If you walked out thinking, “why didn’t my physio give me exercises?”, you’re not alone.
It’s one of the most common questions patients have after their first session.
You walked in with a headache. You expected exercises.
You got assessment, maybe some hands-on work, maybe advice.
And somewhere in your mind, a thought came up:
“Why didn’t we start actual treatment?”
Here is the reality.
We did start treatment.
Just not the part you were expecting.
Quick Answer
Your physiotherapist didn’t start exercises immediately because your body may not have been ready for it yet. Headaches often involve sensitivity in the neck and nervous system, and starting exercises too early can actually worsen symptoms.
In the early phase, physiotherapy focuses on understanding the cause, reducing pain, and preparing your body. Exercises are introduced later when your system can tolerate them better, making them more effective and safer.
Key Takeaways
- Headaches are not always caused by muscles or posture alone
- Starting exercises too early can sometimes worsen symptoms
- Initial sessions focus on assessment and reducing sensitivity
- Manual therapy and education often come before exercises
- Each headache type requires a different treatment approach
- Exercises are most effective when introduced at the right time
- Good physiotherapy is based on timing, not speed
What most patients expect vs what actually happens
Let’s be real for a second.
Most people walk into physio thinking:
- “I’ll get 4-5 exercises”
- “I’ll start fixing this today”
- “More exercises = faster recovery”
But here’s what actually happens in a good session:
- You’re asked detailed questions
- Your neck is assessed in different ways
- Treatment feels slow or minimal
And that gap between expectation and reality is where confusion starts.
Headache treatment is not exercise-first
Most people associate physiotherapy with exercises from day one.
That works well for:
- knee rehab
- shoulder injuries
- post-surgical recovery
But headaches do not behave like that.
Because headache is rarely just:
- a tight muscle
- a weak neck
- or bad posture
It is usually a mix of:
- joint sensitivity
- muscle overactivity
- nervous system involvement
And if we rush into exercises at this stage, we often irritate the system more than we help it.
What happens in first physiotherapy session
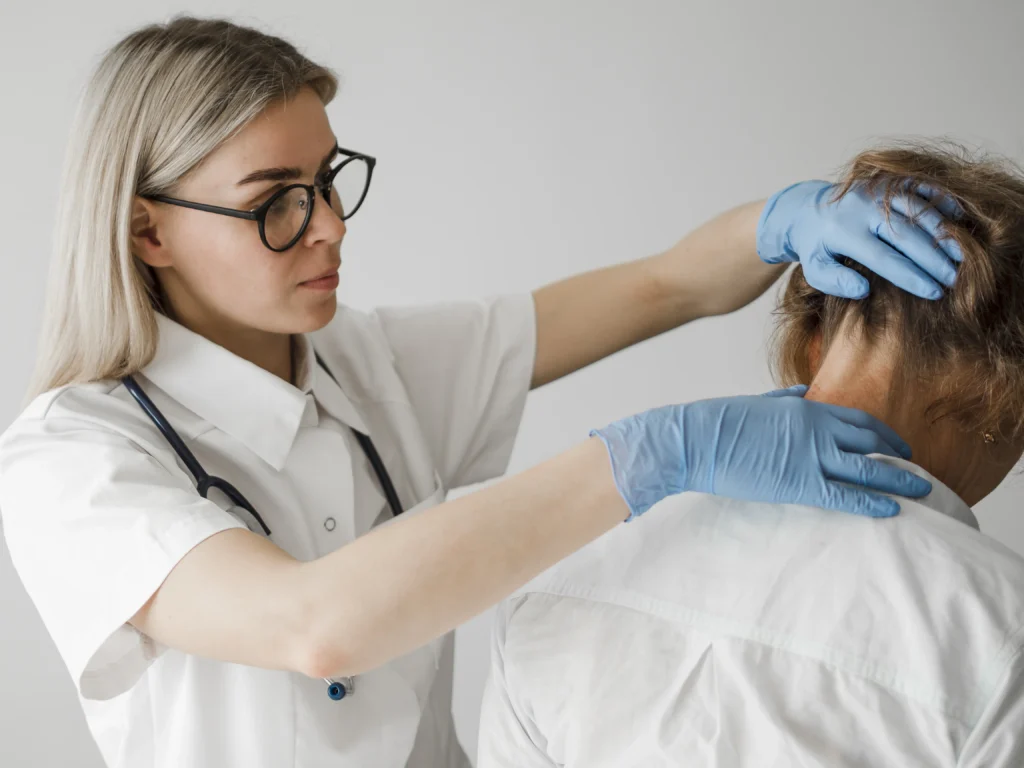
Your first session is not about fixing. It is about understanding.
A physiotherapist is trying to answer:
- Is your headache coming from the neck
- Is your system highly sensitive
- Are there any warning signs
- What movements trigger or relieve symptoms
This is not routine questioning. This is clinical reasoning.
Without this step, exercises become guesswork.
