Cervical myelopathy is a neurological condition caused by compression of the spinal cord in the cervical spine, which is the neck region.
Unlike common neck pain that originates from muscles or joints, cervical myelopathy directly affects the spinal cord and can therefore influence movement, coordination, sensation and overall neurological function.
From a physiotherapist’s perspective, cervical myelopathy is one of the most important spinal disorders to identify early.
If the spinal cord remains compressed for a long time, permanent neurological damage can occur. Early recognition and proper treatment are therefore essential for preserving mobility and independence.
Degenerative cervical myelopathy is considered the most common cause of non traumatic spinal cord dysfunction in adults.
It develops gradually due to age related changes in the cervical spine such as disc degeneration, bone spur formation and ligament thickening that narrow the spinal canal. Smith et al. (2025)
Many patients initially experience subtle symptoms such as mild numbness in the hands or reduced hand coordination.
Because these early symptoms are often ignored, diagnosis may be delayed until neurological problems become more obvious.
Read about our Complete Neck Pain Guide : Causes, Symptoms, Exercises and Treatment
Quick Answer: What Is Cervical Myelopathy?
Cervical myelopathy is a neurological condition caused by compression of the spinal cord in the neck (cervical spine). This compression interferes with nerve signals traveling between the brain and the body.
Common symptoms include hand numbness, difficulty with coordination, balance problems, walking instability, and weakness in the arms or legs. The condition is most commonly caused by age-related degenerative changes in the cervical spine.
Early diagnosis is important because untreated cervical myelopathy may lead to permanent neurological damage. Treatment may include physiotherapy, lifestyle modification, and in moderate or severe cases, surgical decompression of the spinal cord.
Read About: Managing Neck Pain in Women: Home Exercises and Advice
Key Takeaways
- Cervical myelopathy occurs when the spinal cord becomes compressed in the cervical spine.
- Degenerative cervical spine changes are the most common cause of this condition.
- Early symptoms may include hand clumsiness, numbness, reduced coordination, and balance problems.
- Advanced cases may cause walking difficulty, muscle weakness, and bladder dysfunction.
- MRI is the most important diagnostic test to confirm spinal cord compression.
- Physiotherapy focuses on posture correction, cervical stabilization, balance training, and functional rehabilitation.
- Moderate to severe cervical myelopathy often requires surgical decompression followed by structured rehabilitation.
- Early diagnosis and treatment significantly improve long term outcomes and quality of life.
Read about: The Best Physiotherapy Exercises for Cervical Spondylosis Relief
What Happens in Cervical Myelopathy
The spinal cord is the main communication pathway between the brain and the rest of the body. It carries motor signals that control movement and sensory signals that transmit touch, pain and position information.
When the spinal cord is compressed in the cervical spine, several harmful processes can occur.
First, direct mechanical pressure interferes with nerve signal transmission.
Second, compression may reduce blood flow to the spinal cord, which leads to reduced oxygen supply and neuronal damage. Third, chronic inflammation can cause degeneration of nerve fibers.
Over time these changes can affect multiple neurological pathways, which explains why cervical myelopathy may cause problems with both hand function and walking ability. Sharma et al. (2025)
Read about : 15 Common Causes of Neck Pain You Should Know
Causes of Cervical Myelopathy
Several structural problems in the cervical spine can lead to spinal cord compression.
Degenerative Cervical Spondylosis
This is the most common cause of cervical myelopathy. As people age, cervical discs gradually lose hydration and height. This can lead to the formation of bone spurs and thickening of ligaments inside the spinal canal.
These changes reduce the space available for the spinal cord and may compress it.
Read in detail about: What is Cervical Spondylosis? The Truth Behind Chronic Neck Pain
Cervical Disc Herniation
A herniated disc may protrude backward into the spinal canal and press directly on the spinal cord.
Read in detail about: Cervical Disc Degeneration: The Hidden Cause of your Neck Pain
Ossification of Spinal Ligaments
In some individuals the posterior longitudinal ligament becomes calcified and thickened. This condition further narrows the spinal canal and increases the risk of spinal cord compression.
Read about: Cervical Ligament Injury or Neck Ligament Tear
Congenital Spinal Canal Narrowing
Some people are born with a relatively narrow cervical spinal canal. Even mild degenerative changes can cause spinal cord compression in these individuals.
Read in detail about: Cervical Radiculopathy: Why Neck Nerve Pain Travels to the Arm
Trauma
Falls, sports injuries and road traffic accidents may cause acute cervical spinal cord compression.
