Scrofula, or tuberculous cervical lymphadenitis, may sound like an old-world disease, but it continues to appear regularly in clinical practice, especially in countries with a high tuberculosis burden like India.
It is considered one of the most common forms of extrapulmonary tuberculosis, accounting for a significant proportion of TB cases outside the lungs (Vinod S et al., 2023)
From a physiotherapy perspective, what makes scrofula particularly important is not just the infection itself, but the functional limitations that persist even after medical treatment is completed.
Read about our Complete Neck Pain Guide : Causes, Symptoms, Exercises and Treatment
Quick Answer
Scrofula is a form of tuberculosis that affects the lymph nodes in the neck, causing painless swelling that may progress to abscess or scarring if untreated. While medical treatment eliminates the infection, physiotherapy plays a key role in restoring neck mobility, reducing stiffness, and preventing long-term functional limitations.
Read about: Early Signs of Cervical Spine Damage You Should Never Ignore
Key Takeaways
- Scrofula is a tuberculosis-related infection affecting neck lymph nodes.
- It usually presents as a painless swelling that progresses slowly.
- Medical treatment is essential but may not restore full function.
- Fibrosis and scar tissue can lead to long-term stiffness.
- Physiotherapy helps restore movement, posture, and tissue mobility.
- Early rehabilitation prevents chronic neck dysfunction.
- Posture and daily habits play a major role in recovery.
Read about : 15 Common Causes of Neck Pain You Should Know
What Exactly is Scrofula
Scrofula is a chronic infection of the cervical lymph nodes, most commonly caused by Mycobacterium tuberculosis.
It typically presents as a slow-growing, painless swelling in the neck, which often delays medical attention.
Interestingly, clinical literature shows that scrofula can mimic serious conditions like lymphoma or metastatic cancer, which makes early diagnosis challenging in real-world scenarios (D’Amato G et al., 2026)
From a pathological standpoint, the disease progresses through a sequence that is very relevant for rehabilitation:
Disease Progression
- Granuloma formation
- Caseation necrosis
- Liquefaction
- Abscess formation
- Sinus tract development
- Fibrosis and scarring
The final stage, fibrosis, is where most long-term physical issues arise and where physiotherapy becomes essential.
Read: Understanding Swollen Lymph Nodes In The Neck
Simple Self-Check

Many patients I see mention that they ignored the swelling for months because it was not painful. A quick self-check approach can help catch issues earlier.
You should consider getting a neck swelling evaluated if:
- The lump has been present for more than 2 to 3 weeks
- It is slowly increasing in size
- It feels firm or rubbery rather than soft
- It does not reduce with rest or basic medication
- There is a history of tuberculosis exposure in the family
- You feel mild stiffness or tightness in the neck over time
A useful practical tip is this:
If a swelling does not behave like a simple infection and does not resolve within a few weeks, it deserves proper medical attention.
Early diagnosis often means less tissue damage and a smoother recovery later.
Read: Branchial Cleft Cyst: A Complete Guide To Neck Lump
How Patients Actually Present in Clinics
In practice, patients rarely present early. Most describe something like this:
- A lump in the neck that has been present for weeks or months
- Initially painless
- Gradually increasing in size
Clinical observations show that lymph nodes often become matted together, meaning they stick to each other and surrounding tissues, which is a key feature of tuberculous lymphadenitis (Alam MJ et al., 2023)
As the condition progresses:
- The swelling may soften due to internal necrosis
- Skin over the node may discolor
- Abscess formation may occur
- In advanced cases, rupture leads to discharge
A recent clinical case described a painless neck mass that progressed to ulceration and sinus formation over time, highlighting how quietly the disease can evolve (Bocchi P et al., 2024)
Also Read: Neck Pain with Fever: When To Worry And How To Treat
Red Flags
In clinical practice, not every neck swelling behaves the same way. While scrofula usually progresses slowly, there are certain signs that should never be ignored.
If you notice any of the following, it is important to seek medical evaluation without delay:
- Rapid increase in the size of the swelling over days rather than weeks
- Severe pain or tenderness, which is not typical in early scrofula
- Difficulty swallowing or breathing
- Persistent fever, night sweats, or unexplained weight loss
- Multiple enlarged lymph nodes in different parts of the body
- Hard, fixed nodes that do not move at all
These symptoms may indicate complications, drug-resistant infection, or even other serious conditions that mimic scrofula.
From a physiotherapy perspective, recognizing these red flags is important because rehabilitation should never begin until proper medical evaluation and stabilization are completed.
