In clinical practice, Klippel-Feil Syndrome rarely walks in with a label. It shows up as something much more ordinary.
A patient complains of constant neck tightness. Someone else struggles to turn their head while driving. Another mentions uneven shoulders that have been ignored for years.
Only later, often through imaging, does the underlying reality become clear.
Two or more cervical vertebrae are fused. What seemed like a simple postural issue turns out to be something present since birth.
Klippel-Feil Syndrome is a congenital condition where segments of the cervical spine fail to separate during early development.
But reducing it to just “fused vertebrae” misses the bigger picture. What really matters is how the body adapts to that fusion over time.
Read about our Complete Neck Pain Guide : Causes, Symptoms, Exercises and Treatment
Quick Answer
Klippel-Feil Syndrome is a congenital condition where cervical vertebrae are fused, leading to reduced neck mobility and compensatory stress on surrounding joints. Physiotherapy focuses on posture correction, mobility, and strength to improve function and prevent complications.
Read about: Early Signs of Cervical Spine Damage You Should Never Ignore
Key Takeaways
- Klippel-Feil Syndrome is often diagnosed late due to subtle symptoms.
- It affects more than just the neck and may involve other body systems.
- Adjacent joints compensate, leading to early degeneration.
- Physiotherapy is essential for long-term management.
- Posture and daily habits play a major role in symptom control.
Read : How to Treat Neck Pain in Ankylosing Spondylitis
Why Klippel-Feil Syndrome Often Goes Undiagnosed
One of the most overlooked aspects of this condition is how frequently it is missed.
Not every patient has the classic signs. The short neck, low hairline, and restricted movement triad may be incomplete or subtle.
Many individuals grow up without any clear diagnosis.
In fact, a growing body of clinical research suggests that Klippel-Feil Syndrome may be underdiagnosed because symptoms often appear much later in life. (Clarke et al. 1998)
I have seen patients in their late twenties or thirties who were treated repeatedly for muscle stiffness or posture-related pain.
The fusion was only discovered after persistent symptoms led to imaging.
This delay matters. By the time symptoms appear, the body has already spent years compensating.
Read about : 15 Common Causes of Neck Pain You Should Know
What Causes Klippel-Feil Syndrome
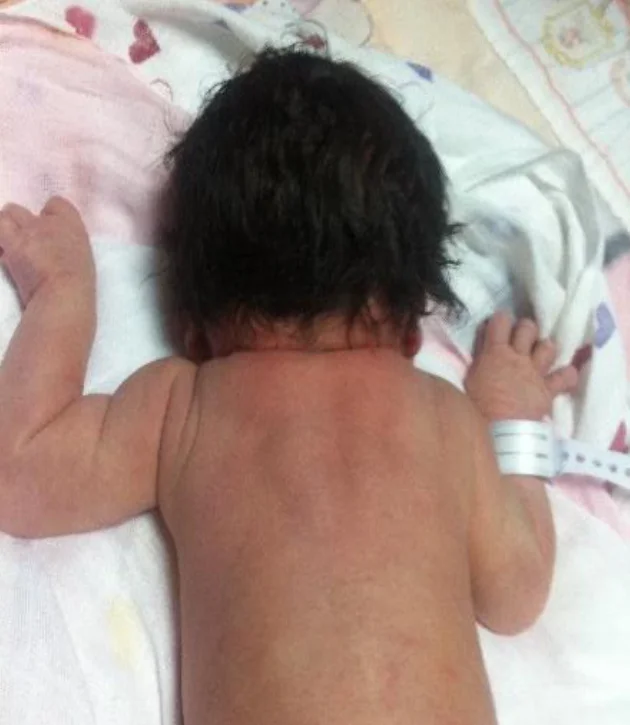
The condition originates during early fetal development, typically between the third and eighth week of gestation, when the cervical vertebrae are supposed to segment properly.
In some cases, genetic factors play a role. Mutations involving developmental genes such as GDF6 and GDF3 have been identified in certain patients. (Samartzis et al. 2006)
However, not all cases follow a clear genetic pattern. Many occur sporadically, which makes early prediction difficult.
