Occipital neuralgia is a nerve pain condition affecting the back of the head, where occipital nerve pain relief at home can help ease symptoms early.
It is a neuropathic pain condition involving irritation or compression of the occipital nerves (greater, lesser, or third), which originate from the upper cervical spine and supply sensation to the back of the head.
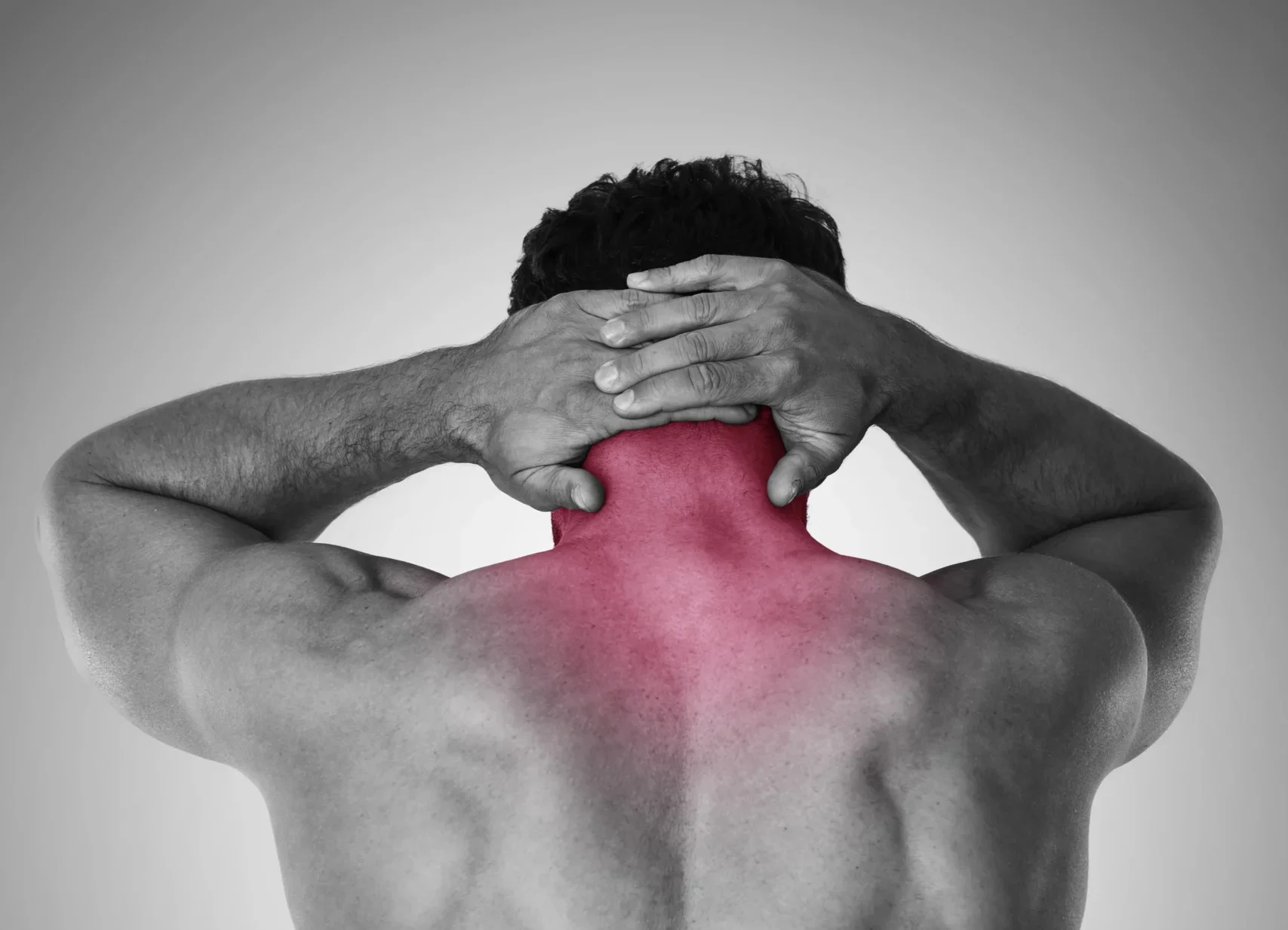
It is characterized by sharp, shooting, electric-like pain that begins at the base of the skull and may radiate toward the scalp, forehead, or behind the eyes. (NCBI)
Unlike migraines or tension headaches, occipital neuralgia is primarily a nerve disorder, not a vascular or muscular headache, though musculoskeletal factors often contribute.