Read in detail: Whiplash Injury After An Accident? Here’s Treatment And Expert Rehab Guide
Risk Factors for Cervical Myelopathy
Certain factors increase the likelihood of developing cervical myelopathy.
These include:
- age above fifty years
- chronic cervical spondylosis
- congenital spinal canal narrowing
- previous neck trauma
- repetitive neck strain
- prolonged forward head posture
Modern lifestyle habits such as prolonged smartphone use and laptop work may accelerate degenerative changes in the cervical spine. Thompson et al. (2024)
Read in detail: Neck Pain from Phone Use? Here’s How to Treat Text Neck Syndrome
Common Symptoms of Cervical Myelopathy

Symptoms of cervical myelopathy usually develop gradually and may vary depending on the severity of spinal cord compression.
Neck Symptoms
Some patients experience neck stiffness or mild neck pain. However neck pain may not always be present.
Hand Symptoms
One of the earliest signs is reduced hand coordination. Patients may report:
- difficulty buttoning clothes
- dropping objects frequently
- numbness or tingling in the hands
- reduced grip strength
Arm Weakness
Compression of motor pathways can cause weakness in the arms or difficulty lifting objects.
Walking Difficulty
Cervical myelopathy commonly affects walking ability. Patients may notice:
- unsteady gait
- frequent tripping
- difficulty climbing stairs
- balance problems
Coordination Problems
Fine motor control may deteriorate due to disruption of spinal cord signals.
Severe Neurological Symptoms
Advanced cervical myelopathy may cause:
- muscle spasticity
- severe walking difficulty
- bladder or bowel dysfunction
These symptoms require urgent medical evaluation.
Read about : What is Cervical Facet Joint Pain, how it causes cervicogenic headaches and how to correct it naturally
Lesser Known Early Signs of Cervical Myelopathy
Many patients assume cervical myelopathy begins with severe neck pain. In reality, the earliest symptoms are often subtle neurological changes.
Examples include:
- deterioration of handwriting
- hand clumsiness
- difficulty typing
- electric shock sensation when bending the neck forward
- reduced balance in dim lighting
- unexplained arm fatigue
These early symptoms are sometimes mistaken for peripheral nerve disorders or simple muscle fatigue.
Read more: Cervical Vertigo Explained: Why Neck Pain Make You Feel Dizzy
Cervical Myelopathy vs Cervical Radiculopathy
Patients frequently confuse cervical myelopathy with cervical radiculopathy. However the two conditions affect different structures.
Cervical myelopathy involves compression of the spinal cord. Because the spinal cord controls multiple body regions, symptoms may include walking difficulty, balance problems and coordination issues.
Cervical radiculopathy involves compression of a spinal nerve root. This usually causes pain, numbness or weakness along a single nerve distribution in the arm.
Recognizing this difference is essential because cervical myelopathy often requires more urgent medical management. Fehlings et al. (2017)
Read about: Which Is The Best Sitting Posture To Avoid Neck Pain And How To Achieve It
Diagnosis of Cervical Myelopathy
Early diagnosis improves the chances of recovery.
Clinical Examination
Doctors and physiotherapists assess neurological signs such as:
- hyperactive reflexes
- positive Hoffman sign
- positive Babinski reflex
- muscle weakness
- sensory disturbances
These signs suggest spinal cord involvement.
Imaging Tests
Magnetic resonance imaging is the most important investigation because it clearly shows spinal cord compression.
Other diagnostic tests may include:
- cervical spine X rays
- CT scan
- electromyography
These investigations help determine the severity and cause of compression.
Read About: Best Sleeping Position for Neck Pain: A Physiotherapist’s Complete Guide
Physiotherapy Management of Cervical Myelopathy

Physiotherapy plays an important role in both conservative management and postoperative rehabilitation.
The main goals of physiotherapy include:
- improving posture
- maintaining spinal mobility
- strengthening supporting muscles
- improving balance and coordination
- preventing functional decline
Posture Correction
Poor neck posture increases mechanical stress on the cervical spine. Physiotherapists educate patients about maintaining a neutral spine during daily activities.
Cervical Stabilization Exercises
Deep cervical flexor muscles help support the cervical spine. Exercises such as chin tuck training can improve spinal stability.
Scapular Strengthening
Strong scapular muscles help maintain proper neck alignment and reduce cervical strain.
Balance Training
Because cervical myelopathy affects walking stability, balance exercises are often included in rehabilitation programs.
Functional Training
Patients practice activities such as walking, stair climbing and hand coordination exercises to improve daily functioning.
Read about: The Complete Guide to Neck Pain in Yoga Practitioners
Surgical Treatment
Moderate to severe cervical myelopathy often requires surgical decompression of the spinal cord.
