Neck pain that radiates into the shoulder or arm can feel frightening. Many patients worry that something serious has happened to their spine or that they may require surgery. One common reason behind such symptoms is a herniated cervical disc, often referred to as a slipped disc in the neck.
In physiotherapy practice, cervical disc herniation is one of the most frequently encountered spinal conditions.
Fortunately, most cases respond very well to non-surgical treatment, targeted rehabilitation, and posture correction.
Modern research shows that structured physiotherapy programs can significantly reduce pain, improve function, and help patients return to their daily activities without invasive treatment.
Read our detailed and Complete Guide to Neck Pain: Causes, Symptoms, Exercises and Treatment
Understanding the Cervical Spine
The cervical spine forms the upper part of the spinal column and consists of seven vertebrae (C1–C7) located in the neck.
Between each vertebra lies an intervertebral disc, which acts as a cushion and shock absorber.
Each disc has two main components:
Nucleus pulposus
A soft gel-like core that absorbs shock and distributes load.
Annulus fibrosus
A strong fibrous outer ring that keeps the disc intact.
These discs allow the neck to move freely while also protecting the spinal cord and nerves.
However, over time the disc can weaken or degenerate. When the inner gel pushes through the outer layer, it results in disc herniation.
When this occurs in the neck, it is known as a herniated cervical disc.
What Is a Herniated Cervical Disc?
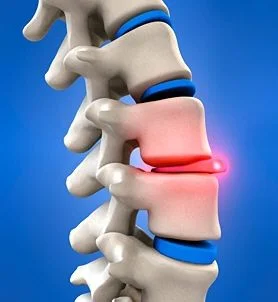
A herniated cervical disc occurs when the soft center of the disc protrudes through the outer layer and compresses nearby nerves or the spinal cord.
This compression can cause symptoms such as:
Neck pain
Arm pain
Numbness or tingling
Weakness in the arm or hand
Disc herniation is one of the major causes of cervical radiculopathy, a condition where nerve roots in the neck become irritated or compressed.
Studies estimate that disc herniation accounts for around 20–25% of cervical radiculopathy cases.
How Common Is Cervical Disc Herniation?
Disc problems are extremely common in adults.
Studies indicate:
- about 2 percent of people develop a disc herniation each year (JCDR)
- the condition is most common between ages 30 and 50
- individuals with sedentary desk jobs have a higher risk
Modern lifestyle habits such as prolonged smartphone use, poor workstation ergonomics, and long hours of computer work have increased the prevalence of cervical spine disorders.
Physiotherapists increasingly see younger patients presenting with disc-related neck pain due to these factors.
Read about : 15 Common Causes of Neck Pain You Should Know
Causes of Cervical Disc Herniation

Disc herniation usually develops due to a combination of mechanical stress and degenerative changes.
Age-Related Disc Degeneration
As we age, spinal discs gradually lose water content and elasticity. This natural process makes them more prone to cracks and tears.
Even small movements can eventually trigger herniation in a weakened disc.
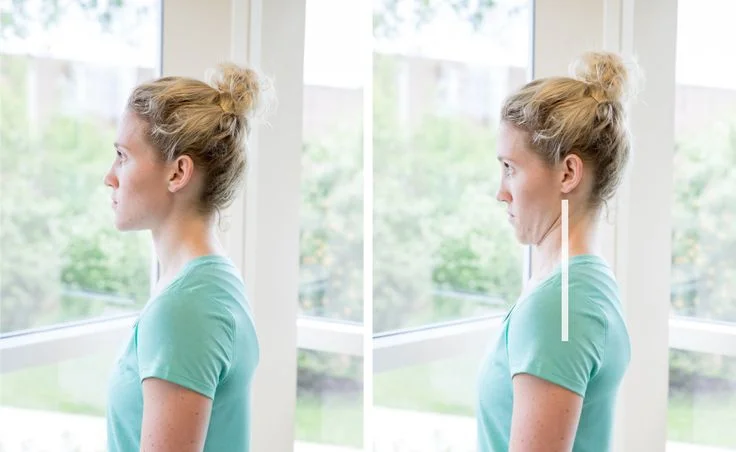
Poor Posture
Poor posture is one of the most underestimated causes of cervical disc problems.
