Introduction To Swollen Lymph Nodes In The Neck
A swelling in the neck changes how people think almost instantly. Some ignore it completely. Others assume the worst.
In practice, most cases are neither extreme.
What matters is not just the swelling, but how it behaves over time and how your body responds around it.
When patients come in, they usually point to the lump. But what I assess goes beyond that.
Because the lymph node is only one part of a much larger system.
Read about our Complete Neck Pain Guide : Causes, Symptoms, Exercises and Treatment
Quick Answer
Swollen lymph nodes in the neck, also called cervical lymphadenopathy, are most commonly caused by infections such as cold, flu, or throat issues. In many cases, they are soft, tender, and reduce within one to two weeks.
However, if the swelling persists beyond three to four weeks, increases in size, or feels hard and fixed, medical evaluation is important. From a physiotherapy perspective, recovery can be supported by improving breathing, posture, and neck mobility to enhance lymphatic flow.
Read about: Early Signs of Cervical Spine Damage You Should Never Ignore
Key Takeaways
- Most swollen lymph nodes in the neck are caused by infections and are not dangerous.
- Soft, tender, and mobile nodes usually indicate a normal immune response.
- Persistent, hard, or growing nodes should always be evaluated medically.
- Lymphatic drainage depends on movement, breathing, and posture.
- Residual neck heaviness after infection is often due to reduced fluid flow, not ongoing disease.
- Physiotherapy supports recovery by improving mobility, muscle balance, and circulation.
- Avoid repeated touching or aggressive massage of the lymph node.
- Recovery is not just about the node, but how the entire system returns to normal.
Also read: How to Relieve Neck Tightness Without Equipment
What Causes a Lymph Node To Swell
Lymph nodes are part of the lymphatic system, which works quietly in the background.
It helps with:
- Immune response
- Fluid balance
- Waste clearance
When something triggers the immune system, lymph nodes react.
They enlarge because:
- Immune cells multiply
- Fluid accumulates
- Filtration activity increases
Recent research shows that cervical lymph nodes are not just local filters.
They are involved in broader fluid clearance pathways, including drainage from the brain and surrounding tissues. (Al-Diwani et al. 2024)
This explains why swelling sometimes feels more “systemic” than local.
Read about : 15 Common Causes of Neck Pain You Should Know
Common Causes
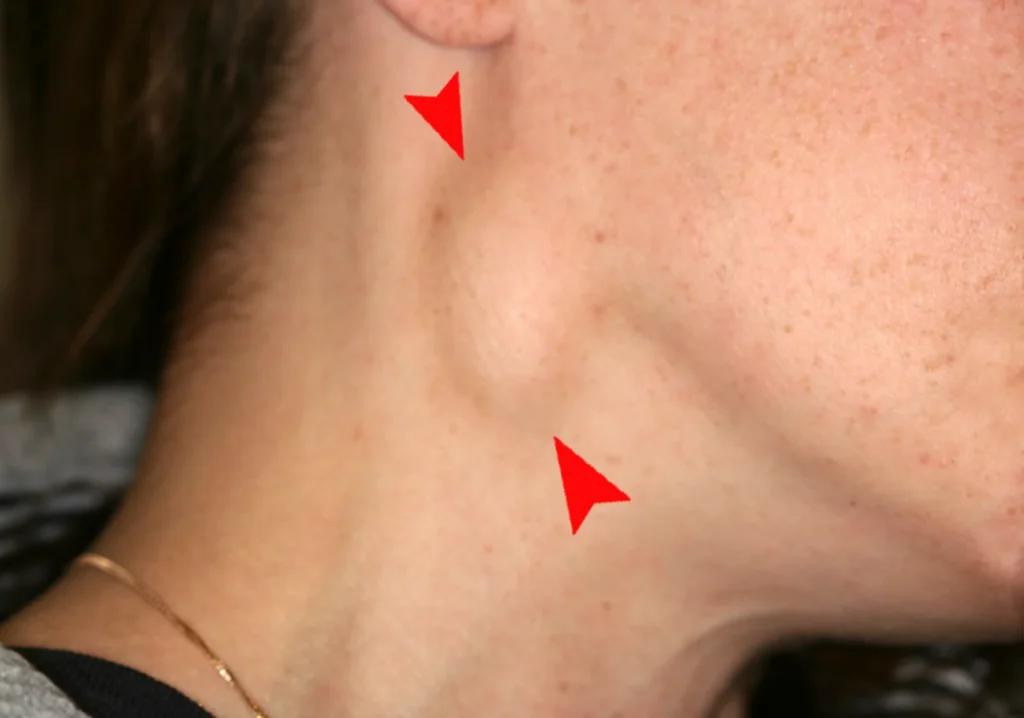
Acute infections
This is the most common scenario.
