What is Thoracic Outlet Syndrome and why does it get missed so often
If you have ever felt tingling in your hand, heaviness in your arm, or a strange pulling sensation from your neck to your fingers, you might have been told it is just posture or maybe even stress.
Many patients hear that in the beginning.
But sometimes, there is something more specific going on.
One condition that often hides behind these vague symptoms is Thoracic Outlet Syndrome, commonly called TOS.
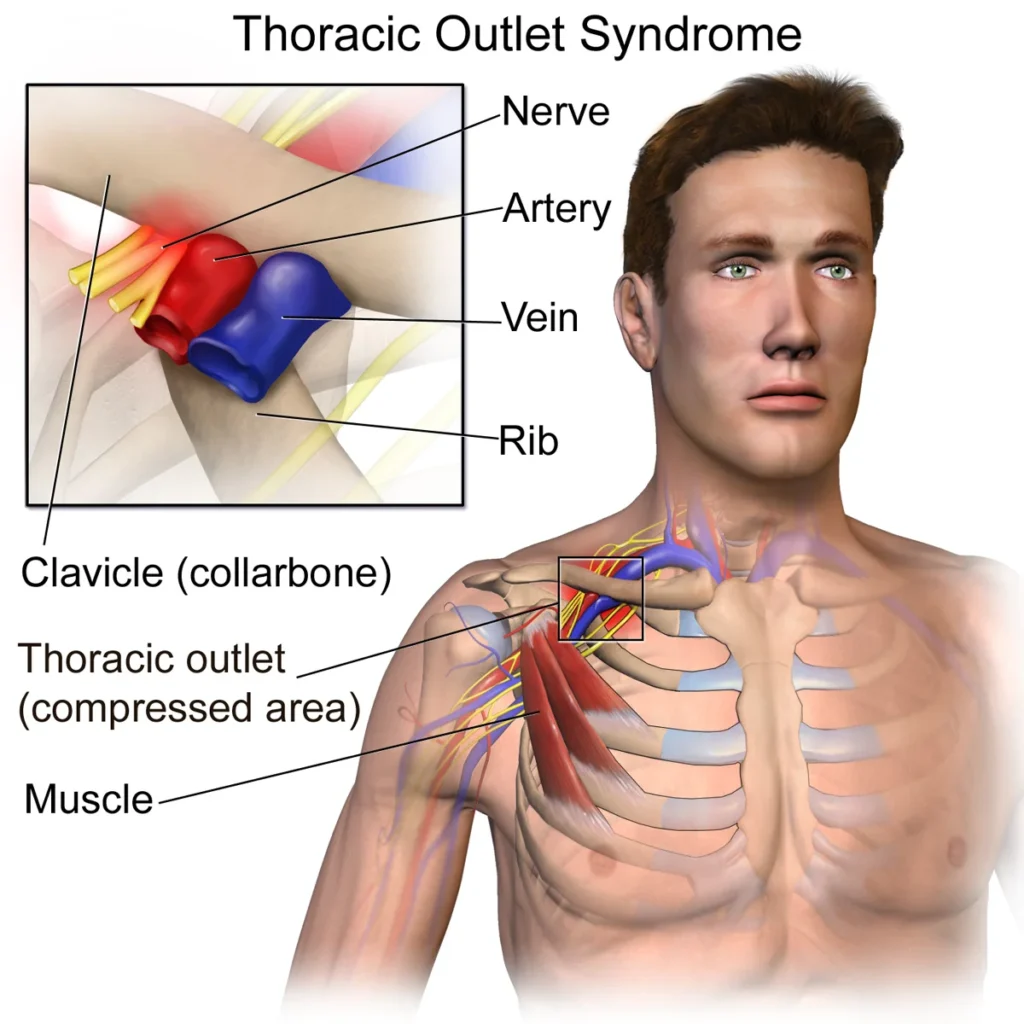
The thoracic outlet is a narrow space between your collarbone and your first rib. Through this small area pass important nerves and blood vessels that supply your arm.
When this space becomes tight or compromised, these structures get compressed. That is when symptoms begin.
What makes TOS difficult is that it does not always show up clearly in scans. In fact, many patients go from doctor to doctor before getting a clear answer.
A recent review highlighted that diagnosis of TOS still relies heavily on clinical judgment because imaging alone is not always sufficient. (Hooper et al., 2010)
Read about our Complete Neck Pain Guide : Causes, Symptoms, Exercises and Treatment
Quick Answer
Thoracic Outlet Syndrome (TOS) is a condition where nerves or blood vessels are compressed between the collarbone and first rib, leading to symptoms like arm tingling, numbness, and weakness.
