Frozen shoulder vs pinched nerve can be confusing because both conditions often start with similar shoulder pain and stiffness.
If you walk into my clinic with shoulder pain, I am not immediately thinking “frozen shoulder” or “nerve issue.”
I am watching how you move.
How you remove your shirt.
How you reach behind your back.
How you react when pain suddenly shoots.
Because here is the truth.
Most people confuse frozen shoulder and nerve pain, and unfortunately, many are treated for the wrong condition for months.
That delay is what makes recovery harder.
Let’s break this down the way I explain it to my patients.
Quick Answer
Frozen shoulder causes deep stiffness and restricts movement in all directions because the joint capsule becomes tight. Nerve pain, on the other hand, feels sharp, burning, or tingling and often travels down the arm due to nerve irritation. If your shoulder feels stuck, think frozen shoulder. If the pain moves or tingles, think nerve involvement.
Key Takeaways
- Frozen shoulder restricts both active and passive movement
- Nerve pain usually includes tingling, burning, or radiating symptoms
- Neck involvement is a strong indicator of nerve-related pain
- Diabetes significantly increases frozen shoulder risk
- Wrong diagnosis often delays recovery more than the condition itself
- Gentle mobility helps frozen shoulder, not aggressive stretching
- Nerve pain improves with posture correction and nerve gliding
The First Clue: Your Movement Tells Me More Than Your Pain
One of the quickest ways I differentiate these two is not by asking questions.
It is by observing movement.
A frozen shoulder patient moves slowly, almost protectively.
The arm feels stuck.
Even simple movements like combing hair look restricted.
A nerve pain patient is different.
They start moving normally, then suddenly stop.
Almost like they hit an electric shock.
That sudden hesitation is a big giveaway.
What Frozen Shoulder Actually Feels Like- Beyond Google Definitions
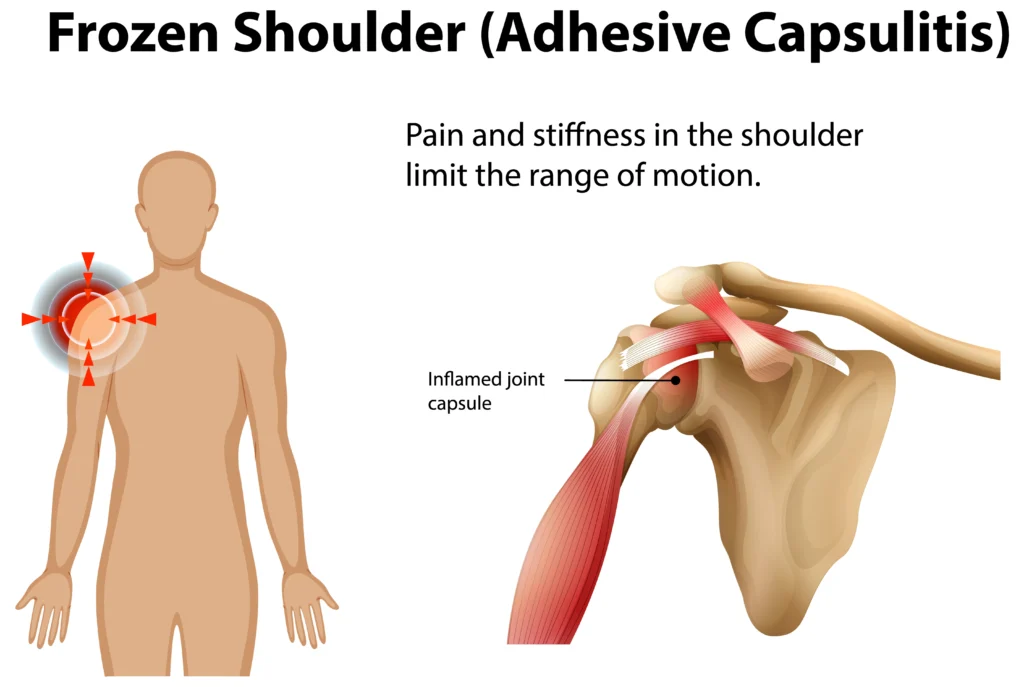
Most articles will tell you it is stiffness.
That is true, but incomplete.
Patients usually say:
- “My shoulder feels jammed”
- “I cannot reach behind my back”
- “It hurts more at night”
- “It came without any major injury”
The most frustrating part is not the pain.
It is the loss of control.
Even if I try to move your arm for you, it does not go fully.
That is a key clinical sign.
Inside the joint, the capsule becomes thick and tight.
It literally restricts motion.
This is why even passive movement is limited.
Research supports that frozen shoulder is driven by inflammation and fibrosis of the joint capsule (Kelley et al., 2013)
Now Compare That With Nerve Pain
Nerve pain behaves very differently.