From a physiotherapy perspective, this condition is deeply connected to upper cervical biomechanics, muscle tension, and postural dysfunction.
Thus makes it highly relevant in modern sedentary lifestyles.
Quick Answer
Occipital neuralgia is a nerve-related condition causing sharp, shooting pain at the back of the head due to irritation or compression of occipital nerves. It is commonly linked to poor posture, muscle tightness, or cervical spine issues and can be effectively managed with physiotherapy, posture correction, and targeted exercises.
Key Takeaways
- Occipital neuralgia is caused by nerve compression, not just headache triggers
- Poor posture is one of the biggest hidden causes
- Physiotherapy plays a crucial role in long-term relief
- Symptoms often mimic migraines but require different treatment
- Early intervention prevents chronic pain cycles
Anatomy You Must Understand
The greater occipital nerve (GON) accounts for nearly 90% of occipital neuralgia cases and passes through tight muscular tunnels such as the trapezius and semispinalis capitis. (NCBI)
This anatomical pathway explains why:
- Muscle tightness → nerve compression
- Poor posture → mechanical irritation
- Repetitive strain → chronic inflammation
Research shows that friction, pressure, or inflammation along these nerve pathways is a key mechanism behind symptoms. (PMC)
Clinical pearl: Most patients are not aware that their “head pain” may actually originate from the neck and upper back dysfunction.
Occipital Neuralgia Causes
1. Mechanical Compression
- Tight suboccipital muscles
- Cervical spine stiffness
- Fascial restrictions
2. Poor Posture & Digital Lifestyle
Forward head posture increases strain on upper cervical structures, leading to nerve irritation.
3. Cervical Spine Disorders
- Osteoarthritis
- Disc degeneration
- Upper cervical instability
4. Trauma or Injury
- Whiplash injuries
- Falls or sports impact
5. Systemic Conditions
- Diabetes-related neuropathy
- Inflammatory diseases
6. Repetitive Microstrain
Sustained screen use or desk work can gradually compress the occipital nerves.
Many cases remain idiopathic, meaning no single cause is identified, but underlying biomechanical contributors are almost always present. (Verywell Health)
Symptoms of Occipital Neuralgia
Classic Symptoms
- Sharp, stabbing, or electric pain at the back of the head
- Pain radiating to scalp, forehead, or eyes
- Tenderness at base of skull
Associated Symptoms
- Burning or throbbing sensation
- Scalp sensitivity (even brushing hair hurts)
- Pain triggered by neck movement
Lesser-Known Signs
- Reduced sensation or numbness in scalp
- Pain mimicking migraine but without aura
- Pain worsened by posture
Pain episodes are typically brief (seconds to minutes) but can recur frequently. (NCBI)
Why Occipital Neuralgia Is Often Misdiagnosed
Many patients are incorrectly treated for:
- Migraine
- Tension headache
- Cervicogenic headache
This happens because symptoms overlap significantly.
The key differentiator:
Occipital neuralgia pain is nerve-based (sharp, shooting), not pressure-based.
Diagnosis: What Confirms It?
Clinical Examination
- Palpation of occipital nerve
- Reproduction of symptoms
Diagnostic Nerve Block
If pain disappears after anesthetic injection → confirms diagnosis. (NCBI)
Imaging (if needed)
- MRI
- CT scan
Used to rule out structural causes.
Physiotherapy Role
Many conventional treatments focus on medications, but fail to address the root mechanical causes.
Physiotherapy plays a central role by targeting:
- Muscle imbalance
- Joint dysfunction
- Postural strain
- Neural sensitivity
Evidence supports a mechanism-based approach, focusing on musculoskeletal contributors and patient education. (Physiopedia)
Physiotherapy Treatment for Occipital Neuralgia
1. Postural Correction
Correcting forward head posture reduces load on occipital nerves.
Key Strategies:
- Chin tucks
- Ergonomic adjustments
- Screen height correction
2. Suboccipital Muscle Release
Tight suboccipital muscles are a major cause of nerve compression.
Techniques:
- Manual therapy
- Self-release using massage ball
- Myofascial release
3. Cervical Mobility Exercises
Improves joint function and reduces nerve irritation.