Not all headaches are treated the same way
Two people can point to the same spot on their head and still need completely different treatment.
That’s because the source of the headache is often not where you feel the pain.
In clinic, we usually look at patterns rather than just location.
Common patterns we see
This type comes from the neck.
Pain often starts at the base of the skull and can travel to the forehead or behind the eyes.
You may notice:
- stiffness in the neck
- pain with certain neck movements
- one-sided headache
In these cases, treatment focuses more on:
- joint mobility
- muscle control
- movement correction
This is the most common type.
It often feels like:
- a tight band around the head
- pressure rather than sharp pain
- heaviness at the end of the day
Here, the problem is not just muscles.
It often involves stress, fatigue, and nervous system sensitivity.
Treatment may include:
- relaxation strategies
- load management
- gentle movement, not aggressive exercise
Migraine with neck involvement
Many people with migraine also have neck symptoms.
But this does not mean the neck is the main cause.
You might experience:
- throbbing pain
- sensitivity to light or sound
- nausea
- neck stiffness before or during an episode
In these cases:
- physiotherapy supports the condition
- but does not replace medical management
The focus is on:
- reducing triggers
- improving neck tolerance
- managing flare-ups
Mixed patterns
This is more common than people think.
A patient may have:
- a primary headache (like migraine)
- plus a secondary neck component
So some days it behaves like a migraine and other days it feels like a neck-driven headache
This is why treatment needs to adapt over time.
Why this matters more than you think
Research shows that many chronic and tension-type headaches involve increased sensitivity in the nervous system. (Bendtsen et al. 2010)
This means your pain is not just about:
- tight muscles
- or joint stiffness
It is also about how your brain and nervous system are processing signals.
What this changes in your treatment
Because of this, treatment is not just:
- stretch this
- strengthen that
Instead, it may include:
- calming the nervous system
- improving movement gradually
- reducing triggers
- building tolerance step by step
Simple way to understand it
Think of it like this:
Two people feel pain in the same area; but one has a “mechanical issue” and the other has a “sensitivity issue”
If both are given the same exercises, only one will improve
The other may actually feel worse
That’s why your plan is different
So if your physiotherapist:
- takes time to assess
- does not rush into exercises
- changes your treatment over sessions
That is not inconsistency.
That is individualized care.
Red flags you should not ignore
Some headaches need medical attention first.
Watch for:
- sudden severe headache unlike before
- dizziness or visual disturbances
- numbness or weakness
- headache after trauma
If you notice these, your physiotherapist may delay treatment and refer you further.
That is the correct approach.
Why physio doesn’t start exercises immediately
Why exercises are sometimes delayed
1. Your system may be too reactive
If small movements:
- increase your headache quickly
- or cause symptoms to linger for hours
then your system is in a high irritability state.
In this phase:
- even correct exercises can feel wrong
- recovery becomes slower
So we first reduce sensitivity before adding load.
2. Pain needs to settle before strengthening
If your neck is:
- stiff
- painful
- overloaded
and we immediately add exercises, your body compensates.
Instead of improving, it reinforces the problem.
That is why we often begin with:
- gentle movement
- manual therapy
- relaxation strategies
3. Manual therapy is not “just temporary relief”
Many patients think hands-on treatment is only for short-term relief.
But in reality, it prepares your body for exercise. (Jull et al. 2002)
This study showed that combining manual therapy with exercise is more effective than exercise alone for cervicogenic headache.
So when your physio uses hands-on techniques first, they are not delaying treatment. They are setting it up properly.
4. Your muscles may not be weak. They may be overworking
This is something most people do not expect.
In headache patients, we often see:
- overactive upper trapezius
- tight suboccipital muscles
- poor deep neck control
If we jump into strengthening:
- we train the wrong muscles
- symptoms continue
So first we improve control. Then we build strength.
A quick real-life example
A patient came in with daily headaches.
She had already tried:
- neck exercises from YouTube
- stretching multiple times a day
Her pain kept increasing.
We stopped all exercises initially.
Focused on:
- reducing muscle overactivity
- improving movement tolerance
After 2 sessions, her headache frequency dropped.
Only then we started targeted exercises.
That’s the difference timing makes.
When exercises can start early
Not every case needs delay.
Exercises may start early if:
- pain is mild and stable
- movement does not worsen symptoms
- the headache is not highly sensitive
- the patient tolerates activity well
In these cases, early movement can actually speed recovery.
So it’s not about delaying. It’s about choosing the right timing.
The role of your brain in headache
This is where modern physiotherapy has evolved.
Pain is not always equal to damage.
In many headache cases, the nervous system becomes more sensitive over time. (Louw et al. 2016)
Pain education has been shown to improve outcomes in musculoskeletal conditions.
So when your physiotherapist explains your condition, that is not filler. It is treatment.
It reduces fear, improves confidence, and helps your system calm down.
What is actually happening in early sessions
It may feel like very little is happening.