Forward head posture dramatically increases stress on cervical discs. Biomechanical studies show that when the head tilts forward just 15 degrees, the load on the neck can increase several times.
This excessive stress accelerates disc degeneration.
Prolonged Sitting
Long hours of sitting, especially in front of computers, create constant pressure on the cervical spine.
Static positions reduce blood circulation to spinal structures and increase disc pressure.
Trauma or Sudden Injury
Injuries such as:
- whiplash accidents
- sports trauma
- falls
can cause the disc to rupture suddenly.
Repetitive Neck Movements
Occupations involving repetitive neck motion increase risk. Examples include dentists, surgeons, tailors, drivers, and computer professionals.
Genetic Factors
Some individuals inherit weaker disc structures, making them more vulnerable to early degeneration.
Lesser Known Risk Factors
Several factors that patients rarely consider may contribute to cervical disc herniation.
Smoking
Smoking reduces blood supply to spinal discs, which accelerates degeneration.
Chronic Stress
Stress causes prolonged muscle tension in the neck and shoulders, increasing pressure on cervical structures.
Weak Deep Neck Muscles
Weak deep cervical stabilizers reduce spinal support and increase disc loading.
Symptoms of Herniated Cervical Disc
Symptoms depend on the level of disc herniation and the nerve affected.
Neck Pain
Neck pain is often the first symptom.
The pain may be:
- dull
- sharp
- burning
- localized to one side of the neck
Pain usually worsens with movement.
Radiating Arm Pain
When a nerve root becomes compressed, pain may radiate into the:
- shoulder
- upper arm
- forearm
- fingers
This pattern of nerve pain is known as cervical radiculopathy.
Read in detail about: Cervical Radiculopathy: Why Neck Nerve Pain Travels to the Arm
Numbness and Tingling
Patients frequently experience:
- pins and needles
- burning sensation
- numbness in specific fingers
These symptoms follow the pathway of the affected nerve.
Read in detail about: Cervical Disc Degeneration: The Hidden Cause of your Neck Pain
Muscle Weakness
In severe cases, nerve compression can lead to weakness in muscles controlling the arm or hand.
Examples include:
- reduced grip strength
- difficulty lifting objects
- weakness while pushing or pulling
Reduced Neck Mobility
Many patients notice stiffness or difficulty turning their head.
Most Common Levels of Cervical Disc Herniation
Certain cervical levels are more commonly affected.
C5–C6 Disc Herniation
This is the most frequently affected level.
Symptoms may include:
- pain in shoulder and arm
- biceps weakness
- numbness in the thumb
C6–C7 Disc Herniation
The second most common level.
Typical symptoms include:
- arm pain extending to the forearm
- triceps weakness
- numbness in the middle finger
How Is Cervical Disc Herniation Diagnosed?
Diagnosis involves clinical examination and imaging tests.
Clinical Examination
A physiotherapist evaluates:
- neck movement
- muscle strength
- reflexes
- nerve sensation
Special tests such as Spurling’s test may reproduce nerve symptoms.
MRI Scan
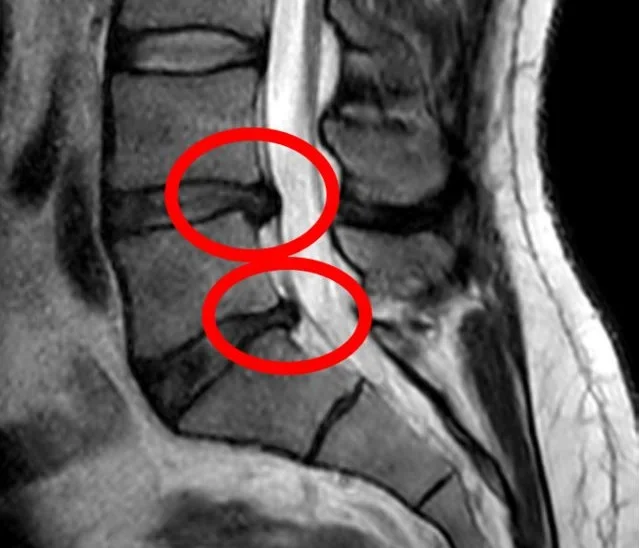
MRI is considered the most accurate imaging technique for diagnosing cervical disc herniation.