- Cold
- Flu
- Throat infections
- Dental infections
In these cases:
- Nodes are usually tender
- Swelling appears quickly
- Reduces as infection settles
Persistent or subacute causes
Some cases do not follow the typical pattern.
You may see:
- Tuberculosis
- Autoimmune conditions
- Chronic inflammatory states
These tend to linger and require deeper evaluation. (Liu et al. 2025)
Less discussed but clinically important
There is something many people are not told.
Even after infection is gone, swelling or fullness can remain.
Not because disease is still active, but because:
- Lymphatic drainage is slow
- Tissue mobility is reduced
- Muscles around the area are tight
This is where recovery often gets delayed.
Read: Sore Throat and Stiff Neck: When to Worry
What Makes Lymph Nodes Reassuring or Concerning
Instead of memorizing long lists, think in patterns.
Usually not concerning
- Soft or slightly rubbery
- Tender to touch
- Moves under the skin
- Appears during illness
Needs further evaluation
- Hard
- Fixed in place
- Increasing in size
- Present beyond 3 to 4 weeks
Advances in imaging show that differentiating benign and malignant lymph nodes still requires careful evaluation and cannot rely on size alone. (Liu et al. 2025)
Read : How to Treat Neck Pain in Ankylosing Spondylitis
Why Swelling Does Not Go Away Quickly
This is one of the most common concerns.
Patients often say
“The infection is gone, but I can still feel something”
There are a few reasons for this.
1. Residual immune activity
The node takes time to return to baseline.
2. Structural change
Sometimes the node becomes slightly fibrotic.
3. Slow lymphatic flow
This is the most overlooked factor.
The lymphatic system does not have a central pump like the heart.
It depends on:
- Movement
- Muscle contractions
- Breathing
Recent work on lymphatic physiology shows that lymph flow is influenced by pressure changes and vessel mechanics, not just passive drainage. (Jaszczak-Dyka et al. 2026)
If these mechanisms are not working well, recovery slows down.
Read more: Rheumatoid Arthritis Neck: Causes, Symptoms and Treatments
The Physiotherapy Perspective
This is usually the point where most explanations stop. Diagnosis is made, medication is given if needed, and then patients are told to wait.
But in real life, recovery does not always follow a straight line.
Many people come back after the infection has settled and say something like,
“The swelling is better, but my neck still feels heavy or tight.”
That is where physiotherapy becomes relevant.
Physiotherapy does not aim to “treat” the lymph node itself. We are not trying to shrink it directly. Instead, we look at everything around it that may be slowing down recovery.
Because what often lingers is not active disease, but the after-effect on the surrounding system.
Read about: Neck And Jaw Pain Together? Here’s The Full Clinical Picture
When I assess someone in this phase, I am thinking about a few key things.
Fluid Movement
First is fluid movement. The lymphatic system depends on subtle pressure changes and movement to keep fluid circulating.
If someone has been inactive, unwell, or breathing shallowly for days, that flow tends to slow down.
This can create a feeling of residual fullness even when the primary issue has improved.
Tissue Mobility
Second is tissue mobility. The neck is a compact area with muscles, fascia, vessels, and lymphatic pathways all running close together.
After inflammation, these tissues can become slightly stiff or restricted. Not enough to show on a scan, but enough for the patient to feel “not quite normal.”
Muscle Balance
Then comes muscle balance. Muscles like the sternocleidomastoid and scalenes often become tense, especially if someone has been guarding their neck or feeling unwell.
That tension can subtly affect local circulation and contribute to discomfort or a dragging sensation.
Posture
And finally, posture. This is something people underestimate.
A forward head position or slouched upper back can compress structures in the front of the neck.
Over time, this does not cause the swelling, but it can make recovery slower and symptoms more noticeable.
So when we work in physiotherapy, the goal is not aggressive treatment. It is gentle correction.
We guide the body back toward:
- Better movement
- Easier breathing
- Reduced unnecessary muscle tension
When these improve, fluid movement improves.
When fluid movement improves, that lingering sensation around the lymph node often settles gradually.
It is a subtle process, but in many cases, this is the missing piece between “the infection is gone” and “I feel normal again.”
