment itself.
Read about: Effective Neck Pain Exercises At Home: A Complete Guide to Relief and Improved Mobility
Physiotherapy Treatment
This is the stage where most of the real recovery happens, yet it is also the part people misunderstand the most.
Many patients come in expecting a list of exercises. Some even say, “Just tell me which movements to do and I’ll start at home.”
But physiotherapy after a cervical fracture is not about jumping into exercises. It is about timing, control, and progression.
The neck is not like other joints. You are dealing with a region that protects the spinal cord, supports the head, and coordinates with the entire upper body.
So the goal is not just movement. The goal is safe movement with stability.
Let me walk you through how this actually progresses in real practice.
Read: Neck Pain from Poor Breathing Pattern? Correct Now!
Phase 1: Protection phase
This phase is often mistaken for complete rest, but that is not entirely true.
Yes, the neck needs protection. Movement is either restricted or very minimal depending on medical advice.
But that does not mean the body should become inactive.
At this stage, the focus is on:
- Maintaining neck stability using prescribed support such as a cervical collar if advised
- Teaching the patient how to move safely without putting strain on the neck
- Breathing exercises, which are more important than most people realize because shallow breathing is very common after injury
- Gentle movements of the shoulders, arms, and even legs to prevent stiffness and improve circulation
One thing I always tell patients here is this:
“You are not resting completely. You are recovering intelligently.”
Read: How To Use Cervical Collar for Neck Support: Benefits & Hidden Risks
Phase 2: Controlled activation
Once the doctor clears basic movement, we begin very subtle activation.
This is where many patients feel confused. They expect visible movement, but most of the work in this phase is almost invisible.
We focus on:
- Gentle activation of deep neck muscles without forcing movement
- Small, controlled motions within a safe range
- Learning how to move without triggering pain or fear
The key here is control, not intensity.
Large movements, stretching, or sudden rotations are avoided. The idea is to “wake up” the muscles again without disturbing healing structures.
Patients often say, “It feels like I’m not doing much.” But this is exactly where the foundation is built.
Also Read: Ultimate 6 Weeks Neck Rehabilitation Exercises For Pain Relief
Phase 3: Strength rebuilding
Now we gradually move into strengthening, but even here, it is not about aggressive exercise.
The neck relies heavily on small stabilizing muscles that are often weak after immobilization.
So we target:
- Deep cervical stabilizers, which support the spine internally
- Scapular muscles, because the shoulder blades play a big role in reducing neck strain
- Postural muscles that help maintain alignment during daily activities
This phase also includes correcting habits.
For example:
- How you sit
- How you use your phone
- How long you stay in one position
Strength without awareness does not help much. Both need to go together.
Read about: Which Is The Best Sitting Posture To Avoid Neck Pain And How To Achieve It
Phase 4: Functional recovery
This is where recovery becomes practical.
By now, patients usually feel better, but they are not fully confident yet. That confidence needs to be rebuilt.
So we focus on:
- Training movements used in daily life, like turning the head while walking or looking up
- Gradually returning to work-related tasks
- Improving coordination between neck, shoulders, and upper back
This phase is less about “exercise” and more about real-life movement.
Because at the end of the day, recovery is not about how well you perform in the clinic. It is about how comfortably you live your daily life.
Read: Burners Syndrome: The Most Ignored Sports Nerve Injury
What many patients get wrong
This part comes directly from experience. These are patterns I see again and again.
Starting exercises too early
This is probably the most common mistake.
Patients feel slightly better and assume healing is complete. They begin neck movements, stretches, or even strengthening without proper guidance.
The problem is that bone healing and ligament healing take time. Just because pain has reduced does not mean the structure is stable.
Starting too early can:
- Increase instability
- Delay healing
- Sometimes worsen the condition
Recovery is not about speed. It is about timing.
Avoiding movement for too long
On the opposite side, some patients become overly cautious.
They avoid moving their neck completely, even after being cleared to start rehabilitation. This often comes from fear.