In most cases, physiotherapy is highly effective and focuses on posture correction, muscle balance, and nerve mobility. Early treatment and consistent habit changes can significantly improve recovery without the need for surgery.
Read about : 15 Common Causes of Neck Pain You Should Know
Key Takeaways
- Thoracic Outlet Syndrome is commonly caused by posture and muscle imbalance rather than structural issues
- Tingling, numbness, and arm heaviness are early signs that should not be ignored
- Physiotherapy is the first line of treatment and works well in most cases
- Posture correction and daily habit changes are just as important as exercises
- Breathing patterns can influence symptoms more than most people realize
- Consistency in treatment is more important than intensity
- Most patients recover within weeks if managed early and correctly
Read in detail about: How to Fix Upper Crossed Syndrome Naturally
Types of Thoracic Outlet Syndrome
From a clinical perspective, TOS is divided into three main types. Understanding this helps in both diagnosis and treatment.
Neurogenic TOS
This is the most common type. It involves compression of the brachial plexus, which is the network of nerves supplying the arm.
Typical signs include tingling, numbness, and weakness.
Studies suggest that around 90 percent of cases fall into this category. (Atasoy, 2010)
Venous TOS
This affects the veins. You may notice swelling, a heavy feeling, or a bluish discoloration in the arm.
Arterial TOS
This is rare but more serious. It involves arterial compression and may cause coldness, pallor, or reduced pulse in the hand.
Read about: Cervical Ligament Injury or Neck Ligament Tear
Why Thoracic Outlet Syndrome develops
Textbooks often focus on structural causes. In clinical practice, the story is usually different.
Most patients I see do not have a structural defect. They have a functional problem that developed over time.
Posture plays a bigger role than people realize
Forward head posture and rounded shoulders reduce the available space in the thoracic outlet.
I often see patients who sit for long hours, slightly leaning forward, unaware of how much strain they are putting on their neck and shoulder region.
Over time, this posture becomes their normal.
Read: Spasm In Neck: What Causes It & How to Fix It Fast
Muscle imbalance is a key factor
Certain muscles become tight and overactive:
- Scalenes in the neck
- Pectoralis minor in the chest
At the same time, stabilizing muscles become weak:
- Lower trapezius
- Rhomboids
- Serratus anterior
This imbalance creates a narrowing effect in the thoracic outlet.
Repetitive activity and lifestyle habits
Athletes who perform overhead movements are at risk, but so are office workers who keep their arms in one position for hours.
Even carrying a heavy bag on one side regularly can contribute.
Trauma and past injuries
Whiplash injuries and clavicle fractures can change biomechanics and increase the likelihood of compression.
Read in detail: Whiplash Injury After An Accident? Here’s Treatment And Expert Rehab Guide
Symptoms that patients often ignore in the early stage
One of the biggest challenges with TOS is that the symptoms do not always look serious at first.
Patients often describe:
- Tingling in the fingers
- A feeling of heaviness in the arm
- Mild weakness in grip
- Neck and shoulder discomfort
There are also patterns that are very telling:
- Symptoms increase by evening
- Arm feels worse when raised
- Relief is felt when lying down
Many people ignore these signs until they start interfering with daily tasks.
Read in detail about: Cervical Radiculopathy: Why Neck Nerve Pain Travels to the Arm
Red flags you should not ignore
Not every tingling or arm discomfort is Thoracic Outlet Syndrome.
This is something I always clarify with patients, because similar symptoms can come from completely different conditions.
There are certain warning signs that should not be ignored:
- Sudden and severe weakness in the arm or hand
- Difficulty holding or gripping objects without dropping them
- Symptoms affecting both arms at the same time
- Pain that does not change with posture or movement
- History of recent trauma followed by worsening symptoms
Sometimes, cervical spine issues or nerve root compression can present in a very similar way.
If your symptoms feel unusual or are rapidly progressing, it is always better to get a proper medical evaluation instead of assuming it is TOS.
Read more: Rheumatoid Arthritis Neck: Causes, Symptoms and Treatments
Diagnosis Of TOS
Diagnosis is not about one test. It is about connecting multiple observations.
In clinic, I look at:
- Posture and alignment
- Movement patterns
- Muscle tightness and weakness
- Neural sensitivity
Special tests like Roos test or Adson’s test can give clues, but they are not definitive on their own.
Recent literature confirms that diagnosis of TOS requires a combination of clinical findings and imaging, not a single test. (Balderman et al., 2019)
Interestingly, improvement with physiotherapy itself often helps confirm the diagnosis.