Patients describe it like:
- burning
- shooting
- tingling
- electric sensation going down the arm
Sometimes they come in saying, “My shoulder hurts,” but when I test the neck, the pain increases.
That is the moment things become clear.
Most of these cases are linked to cervical nerve irritation.
In fact, classic research on cervical radiculopathy shows how pain radiates along specific nerve pathways rather than staying in one joint (Radhakrishnan et al., 1994)
The Shirt Test I Use in Clinic
This is something patients never expect.
I ask them to wear or remove a shirt.
Frozen shoulder patients struggle slowly.
The movement is restricted throughout.
Nerve pain patients start normally.
Then midway, they stop due to a sharp pain shooting down the arm.
That difference is subtle but extremely reliable.
The Sleeping Pattern Clue
Another underrated detail.
Frozen shoulder patients often complain of:
- deep aching pain at night
- inability to sleep on the affected side
Nerve pain patients:
- feel relief in certain neck positions
- may wake up with tingling or numbness
That positional variation is important.
A Lesser Known Overlap That Confuses Even Doctors
Here is something not many articles mention.
You can have both.
Recent studies suggest that shoulder stiffness and nerve sensitivity can coexist, especially in chronic cases where movement has been restricted for long (Exploration of Musculoskeletal Diseases, 2025)
So if someone says, “I have both stiffness and tingling,” do not dismiss it.
It happens more often than we think.
Why Diabetes Changes the Whole Picture
If a patient has diabetes, my suspicion for frozen shoulder immediately increases.
Not slightly. Significantly.
Studies show a strong association between diabetes and adhesive capsulitis (Zreik et al., 2016)
Also, recovery tends to be slower.
This is something many patients are never told early on.
The Biggest Mistake I See in Treatment
People treat both conditions the same way.
That is where things go wrong.
Frozen shoulder needs:
- gentle, progressive mobility work
- patience
- gradual loading
Nerve pain needs:
- neck assessment
- posture correction
- nerve gliding exercises
If you aggressively stretch a nerve condition, symptoms worsen.
If you ignore stiffness in frozen shoulder, mobility never returns.
Different problem. Different solution.
Physiotherapy Exercises I Actually Prescribe
Before jumping into exercises, one thing matters more than the exercise itself.
Doing the wrong type of exercise can make things worse.
So I always divide this into two paths.
If It Is Frozen Shoulder
Focus on Mobility, Not Force.
These exercises should feel like a stretch, not a struggle.
1. Pendulum Exercise
Lean forward slightly and let your arm hang loose.
Gently swing it in small circles.
- Do not control the movement too much
- Let gravity do the work
- 1 to 2 minutes, twice daily
This is often the safest starting point when movement is very limited.
2. Wall Climbing (Finger Walk)
Stand facing a wall and slowly “walk” your fingers upward.
- Stop before sharp pain
- Hold for 5 to 10 seconds
- Repeat 8 to 10 times
This helps restore movement without forcing the joint.
3. Towel Stretch (Behind the Back)
Hold a towel behind your back with both hands.
- Use the good arm to gently pull the affected arm upward
- You should feel a stretch, not pain
- Hold for 10 seconds
This specifically targets internal rotation, which is often the most restricted.
If It Is Nerve Pain
Focus on Nerve Mobility and Neck Control
Here, stretching the shoulder aggressively is a mistake.
We focus on nerve movement and posture.
1. Nerve Gliding Exercise
Extend your arm sideways, gently bend your wrist back, and tilt your neck away.
- Move slowly in and out of the position
- Do not hold if it increases symptoms
- 10 repetitions
This helps reduce nerve sensitivity over time.
2. Chin Tucks
Sit or stand straight and gently pull your chin backward.
- Do not tilt your head down
- Hold for 5 seconds
- Repeat 10 times
This improves cervical alignment and reduces nerve compression.
3. Scapular Retraction
Pull your shoulder blades slightly back and down.
- Avoid shrugging
- Hold for 5 seconds
- Repeat 10 to 15 times
This builds stability and reduces strain on the neck and shoulder.
A Small but Important Tip I Tell Every Patient
If an exercise causes:
- sharp pain
- tingling increase
- pain spreading down the arm
Stop and reassess.
Pain is feedback, not something to push through blindly.
Why These Exercises Work
Modern physiotherapy is moving away from aggressive stretching toward controlled, progressive movement.
Recent studies show that combining mobility, neural techniques, and posture correction gives better outcomes than isolated approaches (Kelley et al., 2013)
Neurodynamic exercises have also been shown to improve symptoms in nerve-related conditions when applied correctly (Kuijper et al., 2009)
Why Scans Sometimes Mislead Patients
This part surprises many people.
An MRI may show:
- mild disc bulge
- minor shoulder changes
But those findings do not always match your symptoms.
Clinical assessment is often more reliable than imaging alone.