The purpose of surgery is to relieve pressure on the spinal cord and prevent further neurological damage.
Common surgical procedures include:
- anterior cervical discectomy and fusion
- cervical laminectomy
- laminoplasty
Clinical guidelines recommend surgery for patients with progressive neurological deficits or significant spinal cord compression. Fehlings et al. (2017)
Read about: What Is Cervical Myofascial Pain Syndrome And How To Relieve Trigger Points
Role of Physiotherapy After Surgery
Postoperative rehabilitation is essential for restoring function after cervical myelopathy surgery.
Physiotherapy programs may include:
- gentle cervical mobility exercises
- strengthening exercises
- gait training
- balance rehabilitation
- functional mobility training
Structured rehabilitation programs have been shown to improve functional recovery and quality of life following spinal cord decompression surgery. Balmaceno Criss et al. (2024)
Read in detail about: How to Fix Upper Crossed Syndrome Naturally
Prognosis and Long Term Outcomes
The prognosis of cervical myelopathy depends on several factors.
Important determinants include:
- severity of spinal cord compression
- duration of symptoms
- patient age
- timing of surgical intervention
Patients who receive early treatment generally experience better neurological recovery compared to those with long standing spinal cord compression.
Delayed treatment may lead to irreversible spinal cord damage. Smith et al. (2025)
Read in detail: Best Desk Setup to Reduce Neck and Back Pain
Best Physiotherapy Exercises for Cervical Myelopathy
Exercise therapy is an important component of cervical myelopathy rehabilitation. While exercises cannot remove spinal cord compression, they help improve spinal stability, muscle strength, balance and overall functional ability.
A structured physiotherapy program can support recovery and prevent further deterioration by improving neuromuscular control and posture. Sharma et al. (2025)
Before beginning any exercise program, patients with cervical myelopathy should consult a physiotherapist or spine specialist to ensure the exercises are appropriate for their condition.
Chin Tuck Exercise
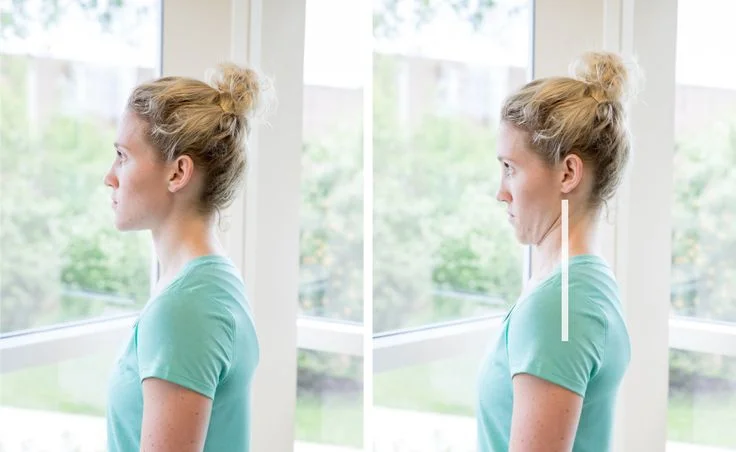
The chin tuck is one of the most effective exercises for activating deep cervical flexor muscles that support the cervical spine.
To perform this exercise:
- Sit or stand with your spine upright
- Gently pull your chin backward without tilting your head
- Hold for five seconds
- Repeat ten times
This exercise improves cervical alignment and reduces forward head posture, which can decrease mechanical stress on the cervical spine.
Learn- How to do Chin Tucks for Neck Pain Relief and Posture Correction
Scapular Retraction Exercise

Strengthening the muscles around the shoulder blades helps maintain proper neck posture.
Steps:
- Sit upright with arms relaxed
- Squeeze your shoulder blades together
- Hold for five seconds
- Repeat ten to fifteen times
Improved scapular stability supports the cervical spine and reduces neck strain.
Balance Training

Because cervical myelopathy often affects walking and coordination, balance exercises are essential during rehabilitation.
Examples include:
- standing on one leg with support
- heel to toe walking
- balance board exercises
Balance training helps retrain the nervous system and reduces fall risk.
Grip Strengthening Exercises

Hand weakness and clumsiness are common symptoms of cervical myelopathy. Strengthening hand muscles can improve functional ability.
Common exercises include:
- squeezing a therapy ball
- finger resistance exercises
- hand putty exercises
These exercises improve grip strength and fine motor coordination.
Gentle Cervical Range of Motion Exercises

Gentle neck mobility exercises can help maintain flexibility and reduce stiffness.