But clinically, a lot is being done.
| What you notice | What your physio is doing |
|---|---|
| Asking questions | Identifying headache type |
| Checking movement | Understanding triggers |
| Touching muscles | Finding pain sources |
| Gentle techniques | Reducing sensitivity |
| Advice | Removing aggravating factors |
This phase is about calming the system.
Not strengthening it yet.
Signs your physiotherapist is doing it right
If your physio:
- does a detailed assessment before treatment
- explains what they are checking
- avoids rushing into exercises
- modifies treatment based on your response
That’s a good sign.
On the other hand, if everyone gets the same exercise sheet on day one, that’s not personalized care.
Lifestyle plays a bigger role than you think
Sometimes your headache is not just about your neck.
It can be influenced by:
- poor sleep
- long screen hours
- stress levels
- breathing patterns
If these are not addressed, exercises alone will not solve the problem.
This is why your physiotherapist may focus on habits before exercises.
The mistake many patients make
They go home and start:
- random YouTube exercises
- aggressive stretching
- daily strengthening routines
Too early.
And then they say:
“Exercises made my headache worse.”
The problem is not exercise.
The problem is timing.
Common myths about headache treatment
Myth 1: More exercises = faster recovery
Not always true
Myth 2: Pain means damage
Often it means sensitivity
Myth 3: Stretching always helps
Too much stretching can irritate symptoms
Myth 4: One exercise works for everyone
Treatment must be individualized
What you should do between sessions
Instead of guessing exercises, focus on:
- keeping movements gentle and comfortable
- avoiding positions that clearly trigger pain
- taking regular breaks from screens
- improving sleep routine
Small changes here often reduce headache intensity more than random exercises.
What research says about timing and progression
Modern rehabilitation follows a phased approach.
Phase 1
Reduce pain and sensitivity
Phase 2
Restore movement control
Phase 3
Build strength and endurance
Recent studies show that exercise is effective in reducing headache frequency and intensity, but only when introduced progressively. (Geneen et al. 2017)
So skipping phases often leads to poor outcomes.
When do exercises actually start
Most patients begin exercises when:
- pain is less reactive
- movement feels safer
- the body tolerates load
Then we introduce:
- deep neck flexor activation
- posture correction
- scapular control
Now exercises become effective instead of irritating.
A small but important insight
Your headache may not be just neck-related.
There can be involvement of:
- jaw mechanics
- breathing patterns
- stress response (La Touche et al. 2009)
This study showed that combining physiotherapy with orofacial treatment improved outcomes in cervicogenic headache.
So sometimes your physio is looking beyond the obvious.
Why some clinics give exercises immediately
Let’s be honest.
Some clinics follow templates.
Everyone gets exercises from day one.
It feels productive.
But it is not always effective.
Because headache management requires precision, not speed.
What progress actually looks like
Progress is not always:
- zero pain in one week
- immediate relief after one session
Instead, you may notice:
- headaches becoming less frequent
- triggers becoming more predictable
- recovery after flare-ups becoming faster
These are real signs your treatment is working.
Final thought from a physiotherapist
If your physiotherapist did not start exercises immediately, it does not mean:
- nothing was done
- your condition is simple
- or treatment was delayed
It usually means:
your treatment is being built step by step
And when exercises are finally introduced, they are far more likely to work.
So if you’re still wondering “why didn’t my physio give me exercises?”, it’s usually because they’re focused on finding and fixing the real cause, not just rushing into treatment.
Frequently Asked Questions
Why didn’t my physiotherapist give exercises in the first session?
Because your condition may be in a sensitive phase where exercises can worsen symptoms. Assessment and pain reduction come first.
Are exercises necessary for headache recovery?
Yes, but they should be introduced at the right time. Early or incorrect exercises can increase symptoms.
Can physiotherapy help without exercises initially?
Yes. Manual therapy, education, and lifestyle changes can reduce pain before exercises begin.
When will I start exercises?
Usually within a few sessions once pain reduces and your body tolerates movement better.
Why did my headache worsen after doing exercises?
It may be due to starting too early, incorrect technique, or doing too much too soon.
Is manual therapy enough for long-term relief?
Manual therapy helps early on, but long-term recovery usually includes exercises and lifestyle changes.
Are all headaches treated the same way?
No. Treatment depends on the cause, type, and sensitivity of your headache.
Should I follow exercises from YouTube?
It is better to follow a personalized plan. Generic exercises can sometimes worsen symptoms.
Stay tuned with us for more health related topics.
Follow us on LinkedIn and Instagram for more.
Medical Disclaimer!
This article has been reviewed and written under the guidance of our Head Physiotherapist, Dr. Kruti Raj (PT, MUHS,CPT,CMPT). The information shared is intended for educational purposes only and should not be considered a substitute for personalized medical advice, diagnosis, or treatment.
Please consult us or any other qualified healthcare professional before beginning any exercise program, especially if you are experiencing pain, recovering from injury, or managing a medical condition.











