Whiplash injury is one of the most misunderstood neck injuries. Many people assume it is a minor problem that resolves quickly, while others fear it may cause permanent damage.
In reality, whiplash lies somewhere between these extremes. For some individuals it resolves within weeks, while for others it can lead to persistent pain and disability.
From a physiotherapist’s perspective, early understanding and proper rehabilitation play a crucial role in recovery.
When managed correctly, most patients can regain normal neck mobility and return to daily activities without long-term complications.
Read about neck pain in our Detailed Guide to Neck Pain: Causes, Symptoms, Exercises and Treatment
Understanding Whiplash Injury
Whiplash is a neck injury caused by a sudden acceleration-deceleration movement of the cervical spine. This motion forces the neck to rapidly bend backward and then forward, similar to the cracking motion of a whip.
Most commonly, this occurs during road traffic accidents, particularly rear-end collisions. However, whiplash can also occur in sports injuries, falls, or physical assaults.
Medical professionals often use the term Whiplash Associated Disorders (WAD) to describe the wide range of symptoms that follow this injury. These symptoms may include neck pain, stiffness, headaches, dizziness, and sometimes cognitive disturbances. (Eexot Journal)
The cervical spine is highly mobile and supported by muscles, ligaments, and discs. During whiplash trauma, these structures may experience micro-tears, inflammation, and joint irritation.
Epidemiology and Prevalence

Whiplash injuries are extremely common worldwide.
Studies estimate that millions of people experience whiplash each year, particularly due to motor vehicle accidents.
In fact, research suggests that approximately 93 percent of patients diagnosed with whiplash fall under Grade II classification, meaning they have neck pain along with reduced range of motion and musculoskeletal signs. (British Journal of Sports Medicine)
Another important finding from research is that recovery patterns vary widely. Some individuals recover within weeks, while 40 to 60 percent of patients may develop chronic symptoms lasting several months or even years. (PubMed)
These numbers highlight why early physiotherapy intervention is essential.
Mechanism of Injury
To understand whiplash, it is helpful to visualize what happens inside the neck during impact.
When a car is hit from behind:
- The torso is pushed forward by the seat.
- The head momentarily stays behind due to inertia.
- The neck bends backward into hyperextension.
- Immediately afterward, the head snaps forward into hyperflexion.
This rapid motion can damage several structures:
- Cervical facet joints
- Intervertebral discs
- Ligaments
- Neck muscles
- Nerve roots
- Joint capsules
Interestingly, many whiplash injuries involve microscopic soft tissue damage rather than visible structural injury on imaging, which is why X-rays often appear normal.
Classification of Whiplash Injury
Doctors classify whiplash injuries using the Quebec Task Force grading system, which helps guide treatment.
Grade 0
No symptoms or physical signs.
Grade I
Neck pain, stiffness, or tenderness but no physical signs.
Grade II
Neck complaints with musculoskeletal signs such as reduced movement or tenderness.
Grade III
Neurological symptoms such as numbness, weakness, or altered reflexes.
Grade IV
Fracture or dislocation of the cervical spine.
Most patients fall within Grade I or II, which usually respond well to conservative treatment including physiotherapy.
Read in detail about: Cervical Disc Degeneration: The Hidden Cause of your Neck Pain
Common Symptoms of Whiplash Injury
Symptoms may appear immediately after the accident or may develop gradually over 24 to 48 hours.
Common symptoms include:
Neck pain and stiffness
The most typical symptom caused by muscle strain and joint irritation.
Headaches
Usually originating from the base of the skull due to tension in suboccipital muscles.
Reduced neck mobility
Patients often report difficulty turning the head or looking upward.
Shoulder and upper back pain
Muscle tension spreads to surrounding areas.
Dizziness and balance disturbances
This occurs due to cervical proprioception disturbances.
Fatigue and concentration difficulties
Some individuals develop cognitive symptoms.
Tingling or numbness in arms
This may indicate nerve root irritation.
Read in detail about: Cervical Radiculopathy: Why Neck Nerve Pain Travels to the Arm
As physiotherapists, we always evaluate these symptoms carefully to rule out serious complications.
Read about : 15 Common Causes of Neck Pain You Should Know
Lesser Known Facts About Whiplash
1. Symptoms can appear days later
Many patients feel normal immediately after the accident but develop pain after 24 to 72 hours.
2. Stress influences recovery
Psychological factors such as fear of movement and anxiety can delay recovery.