Read : A Complete Guide To Neck Arthritis
What We Look At In Clinic
When someone comes in with persistent neck swelling or discomfort, I assess:
- Neck movement
- Muscle tightness
- Rib cage expansion
- Breathing pattern
- Postural alignment
Because all of these affect lymphatic return.
Read: Lhermitte’s sign- An Electic Shock Sensation Down The Neck
Breathing Is More Important Than People Think
Most people breathe shallowly, especially after illness.
But lymphatic flow depends on pressure changes inside the chest.
Deep breathing improves:
- Fluid movement
- Circulation
- Recovery speed
Research into cervical lymphatic pathways shows their role in fluid clearance and systemic regulation. Wang et al. (2025)
Read about: Yoga for Neck Pain: Poses That Actually Work
Movement Helps More Than Rest
After infection, people tend to reduce activity too much.
But the lymphatic system depends on movement.
Even gentle activity:
- Improves circulation
- Prevents stagnation
- Supports recovery
Complete inactivity slows things down.
Also Read: Ultimate 6 Weeks Neck Rehabilitation Exercises For Pain Relief
Rehabilitation That Actually Works
Breathing re-education
- Slow controlled breathing
- Rib cage expansion
- Avoid shallow chest breathing
Read: 10 Proven Home Remedies for Neck Pain from Anxiety
Gentle neck mobility
- Rotation
- Side bending
- Small, controlled movements
Not aggressive stretching.
Postural correction
Instead of forcing straight posture, focus on:
- Reducing forward head position
- Opening the chest
This reduces compression in the neck.
Read: Simple Posture Correction Exercises for Forward Head Posture
Soft tissue relaxation
Targeting:
- Sternocleidomastoid
- Upper trapezius
- Scalene muscles
Gradual return to activity
Avoid both extremes:
- Complete rest
- Sudden overactivity
Read: 10 Proven Home Remedies for Neck Pain from Anxiety
Lesser Known Clinical Observations
These are things patients usually find surprising.
- Lymph nodes can remain slightly enlarged even after recovery
- Hydration affects lymph flow
- Poor sleep slows immune recovery
- Repeatedly touching the node can irritate it
- Tight clothing around the neck can worsen discomfort
Read: How To Use Cervical Collar for Neck Support: Benefits & Hidden Risks
When Physiotherapy Should Not Be The First Step
If you notice:
- Persistent swelling without clear cause
- Hard or fixed node
- Weight loss or prolonged fever
You should first seek medical evaluation.
Physiotherapy comes after diagnosis, not before it.
Learn About: The Ultimate Neck Stretch Routine for Desk Workers in 2026
Final Thoughts
Most swollen lymph nodes in the neck are not dangerous.
But they are meaningful.
They reflect how your immune system is responding and how efficiently your body is recovering.
If you only focus on the lump, you miss the process behind it.
If you understand the system, recovery becomes clearer.
Read about: Effective Neck Pain Exercises At Home: A Complete Guide to Relief and Improved Mobility
Frequently Asked Question
Q1. How long do swollen lymph nodes in the neck last?
Most reduce within one to two weeks, but some may take longer depending on recovery and overall health.
Q2. Can lymph nodes stay enlarged after infection?
Yes, mild enlargement can persist even after recovery and is usually not harmful.
Q3. When should I worry about a neck lump?
If it lasts more than three to four weeks, grows in size, or feels hard and fixed, it should be evaluated.
Q4. Can posture affect lymph node recovery?
Yes, poor posture can slow lymphatic drainage and make symptoms last longer.
Q5. Does physiotherapy help swollen lymph nodes?
It does not directly shrink the node but helps improve fluid movement and recovery.
Q6. Is it safe to keep touching the lymph node?
No, repeated touching can irritate the area and delay healing.
Q7. Can neck stiffness be related to lymph node swelling?
Yes, surrounding muscle tightness can cause stiffness and discomfort.
Stay tuned with us for more health related topics.
Follow us on LinkedIn and Instagram for more.
Medical Disclaimer!
This article has been reviewed and written under the guidance of our Head Physiotherapist, Dr. Kruti Raj (PT, MUHS,CPT,CMPT). The information shared is intended for educational purposes only and should not be considered a substitute for personalized medical advice, diagnosis, or treatment.
Please consult us or any other qualified healthcare professional before beginning any exercise program, especially if you are experiencing pain, recovering from injury, or managing a medical condition.