It clearly shows:
- disc bulging or protrusion
- nerve root compression
- spinal cord involvement
Recent research is also exploring AI-assisted MRI analysis, which can automatically measure spinal structures and improve diagnostic accuracy. (arxiv)
Read about : What is Cervical Facet Joint Pain, how it causes cervicogenic headaches and how to correct it naturally
Can Herniated Cervical Discs Heal Naturally?
One of the most interesting scientific discoveries is that disc herniations can shrink naturally over time.
The body can break down and reabsorb herniated disc material through inflammatory and immune mechanisms.
This explains why many patients experience gradual improvement without surgery.
Read about: Effective Neck Pain Exercises At Home: A Complete Guide to Relief and Improved Mobility
Conservative Treatment: First Line of Management
Most cervical disc herniations are treated without surgery.
Research consistently shows that conservative management including physiotherapy significantly improves pain and function. (JCDR)
Treatment usually focuses on:
- reducing nerve compression
- restoring neck mobility
- strengthening supportive muscles
- correcting posture
Role of Physiotherapy in Cervical Disc Herniation

Physiotherapy plays a central role in recovery.
A structured rehabilitation program includes:
- pain relief techniques
- therapeutic exercise
- neural mobilization
- posture correction
- ergonomic education
Evidence-Based Physiotherapy Treatments
Cervical Traction
Cervical traction gently stretches the neck and increases the space between vertebrae.
Clinical studies show traction can help:
- reduce nerve compression
- decrease disc pressure
- improve nerve circulation
Many patients experience noticeable symptom relief after traction therapy. (Sciencedirect)
Therapeutic Exercise
Exercise therapy is one of the most effective treatments.
Research shows that targeted cervical exercises improve spinal stability and reduce pain. (Springer)
Important exercises include:
- deep cervical flexor activation
- scapular stabilization exercises
- gentle mobility exercises
These exercises restore balance between neck muscles and reduce stress on discs.
Neural Mobilization
Nerve compression can restrict normal nerve movement.
Neural mobilization techniques help restore nerve gliding and reduce symptoms such as tingling and numbness.
Studies demonstrate significant reductions in pain and disability following neural mobilization therapy.
Soft Tissue and Manual Therapy
Modern physiotherapy often includes:
- myofascial release
- trigger point therapy
- joint mobilization
Recent clinical trials show that instrument-assisted soft tissue mobilization combined with conventional physiotherapy significantly improves pain and functional outcomes.
Electrotherapy
Physiotherapists may use modalities such as:
- TENS therapy
- ultrasound therapy
- infrared therapy
These techniques help reduce pain and muscle spasm.
Stages of Rehabilitation
Recovery usually progresses through stages.
Acute Phase (First 2 Weeks)
Goals include:
- pain reduction
- inflammation control
- gentle mobility exercises
Subacute Phase (2–6 Weeks)
Treatment focuses on:
- posture correction
- strengthening exercises
- nerve mobility
Read more: Simple Posture Correction Exercises for Forward Head Posture
Rehabilitation Phase (6–12 Weeks)
Goals include:
- restoring full function
- improving endurance
- preventing recurrence
Home Exercises for Cervical Disc Herniation
Patients are often advised simple exercises.
Chin Tucks
Strengthens deep neck muscles and improves posture.
Learn How to do Chin Tucks for Neck Pain Relief and Posture Correction
Scapular Retraction

Strengthens shoulder blade muscles and reduces neck strain.
Neck Mobility Exercises

Gentle side bending and rotation exercises help maintain flexibility.
Exercises should always be performed under professional guidance.
Lifestyle Changes That Support Recovery
Daily habits greatly influence recovery.
Patients should:
- avoid prolonged phone use
- maintain ergonomic workstation setup
- take frequent movement breaks
- sleep with proper neck support
Small adjustments can significantly reduce spinal stress.
Learn About: The Ultimate Neck Stretch Routine for Desk Workers in 2026
When Is Surgery Necessary?