Read about: Effective Neck Pain Exercises At Home: A Complete Guide to Relief and Improved Mobility
Physiotherapy treatment that actually works
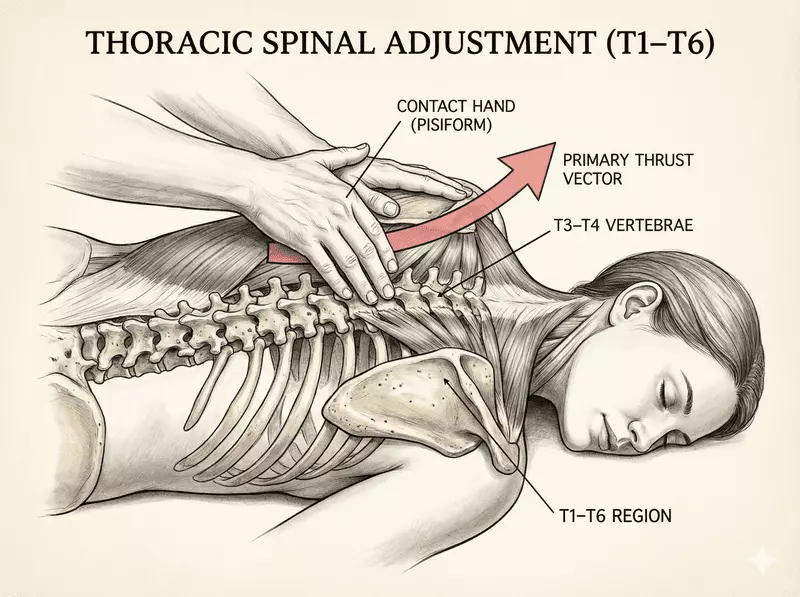
The good news is that most cases improve without surgery when managed correctly.
A recent study showed significant symptom reduction and functional improvement after structured physiotherapy.
(Elwi et al., 2024)
Posture correction is the foundation
This is not just about sitting straight for a few minutes.
It involves retraining your body:
- Chin tuck exercises (Learn : How to do Chin Tucks for Neck Pain Relief and Posture Correction)
- Scapular setting
- Awareness of daily posture
Stretching tight structures
Targeted stretching helps reduce compression:
- Scalene stretch
- Pectoralis minor stretch
- Upper trapezius stretch
These should be gentle and consistent.
Strengthening the right muscles
This is where long term change happens.
Focus on:
- Lower trapezius
- Rhomboids
- Serratus anterior
When these muscles activate properly, they help open the thoracic outlet.
Exercises:
- Chin tucks
- Scapular retraction
- Wall angels
- Resistance band rows
Helps maintain open thoracic outlet space.
Nerve gliding exercises
These are often overlooked but very effective.
They help improve nerve mobility and reduce irritation.
Examples:
- Median nerve glide
- Ulnar nerve glide
Read more on : Manual Therapy for Neck Pain: A Physiotherapist’s Evidence Based Guide
Manual therapy
Hands on techniques can provide relief early in treatment:
- Soft tissue release
- Joint mobilization
- Trigger point therapy
Read about: What Is Cervical Myofascial Pain Syndrome And How To Relieve Trigger Points
Thoracic Mobility Exercises
Improving upper back mobility reduces strain on the neck.
Exercises:
- Thoracic extensions
- Foam roller mobility drills
- Cat-cow movements
Helps restore natural posture and alignment.
Read: How to do Cat Cow Stretch Exercises
Taping & Support
Kinesiology taping can:
- Improve posture awareness
- Reduce muscle overload
Electrotherapy (Adjunct)
Used for pain relief:
- TENS
- Ultrasound therapy
Not primary treatment, but helpful in acute pain.
Advanced Physiotherapy Techniques
Dry Needling
- Releases trigger points in tight muscles
Myofascial Decompression (Cupping)
- Improves tissue mobility
A small clinical observation that changes everything
I have noticed something interesting over the years.
Patients are very consistent with exercises for a few days. Then they return to the same habits.
Sitting the same way. Using the laptop the same way. Sleeping with the arm overhead.
The symptoms return, and it feels like the treatment did not work.
But the issue is not the exercises. It is the overall movement pattern.
TOS improves when daily habits change, not just when exercises are done.
Read: 10 Proven Home Remedies for Neck Pain from Anxiety
The role of breathing which is often overlooked
This is something that is rarely discussed but makes a real difference.
Many people use shallow chest breathing, especially when stressed.
This activates accessory muscles like the scalenes, which are already tight in TOS.
Over time, this increases compression.
Teaching diaphragmatic breathing helps reduce unnecessary muscle tension and improves outcomes.