Read: How to Fix Sagging,Ozempic Neck After Rapid Weight Loss
A Lesser Known Variant: Scrofuloderma
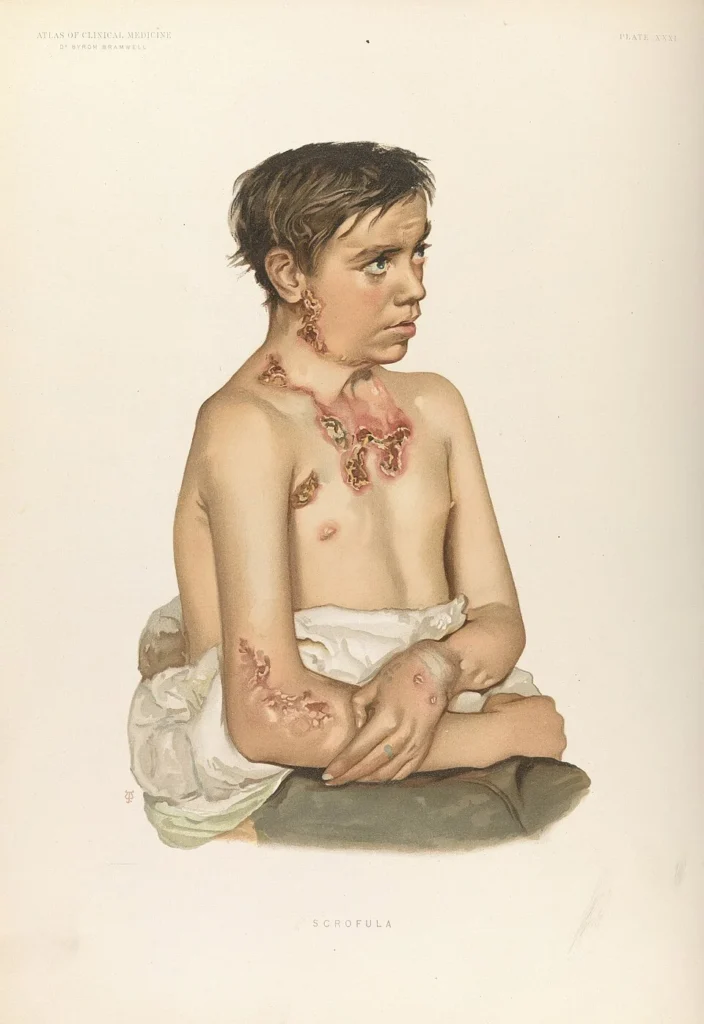
One important but often overlooked condition is scrofuloderma, where the infection spreads from lymph nodes to the overlying skin.
This leads to:
- Chronic ulcers
- Draining sinus tracts
- Significant scarring
Recent case reports show that scrofuloderma is frequently diagnosed late, especially in resource-limited settings (Yadav S, 2023)
From a rehabilitation perspective, this increases the risk of:
- Skin contractures
- Deep adhesions
- Severe restriction in cervical movement
Read: A Complete Guide To Sinuses Related Neck Pain
Why Diagnosis is Often Delayed
Scrofula is often missed or delayed because:
- It is painless in early stages
- Symptoms are non-specific
- Chest X-rays may be normal
- Blood investigations are not always conclusive
Diagnosis usually relies on:
- Fine needle aspiration cytology
- Biopsy
- Molecular tests such as GeneXpert
Even in modern settings, diagnosis may take weeks, which allows the disease to progress further (Neves S et al., 2023)
Also Read: Sore Throat and Stiff Neck: When to Worry
Medical Management: What Happens Before Rehabilitation
Treatment primarily involves anti-tubercular therapy for 6 to 9 months.
In some cases:
- Surgical drainage is required
- Drug-resistant TB may prolong treatment
Recent studies indicate a growing concern regarding drug-resistant forms of extrapulmonary TB, including lymph node involvement (Hossain MB et al., 2025)
From a physiotherapy standpoint, this means patients may present with prolonged inactivity and more severe tissue changes.
Read about: Neck And Jaw Pain Together? Here’s The Full Clinical Picture
The Real Challenge: What Happens After Treatment
This is where most discussions end, but clinically, this is where rehabilitation begins.
Even after infection resolves:
- Tissue elasticity is reduced
- Fibrotic bands develop
- Muscle guarding persists
- Movement becomes restricted
These changes are not always painful initially, but they affect function over time.
Also Read: Neck Pain When Coughing: Causes, Relief, and When to Worry
Role of Physiotherapy in Scrofula Rehabilitation
From a physiotherapist’s point of view, scrofula is not just an infection. It becomes a post-inflammatory musculoskeletal condition affecting the neck.
1. Restoring Tissue Mobility
Fibrosis following tuberculosis is often dense and restrictive.
Effective techniques include:
- Myofascial release
- Scar mobilization
- Skin rolling
These techniques help restore normal tissue glide, which is essential for movement.
Read about: What Is Cervical Myofascial Pain Syndrome And How To Relieve Trigger Points
2. Cervical Movement Re-education
Rather than only focusing on stretching, rehabilitation should include:
- Controlled cervical rotations
- Segmental mobility exercises
- Activation of deep cervical flexors
Research on neck dysfunction shows that improper muscle activation patterns can persist long after the initial condition resolves (Falla D et al., 2018)
Read: Simple Posture Correction Exercises for Forward Head Posture
3. Postural Correction
Long-standing neck swelling often leads to:
- Forward head posture
- Rounded shoulders
- Muscle imbalance
Corrective strategies include:
- Strengthening deep stabilizers
- Scapular control exercises
- Ergonomic adjustments
Read in detail: Best Ergonomic Desk Setup to Reduce Neck and Back Pain
4. Managing Scar and Post-Surgical Adhesions
In cases involving surgical intervention:
- Prevent adhesion formation
- Maintain tissue flexibility
- Gradually restore stretch tolerance
This is crucial to avoid long-term restriction.