“I don’t want to damage it again.”
While the intention is understandable, prolonged avoidance creates a different problem:
- Joint stiffness
- Muscle weakness
- Reduced confidence in movement
This is where guided physiotherapy becomes important. You need to know when to protect and when to move.
Following random online advice
This is something I see more frequently now.
Patients search online and start doing exercises they find on videos or blogs. The issue is not that exercises are wrong. The issue is that they are not tailored.
Every cervical fracture is different:
- Different levels
- Different stability
- Different recovery stages
An exercise that is safe for one person may not be safe for another.
So instead of helping, this often leads to confusion or setbacks.
Summary
If I had to simplify everything into one line, I would say:
Recovery after a cervical fracture is a balance between protecting too much and pushing too early.
The right path is always somewhere in between, guided step by step.
Read about: How to Relieve Morning Neck Stiffness Naturally
Lesser known facts that most articles miss
Not all fractures cause immediate paralysis
Some patients remain neurologically stable initially.
Ligament damage is often more serious than bone injury
But it is not always visible early.
Recovery is not linear
Good days and bad days are normal.
Fear of movement slows recovery
This is called kinesiophobia and is very common.
Read: Spasm In Neck: What Causes It & How to Fix It Fast
Long-term complications
Even after healing, some patients may experience:
- chronic neck pain
- reduced mobility
- muscle weakness
- early degeneration
Risk increases with age and associated conditions.
Read in detail about: Cervical Disc Degeneration: The Hidden Cause of your Neck Pain
Prevention that actually works
Daily habits
- maintain proper posture
- avoid prolonged screen time
Travel safety
- always use seat belts
- adjust headrest properly
For elderly individuals
- focus on bone health
- reduce fall risk
Read more: Heat Or Cold Therapy for Neck Pain: What Actually Works?
What I tell my patients honestly
I usually simplify everything into three points:
- Do not panic, but do not ignore symptoms
- Do not rush recovery
- Do not delay proper rehabilitation
Most people recover well when managed correctly.
Read more: Is Cervical Traction For Neck Pain Really Effective
Conclusion
Cervical fractures are serious, but they are not always catastrophic.
The outcome depends on:
- early diagnosis
- correct treatment choice
- structured physiotherapy
- patient awareness
And most importantly, not treating every patient in the same way.
Also Read : Neck Cracking: Benefits, Risks, and the Truth About Stroke
Frequently Asked Question
Q1. Can a cervical fracture heal without surgery?
Yes, stable cervical fractures can heal with immobilization using a cervical collar along with proper medical supervision and physiotherapy.
Q2. How long does it take to recover from a neck fracture?
Bone healing usually takes 6 to 12 weeks, while complete recovery including strength and movement may take several months.
Q3. When should physiotherapy start after a cervical fracture?
Physiotherapy should only begin after the fracture is stabilized and cleared by a doctor to avoid complications.
Q4. Can I move my neck after a cervical fracture?
Neck movement should be avoided initially. Gradual movement is introduced only under professional guidance during rehabilitation.
Q5. What are warning signs of a serious cervical fracture?
Numbness, weakness, difficulty walking, or loss of bladder and bowel control are serious signs and require immediate medical attention.
Q6. Can symptoms appear later after a neck injury?
Yes, some neurological symptoms may develop days or even weeks after the injury.
Q7. What is the biggest mistake during recovery?
Starting exercises too early or completely avoiding movement for too long can both delay proper recovery.
Stay tuned with us for more health related topics.
Follow us on LinkedIn and Instagram for more.
Medical Disclaimer!
This article has been reviewed and written under the guidance of our Head Physiotherapist, Dr. Kruti Raj (PT, MUHS,CPT,CMPT). The information shared is intended for educational purposes only and should not be considered a substitute for personalized medical advice, diagnosis, or treatment.
Please consult us or any other qualified healthcare professional before beginning any exercise program, especially if you are experiencing pain, recovering from injury, or managing a medical condition.