Also Read: Ultimate 6 Weeks Neck Rehabilitation Exercises For Pain Relief
Simple home routine that patients can actually follow
A simple and realistic routine works better than a complicated one.
Daily plan:
- Chin tucks 10 repetitions
- Scapular retractions 15 repetitions
- Pec stretch hold for 30 seconds
- Nerve glides 10 repetitions
Consistency matters more than intensity.
Read in detail: Best Ergonomic Desk Setup to Reduce Neck and Back Pain
Ergonomic changes that reduce symptoms faster than expected
Many patients improve significantly with small adjustments:
- Screen at eye level
- Proper chair support
- Avoiding prolonged static posture
- Taking short breaks every 30 to 40 minutes
These changes reduce stress on the thoracic outlet throughout the day.
Read about: Which Is The Best Sitting Posture To Avoid Neck Pain And How To Achieve It
When surgery becomes necessary
Surgery is not the first option.
It is usually considered in:
- Severe vascular cases
- Structural abnormalities
- Cases not responding to conservative care
Even in these situations, physiotherapy plays an important role before and after surgery. (Sanders et al., 2007)
Read About: How to Choose the Right and Best Pillow for Neck Pain
Lesser known facts about Thoracic Outlet Syndrome
- It is often mistaken for cervical spine problems
- Women are affected more frequently
- Stress can worsen symptoms due to muscle tension
- Sleeping posture can aggravate symptoms
- Carrying uneven loads can trigger flare ups
Read About: Best Sleeping Position for Neck Pain: A Physiotherapist’s Complete Guide
Common mistakes that slow down recovery
This is something I notice quite often during follow ups. Patients start feeling better, then unknowingly slip back into the same routine that caused the issue.
A few common patterns:
- Doing exercises for a few days and then stopping
- Paying attention to posture only during exercise time
- Stretching too aggressively instead of gradually
- Going back too soon to gym or overhead activities
- Sitting for long hours without breaks
Thoracic Outlet Syndrome does not improve just with exercises alone.
It improves when daily habits change along with treatment. Even small corrections done consistently can make a noticeable difference.
Also read: How to Relieve Neck Tightness Without Equipment
Recovery timeline and expectations
Recovery depends on how early the condition is addressed and how consistent the patient is.
- Mild cases improve in 4 to 6 weeks
- Moderate cases may take 8 to 12 weeks
- Chronic cases take longer but still improve
The key factor is adherence to both exercises and lifestyle changes.
Read about: How to Relieve Morning Neck Stiffness Naturally
Prevention
Prevention is practical and achievable:
- Maintain good posture
- Strengthen upper back muscles
- Avoid prolonged static positions
- Stay physically active
- Be aware of daily habits
Read : Chiropractic for Neck Pain: Does It Really Work?
Conclusion
Thoracic Outlet Syndrome is one of those conditions that can quietly affect daily life without being clearly identified.
But when approached correctly, it responds very well to physiotherapy.
The focus should not only be on relieving symptoms but also on correcting the underlying movement patterns that caused the problem.
If you are experiencing persistent arm discomfort, it is worth getting it assessed early. The earlier the intervention, the better the outcome.
Also Read : Neck Cracking: Benefits, Risks, and the Truth About Stroke
Frequently Asked Questions (FAQs)
1. What is Thoracic Outlet Syndrome?
Thoracic Outlet Syndrome is a condition where nerves or blood vessels are compressed between the collarbone and first rib, causing symptoms in the arm and shoulder.
2. Can physiotherapy completely cure TOS?
In most cases, physiotherapy can significantly reduce or completely resolve symptoms when done consistently.
3. How do I know if my arm pain is TOS?
If your symptoms increase with posture changes or arm position and include tingling or numbness, it may be TOS, but proper assessment is needed.
4. Which exercises are best for TOS?
Chin tucks, scapular strengthening, stretching of chest muscles, and nerve gliding exercises are commonly recommended.
5. Can gym workouts worsen Thoracic Outlet Syndrome?
Yes, especially overhead exercises or poor form can increase compression and worsen symptoms.
6. Is surgery always required for TOS?
No, surgery is only considered in severe or non responsive cases. Most people improve with physiotherapy.
Stay tuned with us for more health related topics.
Follow us on LinkedIn and Instagram for more.
Medical Disclaimer!
This article has been reviewed and written under the guidance of our Head Physiotherapist, Dr. Kruti Raj (PT, MUHS,CPT,CMPT). The information shared is intended for educational purposes only and should not be considered a substitute for personalized medical advice, diagnosis, or treatment.
Please consult us or any other qualified healthcare professional before beginning any exercise program, especially if you are experiencing pain, recovering from injury, or managing a medical condition.