Patients should perform slow and controlled movements such as:
- gentle neck rotation
- side bending
- small range flexion and extension
However, aggressive neck movements should be avoided because excessive motion may increase spinal stress.
Read About: How to Choose the Right and Best Pillow for Neck Pain
Important Safety Considerations
Exercise programs for cervical myelopathy must be carefully supervised. Patients should stop exercising and consult a healthcare professional if they experience:
- worsening numbness
- increasing weakness
- severe neck pain
- dizziness or balance loss
Properly guided rehabilitation programs can improve physical function and quality of life in patients with degenerative cervical myelopathy. Balmaceno Criss et al. (2024)
Read about: Effective Neck Pain Exercises At Home: A Complete Guide to Relief and Improved Mobility
Lifestyle Strategies to Protect the Cervical Spine
Certain lifestyle changes may help reduce cervical spine stress and support recovery.
Maintain Healthy Neck Posture
Avoid prolonged forward head posture while using smartphones or computers.
Take Regular Movement Breaks
Changing posture frequently reduces spinal stress.
Exercise Regularly
Strengthening the neck and shoulder muscles improves spinal stability.
Improve Sleep Ergonomics
Using a supportive pillow helps maintain proper cervical alignment during sleep.
Avoid High Impact Activities
Sudden neck movements or heavy lifting may worsen symptoms.
Read more on : Manual Therapy for Neck Pain: A Physiotherapist’s Evidence Based Guide
When to Seek Medical Help
Consult a healthcare professional if you experience:
- persistent hand numbness
- progressive weakness in arms or legs
- balance problems
- frequent falls
- difficulty performing fine hand movements
Early diagnosis significantly improves treatment outcomes.
Read about: The Most Effective McKenzie Exercises For Neck Pain
Final thoughts
Cervical myelopathy is a serious neurological condition caused by compression of the spinal cord in the neck.
Symptoms often develop gradually and may initially appear mild, but the condition can progress to severe neurological impairment if untreated.
Early recognition, accurate diagnosis and timely treatment are essential for preventing permanent disability.
Physiotherapy plays a crucial role in improving posture, strengthening supportive muscles, restoring mobility and enhancing functional independence.
When necessary, surgical decompression followed by structured rehabilitation can significantly improve quality of life.
Read more: Is Cervical Traction For Neck Pain Really Effective
Frequently Asked Questions About Cervical Myelopathy
1. What is cervical myelopathy?
Cervical myelopathy is a condition in which the spinal cord becomes compressed in the neck region. This compression can interfere with nerve signals and lead to symptoms such as numbness, weakness, poor coordination and difficulty walking.
2. What are the early symptoms of cervical myelopathy?
Early symptoms may include hand numbness, difficulty with fine motor tasks such as buttoning clothes, reduced grip strength, neck stiffness and problems with balance.
3. What causes cervical myelopathy?
The most common cause is degenerative cervical spondylosis, which occurs when age related changes such as disc degeneration, bone spurs and ligament thickening narrow the spinal canal and compress the spinal cord.
4. Is cervical myelopathy a serious condition?
Yes. Cervical myelopathy is considered a serious neurological condition because prolonged spinal cord compression can lead to permanent nerve damage if left untreated.
5. Can physiotherapy help cervical myelopathy?
Physiotherapy can help improve posture, strengthen neck and shoulder muscles, enhance balance and maintain mobility. It is also an important part of rehabilitation after spinal surgery.
6. Does cervical myelopathy always require surgery?
Mild cases may sometimes be managed with conservative treatment such as physiotherapy and lifestyle modifications, but moderate to severe cervical myelopathy often requires surgical decompression.
7. What exercises are recommended for cervical myelopathy?
Exercises such as chin tuck exercises, scapular strengthening, gentle cervical mobility exercises and balance training are commonly used in physiotherapy programs.
8. Can cervical myelopathy be prevented?
Although age related spinal degeneration cannot always be prevented, maintaining good posture, staying physically active and avoiding prolonged neck strain may reduce the risk.
Stay tuned with us for more health related topics.
Follow us on LinkedIn and Instagram for more.
Medical Disclaimer!
This article has been reviewed and written under the guidance of our Head Physiotherapist, Dr. Kruti Raj (PT, MUHS,CPT,CMPT). The information shared is intended for educational purposes only and should not be considered a substitute for personalized medical advice, diagnosis, or treatment.
Please consult us or any other qualified healthcare professional before beginning any exercise program, especially if you are experiencing pain, recovering from injury, or managing a medical condition.