This is why some people keep switching treatments without results.
Recovery Is Not Always Predictable
Earlier, frozen shoulder was believed to resolve in 1 to 2 years.
Now we know it is not that simple.
Some recover faster. Some take longer.
Recent clinical reviews suggest variability based on:
- metabolic health
- activity levels
- early intervention (NCBI StatPearls, updated clinical review)
What I Tell My Patients Honestly
If your arm feels stuck in all directions, think frozen shoulder.
If your pain travels, tingles, or shoots, think nerve involvement.
If you are unsure, do not guess.
Because guessing delays recovery more than the condition itself.
How to Know If You’re on the Right Track
This is something patients rarely ask early, but it makes a huge difference.
Because not all progress feels like improvement.
Sometimes healing feels slow. Sometimes it feels confusing.
So here is how I help my patients judge it correctly.
Signs You’re Improving, Even If It Feels Slow:
- You can move slightly more than last week
- Pain intensity is the same, but movement is easier
- Daily tasks feel less restricted
- Night pain is becoming less frequent
That is real progress.
It may not feel dramatic, but it is exactly how recovery should look.
Signs You Might Be Doing Too Much
- Pain spikes after exercise and stays for hours
- Stiffness increases the next day
- Tingling or burning symptoms increase
- You feel worse after “pushing through” exercises
This is common, especially in motivated patients.
More effort does not always mean better results.
A Pattern I See Very Often
People with frozen shoulder tend to: push too hard too early
People with nerve pain tend to: ignore posture and focus only on the shoulder
Both slow down recovery.
The 24-Hour Rule I Use in Clinic
After doing any exercise, ask yourself:
“Do I feel the same or better after 24 hours?”
- If yes → you’re on the right track
- If worse → you need to scale back
This simple rule prevents most setbacks.
Why This Section Matters
Recovery is not just about what exercises you do.
It is about how your body responds to them.
That awareness is what separates fast recovery from long frustration.
Final Thoughts On Frozen Shoulder Vs Pinched Nerve
If there is one thing I want you to take away from this article, it is this:
Shoulder pain is not just about where it hurts. It is about how it behaves.
In clinic, I rarely rush to label something as frozen shoulder or nerve pain on day one.
I observe patterns. I look at movement.
I listen to how the pain responds to simple tests.
Because the name of the condition matters less than understanding the pattern behind it.
Frozen shoulder tends to lock the joint and limit every direction.
Nerve pain tends to travel, change, and react to neck position.
That difference guides everything.
What I have also learned over the years is this:
- People recover faster when they stop guessing
- They do better when treatment matches the actual problem
- And most importantly, they improve when they stay consistent, not aggressive
You do not need complicated routines. You need the right approach for your condition.
If your shoulder feels stuck, work on gentle mobility and give it time.
If your pain travels or tingles, do not ignore your neck.
And if you are still unsure, that is your sign to get assessed properly rather than experimenting blindly.
Recovery is rarely about doing more.
It is about doing what actually fits your problem.
Understanding frozen shoulder vs pinched nerve early can prevent the wrong treatment and help recovery start sooner.
Frequently Asked Questions
1. How do I know if my shoulder pain is nerve-related or frozen shoulder?
If your pain includes tingling, burning, or travels down your arm, it is likely nerve-related. If your shoulder feels stiff and restricted in all movements, it is more likely frozen shoulder.
2. Can frozen shoulder cause tingling or numbness?
Frozen shoulder typically does not cause tingling. If you feel numbness or pins and needles, nerve involvement should be considered.
3. Is neck pain always present in nerve-related shoulder pain?
Not always, but many cases of nerve pain originate from the neck even if neck pain is mild or unnoticed.
4. Should I exercise if my shoulder is painful?
Yes, but only the right type of exercise. Frozen shoulder needs gentle mobility, while nerve pain needs nerve-friendly movements and posture correction.
5. How long does it take to recover from frozen shoulder?
Recovery varies widely. Some people improve in months, while others may take over a year depending on treatment and consistency.
6. Can both frozen shoulder and nerve pain happen together?
Yes, especially in long-standing cases where stiffness and nerve sensitivity overlap.
7. When should I see a physiotherapist?
If your pain lasts more than two weeks, limits movement, or includes tingling or weakness, a proper assessment is recommended.
Stay tuned with us for more health related topics.
Follow us on LinkedIn and Instagram for more.
Medical Disclaimer!
This article has been reviewed and written under the guidance of our Head Physiotherapist, Dr. Kruti Raj (PT, MUHS,CPT,CMPT). The information shared is intended for educational purposes only and should not be considered a substitute for personalized medical advice, diagnosis, or treatment.
Please consult us or any other qualified healthcare professional before beginning any exercise program, especially if you are experiencing pain, recovering from injury, or managing a medical condition.