Read more: Rheumatoid Arthritis Neck: Causes, Symptoms and Treatments
It Is Not Just a Neck Condition
One of the biggest misconceptions is that Klippel-Feil Syndrome only affects the cervical spine.
In reality, it can be associated with multiple systems in the body.
Patients may also present with:
- Hearing impairments
- Congenital heart conditions
- Kidney abnormalities
- Neurological variations
From a physiotherapy perspective, this changes how we assess patients.
It is not enough to focus only on the neck. A broader clinical screening is essential. (Pediatric Oncall 2023)
Read: What is Torticollis? How to treat neck tilt condition
Symptoms That Patients Actually Report
Textbooks list features like reduced neck movement or visible deformity, but real patients describe things differently.
They say:
- My neck always feels tight
- I cannot turn properly while reversing my car
- One shoulder feels higher than the other
- Pain increases after sitting for long hours
These lived experiences are often more telling than textbook definitions.
Common clinical findings include:
In some cases, neurological symptoms such as tingling or weakness may develop when nearby nerves are affected.
Read about : What is Cervical Facet Joint Pain, how it causes cervicogenic headaches and how to correct it naturally
Red Flags You Should Never Ignore
Most cases of Klippel-Feil Syndrome are manageable with conservative care, but there are certain symptoms that should never be brushed aside.
These are not “wait and watch” situations.
Watch for These Warning Signs:
- Sudden increase in neck pain that does not settle with rest
- Numbness, tingling, or weakness in arms or hands
- Difficulty with balance or coordination
- Loss of fine motor control, such as buttoning a shirt
- Persistent headaches associated with dizziness
- Any change in bladder or bowel control
Read more: Cervical Vertigo Explained: Why Neck Pain Make You Feel Dizzy
Why This Matters
These signs may indicate:
- Nerve compression
- Spinal cord involvement
- Progressive neurological changes
In such cases, continuing only exercises without further evaluation can delay necessary medical intervention.
Read in detail about: Cervical Radiculopathy: Why Neck Nerve Pain Travels to the Arm
Practical Advice
If any of these symptoms appear, the safest approach is:
- Pause aggressive exercises
- Seek medical evaluation
- Continue only gentle, guided movements
Read in detail about: Cervical Disc Degeneration: The Hidden Cause of your Neck Pain
What Is Happening Biomechanically
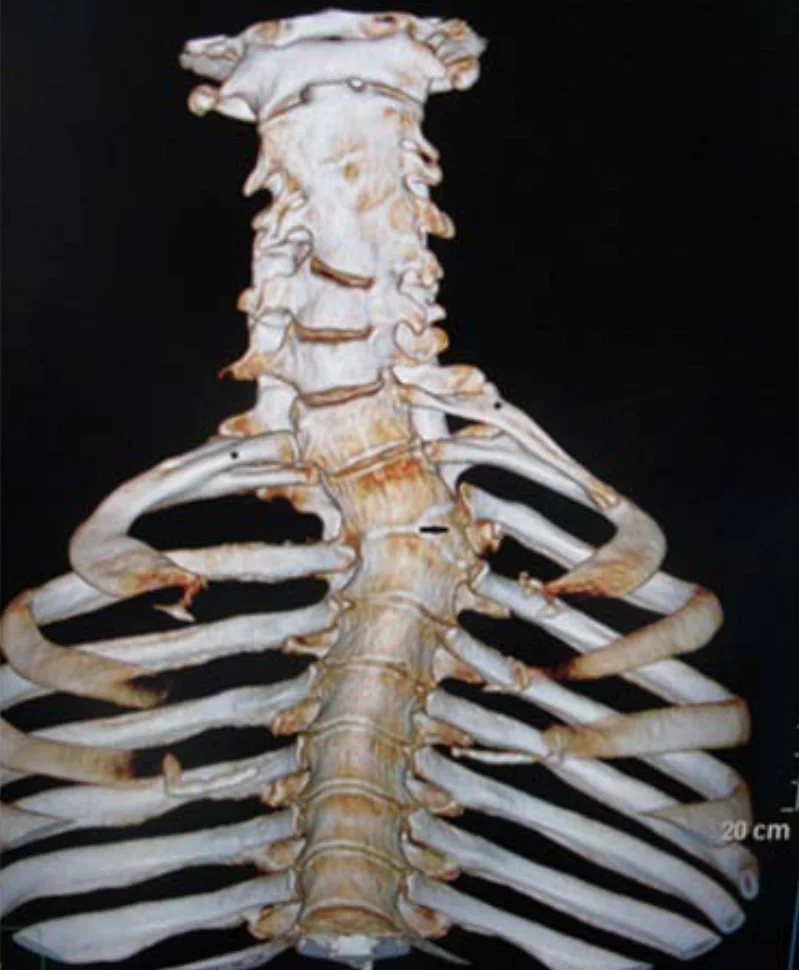
This is where things start to make sense.