3. Imaging often looks normal
Soft tissue injuries may not appear on X-rays or MRI scans.
4. Women are at higher risk
Studies suggest females may have increased susceptibility due to lower neck muscle mass.
5. Muscle dysfunction can persist
Even after pain improves, deep neck muscles may remain weak.
These hidden factors explain why rehabilitation must focus on both physical and psychological recovery.
Scientific Insights About Whiplash Injury
1. Deep Neck Muscles Can Stay Dysfunctional for Years
Recent research using ultrasound imaging found that people with chronic whiplash often have altered function in the deepest layers of neck muscles, even years after the injury.
These muscles show reduced movement and coordination during neck rotation. Interestingly, targeted neck-specific exercises over several months can significantly improve this muscle function. (PubMed)
This explains why some patients continue to experience neck pain long after the accident if rehabilitation is incomplete.
2. Whiplash Can Affect Jaw Function
One surprising finding from recent research is that jaw movement and neck movement are closely linked. Studies have shown that people with whiplash injuries may develop altered jaw-neck coordination even two years after the trauma. (PubMed)
This is why some patients with whiplash complain about:
- jaw tightness
- difficulty chewing
- clicking in the jaw joint
Physiotherapists sometimes include jaw relaxation and neck coordination exercises to address this connection.
3. Whiplash Can Disturb Your Neck’s “Position Sense”
The cervical spine has a highly sensitive proprioceptive system that tells your brain where your head is positioned in space.
After a whiplash injury, this system may become impaired, leading to poor head-position accuracy and symptoms like dizziness or balance problems. (PubMed)
Rehabilitation programs that include sensorimotor training and head repositioning exercises can help restore this system.
4. Chronic Whiplash May Affect the Brain
Recent neuroimaging studies show that chronic whiplash pain may be associated with changes in gray matter in certain brain regions involved in pain modulation.
The encouraging news is that these changes may partially reverse after proper treatment and rehabilitation. (ScienceDirect)
This finding highlights that persistent whiplash pain is not just “in the neck” but involves the nervous system as well.
5. The Tongue May Help Stabilize the Neck
A fascinating recent study found that placing the tongue gently against the roof of the mouth may increase activation of deep neck stabilizing muscles. (PubMed)
Some physiotherapists now use this technique during deep neck flexor exercises to improve cervical stability.
How Whiplash Is Diagnosed
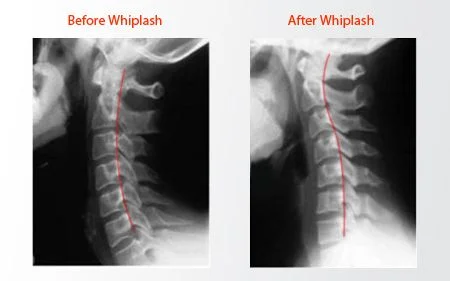
Diagnosis primarily relies on clinical examination.
Doctors and physiotherapists assess:
- Range of neck movement
- Muscle tenderness
- Neurological function
- Posture and muscle control
Imaging tests may be used if severe injury is suspected.
X-ray
To rule out fractures.
MRI
To evaluate soft tissue or nerve damage.
CT scan
Used in cases of severe trauma.
In most cases, however, diagnosis is based on symptoms and physical findings.
Physiotherapy Assessment
A physiotherapy evaluation is essential for designing the correct rehabilitation program.
The assessment typically includes:
Pain analysis
Location, severity, and aggravating factors.
Range of motion testing
Flexion, extension, rotation, and side bending.
Muscle strength evaluation
Particularly deep cervical flexors.
Postural analysis
Forward head posture often worsens symptoms.
Functional movement testing
Activities such as driving or desk work.
This detailed assessment helps identify underlying movement dysfunction.
Read about: Effective Neck Pain Exercises At Home: A Complete Guide to Relief and Improved Mobility
Physiotherapy Treatment for Whiplash Injury

Physiotherapy plays a central role in recovery from whiplash.
Research suggests that active physiotherapy interventions can improve pain levels and range of movement in patients with whiplash-associated disorders. (BMJ Open)
Treatment usually progresses in phases.
Phase 1: Pain Control and Protection
During the first few days after injury, the focus is on reducing pain and inflammation.
Common strategies include:
Gentle neck movements
Early movement helps prevent stiffness.
Ice therapy
Helps reduce inflammation.
Postural advice
Avoid prolonged forward head posture.
Education
Patients are reassured that recovery is possible.