Read: Spasm In Neck: What Causes It & How to Fix It Fast
5. Addressing Persistent Pain and Discomfort
Some patients report ongoing symptoms such as:
- Pulling sensation
- Deep dull ache
- Mild numbness
These are often due to:
- Residual fibrosis
- Nerve irritation
- Altered biomechanics
Read : How to Treat Neck Pain in Ankylosing Spondylitis
Psychological Impact That Often Goes Unnoticed
Visible scars or neck deformities can affect:
- Self-confidence
- Social interaction
- Emotional well-being
Improving posture and physical appearance through rehabilitation often contributes positively to mental health, even if indirectly.
Read about: Effective Neck Pain Exercises At Home: A Complete Guide to Relief and Improved Mobility
When Should Physiotherapy Begin
Timing is important.
Rehabilitation should begin only when:
- Infection is controlled
- No active discharge is present
- Pain levels are manageable
Starting too early may worsen inflammation and delay healing.
Read about: Yoga for Neck Pain: Poses That Actually Work
Common Mistakes Patients Make During Recovery
One thing I often notice in practice is that recovery from scrofula is not delayed because of the disease itself, but because of small, avoidable mistakes during the healing phase.
Being aware of these can make a noticeable difference in how quickly and comfortably you recover.
Here are some of the most common ones:
Starting neck exercises too early
Many patients begin stretching as soon as the swelling reduces. If done before the infection is fully controlled, this can increase irritation and delay healing.
Ignoring mild stiffness
A slight restriction in movement may not seem important initially, but over time it can develop into persistent tightness if not addressed early.
Avoiding movement out of fear
Some patients keep their neck completely still to “protect” it. This often leads to more stiffness and muscle weakness rather than recovery.
Not addressing scar tissue
Once the wound heals, the focus shifts away from the area. However, untreated scar tissue can silently restrict movement and cause long-term discomfort.
Poor posture during recovery
Spending long hours with a forward head posture, especially on phones or laptops, can worsen neck strain and slow down rehabilitation.
Stopping physiotherapy too early
As soon as pain reduces, many patients discontinue exercises. This is one of the biggest reasons why stiffness returns later.
A simple way to think about recovery is this:
Healing does not end when the swelling disappears. It continues until normal movement and function are fully restored.
Read About: How to Choose the Right and Best Pillow for Neck Pain
Nutrition and Recovery
Nutritional status plays a major role in recovery from tuberculosis.
Key factors include:
- Adequate protein intake
- Vitamin C for tissue repair
- Zinc for immune function
Malnutrition has been strongly associated with delayed healing and poorer outcomes in TB patients (World Health Organization, 2023)
Read more: Is Cervical Traction For Neck Pain Really Effective
Prognosis and Long-Term Outcomes
With proper medical treatment and structured rehabilitation:
- Neck mobility improves
- Pain reduces
- Functional recovery is achievable
Without physiotherapy:
- Stiffness may persist
- Movement remains restricted
- Quality of life is affected
Read about: How to Relieve Morning Neck Stiffness Naturally
Final Thoughts from a Physiotherapist
Scrofula is often treated as a condition that ends with medication, but in reality, recovery continues beyond infection control.
What I have consistently observed is this:
Patients who engage in guided rehabilitation regain movement faster, experience less discomfort, and return to normal life with greater confidence.
Physiotherapy does not replace medical treatment, but it completes the recovery process.
Also Read : Neck Cracking: Benefits, Risks, and the Truth About Stroke
Frequently Asked Questions
1. What is scrofula?
Scrofula is a type of tuberculosis that affects the lymph nodes in the neck, leading to painless swelling and possible long-term stiffness.
2. Is scrofula contagious?
The condition itself is not directly contagious, but the underlying tuberculosis infection can spread through airborne droplets.
3. Can scrofula be cured completely?
Yes, with proper anti-tubercular treatment and rehabilitation, most patients recover well.
4. Is physiotherapy necessary after scrofula?
Yes, physiotherapy helps restore neck mobility, reduce stiffness, and improve overall function.
5. How long does recovery take?
Medical treatment usually takes 6 to 9 months, while physical recovery depends on rehabilitation consistency.
6. Can scrofula cause permanent damage?
If not properly managed, it can lead to fibrosis, scarring, and long-term stiffness.
7. When should exercises begin?
Exercises should start only after infection is controlled and under professional guidance.
8. Does scrofula come back?
Recurrence is possible, especially in cases of incomplete treatment or weakened immunity.