When two vertebrae are fused, movement at that segment is lost. The body does not stop moving, so adjacent segments take on extra work.
Over time, this creates a chain reaction:
- Increased mobility in nearby joints
- Muscle overuse and fatigue
- Gradual wear and tear
- Early degenerative changes
This phenomenon explains why relatively young adults with Klippel-Feil Syndrome can present with symptoms similar to older individuals with cervical spondylosis.
Read in detail about: What is Cervical Spondylosis? The Truth Behind Chronic Neck Pain
New Understanding: Brain and Nerve Involvement
Recent neurological research has expanded our understanding beyond the structural aspect of the condition.
Some studies suggest that Klippel-Feil Syndrome may also involve neurodevelopmental components, influencing coordination and motor control. (Tracy et al. 2020)
Clinically, this can present as:
- Altered movement patterns
- Reduced coordination
- Chronic pain sensitivity
For physiotherapists, this means treatment is not only about joints and muscles. It also involves retraining how the nervous system controls movement.
Also read: How to Relieve Neck Tightness Without Equipment
Physiotherapy Assessment: Looking Beyond the Neck
A thorough assessment is never limited to the cervical spine.
In practice, I evaluate:
- Thoracic spine mobility
- Scapular positioning
- Muscle activation patterns
- Breathing mechanics
- Neurological signs
Many patients are surprised to learn that improving upper back mobility can significantly reduce neck strain.
Read about: What Is Military Neck Or Cervical Kyphosis And How To Treat It
What Actually Works in Physiotherapy
There is a big difference between textbook exercises and real-world management.
Read more: Which Is The Best Sitting Posture To Avoid Neck Pain And How To Achieve It
1. Load Management
Daily habits matter more than occasional exercises.
We address:
- Sitting posture
- Screen height
- Workstation setup
- Sleep positioning
Small changes here often bring significant relief.
Read more: Best Sleeping Position for Neck Pain: A Physiotherapist’s Complete Guide
2. Movement Quality Over Quantity
Doing more repetitions is not the goal. Moving correctly is.
Patients are trained to:
- Avoid compensatory patterns
- Use proper muscle activation
- Move within safe ranges
3. Focus on the Thoracic Spine
A stiff upper back often contributes more to neck discomfort than the cervical spine itself.
Improving thoracic mobility reduces stress on the neck.
4. Strengthening the Right Muscles
Key focus areas include:
- Deep neck flexors
- Scapular stabilizers
- Upper back musculature
These muscles help distribute load more efficiently.
5. Pain Education
One of the most important parts of rehabilitation is helping patients understand their pain.
Pain does not always mean damage. In many cases, it reflects sensitivity due to overuse or compensation.
Also Read: Ultimate 6 Weeks Neck Rehabilitation Exercises For Pain Relief
Evidence Supporting Physiotherapy
Recent case-based rehabilitation studies show that structured physiotherapy programs can significantly improve function, reduce pain, and enhance quality of life. (Tracy et al. 2020)
This reinforces the role of physiotherapy as a primary management strategy rather than just a supportive option.