Previously, doctors recommended cervical collars, but modern research discourages prolonged immobilization.
Phase 2: Restoring Mobility
Once pain begins to reduce, mobility exercises are introduced.
Examples include:
Neck rotation exercises
Slowly turning the head side to side.
Chin tuck exercise
Strengthens deep cervical muscles.
Learn How to do Chin Tucks for Neck Pain Relief and Posture Correction
Shoulder rolls
Reduce tension in surrounding muscles.
Thoracic mobility exercises
Improve spinal alignment.
The goal is gradual restoration of normal neck movement.
Phase 3: Strengthening the Neck
Strengthening exercises are critical to prevent chronic pain.
Important exercises include:
Deep neck flexor training
Activates stabilizing muscles.
Scapular strengthening
Improves shoulder and neck coordination.
Isometric neck exercises
Improve muscle endurance.
Resistance band exercises
Enhance cervical stability.
These exercises restore functional strength.
Phase 4: Functional Rehabilitation
The final stage focuses on returning to normal daily activities.
This may include:
- Ergonomic training
- Work posture correction
- Driving posture advice
- Sport-specific training
The aim is full functional recovery.
Simple Posture Correction Exercises for Forward Head Posture
New and Emerging Treatments
Modern research is exploring several new approaches to whiplash rehabilitation.
Behavioral physiotherapy
Combining physical exercises with psychological support may improve recovery outcomes and prevent chronic pain development. (PubMed)
Multidisciplinary treatment
Programs involving physiotherapists, psychologists, and physicians have shown promising results in improving recovery. (PubMed)
Neuromuscular training
Exercises targeting deep cervical stabilizers may improve motor control.
These newer approaches highlight the importance of holistic rehabilitation.
Possible Complications
Although most people recover well, some may develop chronic symptoms.
Possible complications include:
Chronic neck pain
Persistent discomfort lasting months.
Cervicogenic headaches
Headaches originating from neck joints.
Read about : What is Cervical Facet Joint Pain, how it causes cervicogenic headaches and how to correct it naturally
Reduced neck mobility
Due to muscle stiffness.
Postural dysfunction
Forward head posture worsens symptoms.
Psychological distress
Anxiety and fear of movement.
Early physiotherapy significantly reduces these risks.
Learn About: The Ultimate Neck Stretch Routine for Desk Workers in 2026
Prevention Tips
While not all accidents can be prevented, certain strategies reduce injury risk.
Proper car seat positioning
Headrests should align with the back of the head.
Strengthening neck muscles
Strong muscles improve shock absorption.
Maintaining good posture
Reduces strain on cervical spine.
Safe driving practices
Prevent rear-end collisions.
Prevention strategies are especially important for individuals who drive frequently.
When to Seek Medical Help
Immediate medical attention is required if symptoms include:
- Severe neck pain
- Loss of arm strength
- Persistent numbness
- Difficulty walking
- Severe headaches
These may indicate serious spinal injury.
Clinical Insight
In clinical practice, one of the most common mistakes patients make after whiplash is complete rest.
While rest may help for a day or two, prolonged inactivity actually slows recovery. Gentle, guided movement is essential for restoring normal neck function.
Many patients also underestimate the importance of posture. A forward head posture can double the load on the cervical spine and prolong pain.
Physio Prescription (Evidence-Based Whiplash Exercise Routine)
Modern physiotherapy guidelines recommend early controlled movement and neck muscle activation rather than prolonged rest after a whiplash injury.
Research shows that strengthening the deep cervical muscles and improving posture can significantly reduce pain and disability in patients with whiplash-associated disorders.
You can begin this simple routine once acute pain starts settling. Perform the exercises once or twice daily, keeping movements gentle and controlled.
1. Deep Neck Nod (Cranio-Cervical Flexion)

Lie on your back with a small pillow under your head. Gently nod your head as if saying “yes,” without lifting it off the pillow. Hold for 5 seconds.
Repeat 10 times.
2. Neck Isometric Strengthening

Sit upright and place your palm on your forehead. Gently press your head against your hand without allowing movement. Hold for 5 seconds.
Repeat 5 times, then perform the same resistance to the back and sides of the head.