Exercises:
- Neck rotations
- Side bending stretches
- Upper cervical mobilization
4. Nerve Desensitization Techniques
Gentle exposure reduces nerve hypersensitivity.
5. Strengthening Deep Neck Flexors
Weak stabilizers increase strain on superficial muscles.
Example:
- Chin tuck with hold (10 seconds × 10 reps)
6. Scapular Stabilization
Upper back weakness indirectly increases cervical strain.
Exercises:
- Scapular retraction
- Wall angels
- Resistance band rows
Advanced & Medical Treatment Options
Medications
- NSAIDs
- Antidepressants
- Anticonvulsants (NCBI)
Nerve Blocks
Used for both diagnosis and treatment.
Radiofrequency Therapy
Helps reduce nerve signaling.
Occipital Nerve Stimulation
Used in chronic, resistant cases with promising outcomes. (SpringerLink)
Surgery (Rare)
Only for severe compression cases.
Evidence-Based Insights
- Occipital neuralgia is primarily caused by nerve compression rather than inflammation alone. (NCBI)
- Conservative treatments like physiotherapy alone may not outperform placebo unless mechanism-specific interventions are used. (NCBI)
- Multimodal treatment (physio + medical) shows better outcomes. (Physiopedia)
- Emerging therapies like nerve stimulation show significant improvement in refractory cases. (SpringerLink)
Lesser-Known Facts
- It is considered a rare condition, often underdiagnosed. (Physiopedia)
- Pain can radiate to the eyes due to trigeminocervical connections. (Physiopedia)
- Poor posture alone can trigger symptoms without any injury
- Even tight hairstyles or helmet pressure can aggravate it
Daily Habits That Can Worsen Occipital Neuralgia
- Long screen time
- Sleeping with high pillows
- Poor ergonomics
- Stress-induced muscle tension
Home Care Tips
- Apply warm compress to neck
- Maintain neutral spine posture
- Use cervical support pillow
- Take frequent breaks from screens
- Practice relaxation breathing
My Clinical Insight
Most patients I see with occipital neuralgia are not suffering from a “random nerve issue”, they are experiencing the consequences of years of poor posture, muscle imbalance, and cervical overload.
Treating only pain without correcting biomechanics leads to recurrence.
Physio Prescription
- Daily chin tuck exercises
- Upper back strengthening (3-4 times/week)
- Ergonomic workstation setup
- Suboccipital release (daily)
- Avoid prolonged neck flexion
Red Flags
- Sudden severe headache (worst ever)
- Vision loss or neurological symptoms
- Fever with neck stiffness
- Progressive worsening
Myth vs Reality
Myth: It’s just a type of headache
Reality: It is a nerve disorder requiring targeted treatment
Final Word
Occipital neuralgia is not just pain, it is a signal from your nervous system that something is mechanically wrong.
Early intervention with physiotherapy, posture correction, and targeted exercises can not only relieve symptoms but prevent recurrence and chronicity.
Don’t ignore early signs, start occipital nerve pain relief at home to avoid chronic discomfort.
Frequently Asked Questions
1. Can occipital neuralgia go away on its own?
Mild cases may improve, but most require treatment to prevent recurrence.
2. Is occipital neuralgia serious?
It is not life-threatening but can significantly affect quality of life.
3. How is it different from migraine?
It causes sharp nerve pain, unlike throbbing vascular migraine pain.
4. Can physiotherapy cure it?
Physiotherapy can significantly reduce symptoms and address root causes.
5. What triggers flare-ups?
Poor posture, stress, and prolonged screen use are common triggers.
6. Is exercise safe?
Yes, if guided properly—avoid aggressive neck movements.
7. Can sleep position affect it?
Yes, improper pillow height can worsen symptoms.
8. When should I see a doctor?
If symptoms are severe, persistent, or worsening.
Stay tuned with us for more health related topics.
Follow us on LinkedIn and Instagram for more.
Medical Disclaimer!
This article has been reviewed and written under the guidance of our Head Physiotherapist, Dr. Kruti Raj (PT, MUHS,CPT,CMPT). The information shared is intended for educational purposes only and should not be considered a substitute for personalized medical advice, diagnosis, or treatment.
Please consult us or any other qualified healthcare professional before beginning any exercise program, especially if you are experiencing pain, recovering from injury, or managing a medical condition.