Read about: Effective Neck Pain Exercises At Home: A Complete Guide to Relief and Improved Mobility
Activities That Need Caution
Patients with Klippel-Feil Syndrome should be mindful of certain activities.
These include:
- High-impact sports
- Contact sports
- Sudden neck movements
- Heavy overhead lifting
The goal is not restriction but intelligent activity modification.
Read about: Yoga for Neck Pain: Poses That Actually Work
Rare but Serious Complications
Although uncommon, certain complications require immediate attention.
These include:
- Spinal cord compression
- Progressive neurological deficits
- Myelopathy
In such cases, referral to a specialist is essential.
Ignoring these signs can lead to long-term consequences.
Read more: Cervical Myelopathy: The Hidden Neck Condition Affecting Your Walking
Living with Klippel-Feil Syndrome
This condition does not define a person’s capabilities, but it does require awareness.
The patients who do best are those who:
- Stay consistent with movement
- Avoid prolonged static postures
- Listen to their body
- Seek early intervention when symptoms change
Over time, they learn how to work with their body rather than against it.
Read more: Is Cervical Traction For Neck Pain Really Effective
Simple Daily Changes That Make a Big Difference
Most patients expect recovery to come only from exercises, but in reality, daily habits play a much bigger role.
These small adjustments often reduce symptoms more than any single exercise.
At Work or Desk
- Keep your screen at eye level to avoid forward head posture
- Use a chair that supports your upper back, not just lower back
- Take short movement breaks every 30 to 40 minutes
Read in detail: Best Desk Setup to Reduce Neck and Back Pain
While Using Phone
- Avoid bending your neck downward for long periods
- Bring the phone up to eye level instead
- Switch hands occasionally to reduce one-sided strain
Read in detail: Neck Pain from Phone Use? Here’s How to Treat Text Neck Syndrome
During Sleep
- Use a pillow that keeps your neck in a neutral position
- Avoid very high or very flat pillows
- Side or back sleeping is usually more comfortable than stomach sleeping
Read About: How to Choose the Right and Best Pillow for Neck Pain
During Travel or Driving
- Adjust mirrors so you do not need excessive neck rotation
- Use back support to maintain upright posture
- Take breaks during long journeys
Also Read : Neck Cracking: Benefits, Risks, and the Truth About Stroke
Conclusion
Klippel-Feil Syndrome is more than a structural anomaly. It is a lifelong interaction between anatomy, movement, and adaptation.
From a physiotherapy perspective, the focus is not on correcting the fusion but on optimizing everything around it.
When approached correctly, individuals can maintain mobility, reduce pain, and live fully active lives.
Read : Chiropractic for Neck Pain: Does It Really Work?
Frequently Asked Questions
1. What is Klippel-Feil Syndrome?
It is a congenital condition where two or more cervical vertebrae are fused, limiting neck movement.
2. Can it be diagnosed late in life?
Yes, many people are diagnosed in adulthood when symptoms appear.
3. Is physiotherapy effective?
Yes, it helps improve mobility, reduce pain, and prevent complications.
4. Can it cause nerve problems?
Yes, compression or irritation of nerves may lead to tingling or weakness.
5. Is surgery always required?
No, most cases are managed conservatively with physiotherapy.
6. Can I exercise safely?
Yes, but exercises should be guided by a professional.
7. Does it worsen over time?
It can, especially if compensatory strain is not managed.
Stay tuned with us for more health related topics.
Follow us on LinkedIn and Instagram for more.
Medical Disclaimer!
This article has been reviewed and written under the guidance of our Head Physiotherapist, Dr. Kruti Raj (PT, MUHS,CPT,CMPT). The information shared is intended for educational purposes only and should not be considered a substitute for personalized medical advice, diagnosis, or treatment.
Please consult us or any other qualified healthcare professional before beginning any exercise program, especially if you are experiencing pain, recovering from injury, or managing a medical condition.