3. Chin Retraction (Posture Correction)
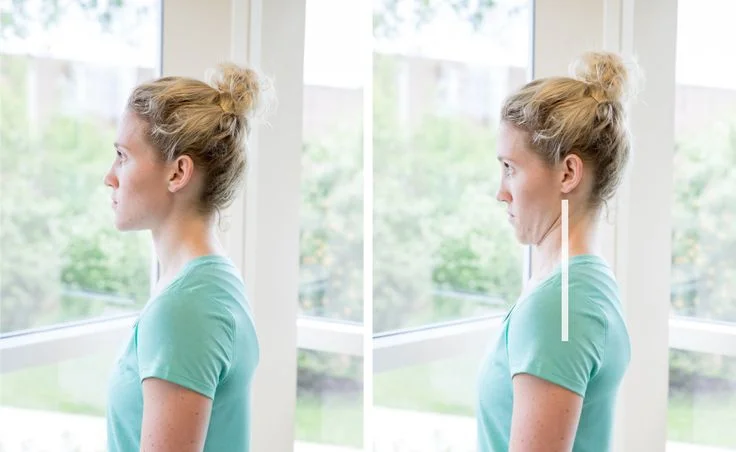
Sit or stand straight. Slowly pull your chin backward to create a small “double chin.” Keep your eyes level and shoulders relaxed.
Hold for 5 seconds and repeat 10 times.

Sit upright and gently squeeze your shoulder blades together without lifting your shoulders.
Hold for 5 seconds and repeat 10 times.
5. Gentle Neck Rotation

Slowly turn your head to the right as far as comfortable, then return to center. Repeat to the left.
Perform 10 repetitions on each side.
These exercises help restore neck mobility, improve muscle coordination, and support cervical spine stability, which are key goals in whiplash rehabilitation according to physiotherapy research and clinical guidelines.
Important: Stop the exercises and consult a physiotherapist if you experience increasing arm numbness, severe dizziness, or sharp radiating pain.
Red Flags
Consult a doctor immediately if you notice:
- Progressive arm weakness
- Loss of sensation in arms
- Severe dizziness
- Difficulty swallowing
- Severe headaches after trauma
These symptoms may indicate serious neurological involvement.
Common Myth
Myth: Wearing a cervical collar helps whiplash heal faster.
Reality: Modern research shows that prolonged use of cervical collars may delay recovery by weakening neck muscles. Gentle movement and physiotherapy are more effective.
Clinical Takeaway
Whiplash is not simply a muscle strain. It can involve neuromuscular control, proprioception, jaw-neck coordination, and even brain pain pathways, which is why a structured physiotherapy rehabilitation program is essential for complete recovery.
Frequently Asked Questions (FAQs)
1. How long does it take to recover from a whiplash injury?
Most mild to moderate whiplash injuries improve within 2 to 6 weeks with proper care and physiotherapy. However, some people may experience symptoms for several months. Early movement, posture correction, and guided exercises can significantly speed up recovery.
2. What are the first symptoms of whiplash injury?
The most common early symptoms include neck pain, stiffness, headaches at the base of the skull, reduced neck movement, and shoulder discomfort. In some cases, symptoms may appear several hours or even a day after the accident.
3. Can whiplash heal on its own?
Mild whiplash injuries may improve naturally over time. However, physiotherapy is often recommended to restore neck strength, improve posture, and prevent long-term complications such as chronic neck pain.
4. What exercises help recovery from whiplash?
Gentle exercises such as chin tucks, neck rotations, deep neck flexor activation, and shoulder blade squeezes are commonly recommended in physiotherapy programs. These exercises help restore neck stability and mobility.
5. When should I see a doctor after a whiplash injury?
You should seek medical attention if you experience severe neck pain, numbness in the arms, dizziness, difficulty moving the neck, or worsening headaches after a car accident or trauma.
Final Word
Whiplash injury may seem frightening, especially after a car accident. However, with the right approach, most patients recover fully.
The key principles are early movement, physiotherapy-guided rehabilitation, posture correction, and gradual strengthening.
As physiotherapists, our goal is not only to reduce pain but also to restore confidence in movement. When patients understand their injury and actively participate in rehabilitation, recovery becomes faster and more complete.
Stay tuned with us for more health related topics.
Follow us on LinkedIn and Instagram for more.
Medical Disclaimer!
This article has been reviewed and written under the guidance of our Head Physiotherapist, Dr. Kruti Raj (PT, MUHS,CPT,CMPT). The information shared is intended for educational purposes only and should not be considered a substitute for personalized medical advice, diagnosis, or treatment.
Please consult us or any other qualified healthcare professional before beginning any exercise program, especially if you are experiencing pain, recovering from injury, or managing a medical condition.