Although most patients recover with physiotherapy, surgery may be recommended if:
- severe nerve compression occurs
- progressive weakness develops
- symptoms do not improve after several months
Common surgical procedures include:
- cervical discectomy
- artificial disc replacement
- spinal fusion
Modern surgical techniques aim to preserve motion and reduce complications. (arxiv)
Prevention Strategies
Preventing cervical disc problems requires consistent care of the spine.
Key strategies include:
- maintaining good posture
- strengthening neck muscles
- adjusting computer screens to eye level
- limiting smartphone use
Regular exercise and ergonomic awareness are essential.
Clinical Experience
In physiotherapy practice, one pattern appears repeatedly. Many patients with cervical disc herniation spend long hours using laptops or smartphones with their head tilted forward.
This posture places enormous stress on the cervical discs and surrounding muscles.
However, once patients learn to correct posture and strengthen their deep neck muscles, many experience dramatic improvements in pain and function.
Early physiotherapy intervention often prevents the need for more invasive treatments.
Physio Prescription
For patients with cervical disc herniation:
- practice chin tuck exercises daily
- strengthen deep neck stabilizers
- perform scapular stabilization exercises
- take breaks every 30 minutes during desk work
- maintain proper pillow support during sleep
Consistency with these habits is essential for recovery.
Also read: How to Relieve Neck Tightness Without Equipment
Red Flags
Immediate medical attention is required if patients experience:
- progressive arm weakness
- loss of hand coordination
- difficulty walking
- bladder or bowel problems
These symptoms may indicate spinal cord compression.
Common Myth
Myth
A slipped disc always requires surgery.
Truth
Most cervical disc herniations improve with conservative treatment including physiotherapy, exercise, and posture correction.
Frequently Asked Questions (FAQs)
1. Can a herniated cervical disc heal without surgery?
Yes. In many cases, a herniated cervical disc improves with conservative treatment such as physiotherapy, posture correction, and targeted exercises. Most patients recover within a few weeks to a few months without surgery.
2. What are the most common symptoms of a cervical disc herniation?
Typical symptoms include neck pain, pain radiating to the shoulder or arm, numbness or tingling in the fingers, and sometimes weakness in the arm or hand.
3. How long does it take to recover from a herniated cervical disc?
Recovery time varies depending on the severity of the condition. Mild cases may improve within 4 to 6 weeks, while more severe cases may take 3 to 6 months with proper rehabilitation.
4. Is physiotherapy effective for cervical disc herniation?
Yes. Physiotherapy is one of the most effective treatments. Techniques such as cervical traction, therapeutic exercises, neural mobilization, and posture correction help reduce nerve pressure and improve function.
5. What activities should be avoided with a cervical disc herniation?
Patients should avoid prolonged phone use, poor sitting posture, heavy lifting, and sudden neck movements during the early stages of recovery.
6. Can exercise worsen a herniated cervical disc?
Incorrect or aggressive exercises may worsen symptoms. Therefore, exercises should be performed under the guidance of a physiotherapist and progressed gradually.
7. When should surgery be considered for a cervical disc herniation?
Surgery may be recommended if there is severe nerve compression, progressive muscle weakness, or if symptoms do not improve after several months of conservative treatment.
Final Word
A herniated cervical disc can be painful and disruptive, but it is rarely a permanent or life-threatening condition.
With proper physiotherapy, patient education, and lifestyle changes, most individuals recover successfully and return to normal life.
The most powerful treatment tools remain simple but effective:
movement, posture awareness, and targeted strengthening.
When patients actively participate in rehabilitation, recovery becomes not only possible but highly likely.
Stay tuned with us for more health related topics.
Follow us on LinkedIn and Instagram for more.
Medical Disclaimer!
This article has been reviewed and written under the guidance of our Head Physiotherapist, Dr. Kruti Raj (PT, MUHS,CPT,CMPT). The information shared is intended for educational purposes only and should not be considered a substitute for personalized medical advice, diagnosis, or treatment.
Please consult us or any other qualified healthcare professional before beginning any exercise program, especially if you are experiencing pain, recovering from injury, or managing a medical condition.











